Nerve-sparing radical hysterectomy compared to standard radical hysterectomy for women with early stage cervical cancer (stage Ia2 to IIa)
- PMID: 30746689
- PMCID: PMC6370917
- DOI: 10.1002/14651858.CD012828.pub2
Nerve-sparing radical hysterectomy compared to standard radical hysterectomy for women with early stage cervical cancer (stage Ia2 to IIa)
Abstract
Background: Radical hysterectomy is one of the standard treatments for stage Ia2 to IIa cervical cancer. Bladder dysfunction caused by disruption of the pelvic autonomic nerves is a common complication following standard radical hysterectomy and can affect quality of life significantly. Nerve-sparing radical hysterectomy is a modified radical hysterectomy, developed to permit resection of oncologically relevant tissues surrounding the cervical lesion, while preserving the pelvic autonomic nerves.
Objectives: To evaluate the benefits and harms of nerve-sparing radical hysterectomy in women with stage Ia2 to IIa cervical cancer.
Search methods: We searched the Cochrane Central Register of Controlled Trials (CENTRAL; 2018, Issue 4), MEDLINE via Ovid (1946 to May week 2, 2018), and Embase via Ovid (1980 to 2018, week 21). We also checked registers of clinical trials, grey literature, reports of conferences, citation lists of included studies, and key textbooks for potentially relevant studies.
Selection criteria: We included randomised controlled trials (RCTs) evaluating the efficacy and safety of nerve-sparing radical hysterectomy compared to standard radical hysterectomy for women with early stage cervical cancer (stage Ia2 to IIa).
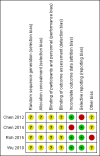
Data collection and analysis: We applied standard Cochrane methodology for data collection and analysis. Two review authors independently selected potentially relevant RCTs, extracted data, evaluated risk of bias of the included studies, compared results and resolved disagreements by discussion or consultation with a third review author, and assessed the certainty of evidence.
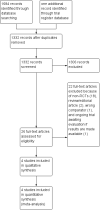
Main results: We identified 1332 records as a result of the search (excluding duplicates). Of the 26 studies that potentially met the review criteria, we included four studies involving 205 women; most of the trials had unclear risks of bias. We identified one ongoing trial.The analysis of overall survival was not feasible, as there were no deaths reported among women allocated to standard radical hysterectomy. However, there were two deaths in among women allocated to the nerve-sparing technique. None of the included studies reported rates of intermittent self-catheterisation over one month following surgery. We could not analyse the relative effect of the two surgical techniques on quality of life due to inconsistent data reported. Nerve-sparing radical hysterectomy reduced postoperative bladder dysfunctions in terms of a shorter time to postvoid residual volume of urine ≤ 50 mL (mean difference (MD) -13.21 days; 95% confidence interval (CI) -24.02 to -2.41; 111 women; 2 studies; low-certainty evidence) and lower volume of postvoid residual urine measured one month following operation (MD -9.59 days; 95% CI -16.28 to -2.90; 58 women; 2 study; low-certainty evidence). There were no clear differences in terms of perioperative complications (RR 0.55; 95% CI 0.24 to 1.26; 180 women; 3 studies; low-certainty evidence) and disease-free survival (HR 0.63; 95% CI 0.00 to 106.95; 86 women; one study; very low-certainty evidence) between the comparison groups.
Authors' conclusions: Nerve-sparing radical hysterectomy may lessen the risk of postoperative bladder dysfunction compared to the standard technique, but the certainty of this evidence is low. The very low-certainty evidence for disease-free survival and lack of information for overall survival indicate that the oncological safety of nerve-sparing radical hysterectomy for women with early stage cervical cancer remains unclear. Further large, high-quality RCTs are required to determine, if clinically meaningful differences of survival exist between these two surgical treatments.
Conflict of interest statement
CK: nothing to declare AA: nothing to declare KG: nothing to declare CN: nothing to declare PL: nothing to declare
Figures




















Update of
- doi: 10.1002/14651858.CD012828
Similar articles
-
Postoperative interventions for preventing bladder dysfunction after radical hysterectomy in women with early-stage cervical cancer.Cochrane Database Syst Rev. 2021 Jan 25;1(1):CD012863. doi: 10.1002/14651858.CD012863.pub2. Cochrane Database Syst Rev. 2021. PMID: 33491176 Free PMC article.
-
Extended-field radiotherapy for locally advanced cervical cancer.Cochrane Database Syst Rev. 2018 Oct 26;10(10):CD012301. doi: 10.1002/14651858.CD012301.pub2. Cochrane Database Syst Rev. 2018. PMID: 30362204 Free PMC article.
-
[Feasibility of unilateral or bilateral nerve-sparing radical hysterectomy in patients with cervical cancer and evaluation of the post-surgery recovery of the bladder and rectal function].Zhonghua Zhong Liu Za Zhi. 2011 Jan;33(1):53-7. Zhonghua Zhong Liu Za Zhi. 2011. PMID: 21575466 Chinese.
-
Efficacy and oncologic safety of nerve-sparing radical hysterectomy for cervical cancer: a randomized controlled trial.J Gynecol Oncol. 2015 Apr;26(2):90-9. doi: 10.3802/jgo.2015.26.2.90. J Gynecol Oncol. 2015. PMID: 25872890 Free PMC article. Clinical Trial.
-
Laparoscopy versus laparotomy for the management of early stage endometrial cancer.Cochrane Database Syst Rev. 2018 Oct 31;10(10):CD006655. doi: 10.1002/14651858.CD006655.pub3. Cochrane Database Syst Rev. 2018. PMID: 30379327 Free PMC article.
Cited by
-
Comparative Outcomes of Laparoscopic Radical Hysterectomy and Nerve-Sparing Technique in Cervical Cancer Patients.JSLS. 2025 Apr-Jun;29(2):e2024.00073. doi: 10.4293/JSLS.2024.00073. Epub 2025 May 13. JSLS. 2025. PMID: 40365089 Free PMC article.
-
Complications of radical hysterectomy with pelvic lymph node dissection for cervical cancer: a 10-year single-centre clinical observational study.BMC Cancer. 2022 Dec 8;22(1):1286. doi: 10.1186/s12885-022-10395-9. BMC Cancer. 2022. PMID: 36476575 Free PMC article.
-
Identification and injury to the inferior hypogastric plexus in nerve-sparing radical hysterectomy.Sci Rep. 2019 Sep 13;9(1):13260. doi: 10.1038/s41598-019-49856-w. Sci Rep. 2019. PMID: 31519975 Free PMC article. Clinical Trial.
-
Nerve-sparing radical hysterectomy in the precision surgery for cervical cancer.J Gynecol Oncol. 2020 May;31(3):e49. doi: 10.3802/jgo.2020.31.e49. Epub 2020 Jan 21. J Gynecol Oncol. 2020. PMID: 32266799 Free PMC article. Review.
-
Preoperative Evaluation of Perineural Invasion in Cervical Cancer: Development and Independent Validation of a Novel Predictive Nomogram.Front Oncol. 2021 Dec 23;11:774459. doi: 10.3389/fonc.2021.774459. eCollection 2021. Front Oncol. 2021. PMID: 35004296 Free PMC article.
References
References to studies included in this review
Chen 2012 {published data only}
-
- Chen C, Li W, Li F, Liu P, Zhou J, Lu L, et al. Classical and nerve‐sparing radical hysterectomy: an evaluation of the nerve trauma in cardinal ligament. Gynecologic Oncology 2012;125(1):245‐51. - PubMed
Chen 2014 {published data only}
-
- Chen L, Zhang WN, Zhang SM, Yang ZH, Zhang P. Effect of laparoscopic nerve‐sparing radical hysterectomy on bladder function, intestinal function recovery and quality of sexual life in patients with cervical carcinoma. Asian Pacific Journal of Cancer Prevention 2014;15(24):10971‐5. - PubMed
Roh 2015 {published data only}
Wu 2010 {published data only}
-
- Wu J, Liu X, Hua K, Hu C, Chen X, Lu X. Effect of nerve‐sparing radical hysterectomy on bladder function recovery and quality of life in patients with cervical carcinoma. International Journal of Gynecological Cancer 2010;20(5):905‐9. - PubMed
References to studies excluded from this review
Barbic 2012 {published data only}
-
- Barbic M, Rakar S, Levicnik A, Stefano AB. Comparison of nerve content in removed parametrial tissue after classic radical hysterectomy and nerve‐sparing radical hysterectomy‐histologic evaluation. European Journal of Gynaecological Oncology 2012;33(1):21‐4. - PubMed
Bogani 2014 {published data only}
-
- Bogani G, Cromi A, Uccella S, Serati M, Casarin J, Pinelli C, et al. Nerve‐sparing versus conventional laparoscopic radical hysterectomy: a minimum 12 months' follow‐up study. International Journal of Gynecological Cancer 2014;24(4):787‐93. - PubMed
Ceccaroni 2010 {published data only}
-
- Ceccaroni M, Pontrelli G, Spagnolo E, Scioscia M, Bruni F, Paglia A, et al. Parametrial dissection during laparoscopic nerve‐sparing radical hysterectomy: a new approach aims to improve patients' postoperative quality of life. American Journal of Obstetrics and Gynecology 2010;202(3):320.e1‐2. - PubMed
Ceccaroni 2012 {published data only}
-
- Ceccaroni M, Roviglione G, Spagnolo E, Casadio P, Clarizia R, Peiretti M, et al. Pelvic dysfunctions and quality of life after nerve‐sparing radical hysterectomy: a multicenter comparative study. Anticancer Research 2012;32(2):581‐8. - PubMed
Charoenkwan 2010 {published data only}
-
- Charoenkwan K. A simplified technique for nerve‐sparing type III radical hysterectomy: by reorganizing their surgical sequence, surgeons could more easily identify key nerves. American Journal of Obstetrics and Gynecology 2010;203(6):600.e1‐6. - PubMed
Cibula 2010 {published data only}
-
- Cibula D, Velechovska P, Slama J, Fischerova D, Pinkavova I, Pavlista D, et al. Late morbidity following nerve‐sparing radical hysterectomy. Gynecologic Oncology 2010;116(3):506‐11. - PubMed
Ditto 2009 {published data only}
-
- Ditto A, Martinelli F, Borreani C, Kusamura S, Hanozet F, Brunelli C, et al. Quality of life and sexual, bladder, and intestinal dysfunctions after class III nerve‐sparing and class II radical hysterectomies: a questionnaire‐based study. International Journal of Gynecological Cancer 2009;19(5):953‐7. - PubMed
Hockel 2000 {published data only}
-
- Hockel M, Naumann G, Alexander H, Horn LC, Fischer U, Schmidt F, et al. Nerve‐sparing radical hysterectomy: iI. Results after three years. Geburtshilfe und Frauenheilkunde 2000;60(6):320‐5.
Kanao 2014 {published data only}
Kim 2017 {published data only}
-
- Kim HS, Kim M, Luo Y, Lee M, Song YS. Favorable factors for preserving bladder function after nerve‐sparing radical hysterectomy: a protocol‐based validation study. Journal of Surgical Oncology 2017;116(4):492‐9. - PubMed
Milani 1991 {published data only}
-
- Milani R, Maggioni A, Scalambrino S, Landoni F, Caruso O, Mangioni C. Bladder function following randomization to two different radical hysterectomy procedures: A prospective study. International Urogynecology Journal 1991;2(2):77‐8.
Querleu 2002 {published data only}
-
- Querleu D, Narducci F, Poulard V, Lacaze S, Occelli B, Leblanc E, et al. Modified radical vaginal hysterectomy with or without laparoscopic nerve‐sparing dissection: a comparative study. Gynecologic Oncology 2002;85(1):154‐8. - PubMed
Raspagliesi 2006 {published data only}
-
- Raspagliesi F, Ditto A, Fontanelli R, Zanaboni F, Solima E, Spatti G, et al. Type II versus Type III nerve‐sparing radical hysterectomy: comparison of lower urinary tract dysfunctions. Gynecologic Oncology 2006;102(2):256‐62. - PubMed
Raspagliesi 2017 {published data only}
-
- Raspagliesi F, Bogani G, Spinillo A, Ditto A, Bogliolo S, Casarin J, et al. Introducing nerve‐sparing approach during minimally invasive radical hysterectomy for locally‐advanced cervical cancer: a multi‐institutional experience. European Journal of Surgical Oncology 2017;43(11):2150‐6. - PubMed
Sakuragi 2015 {published data only}
Shi 2016 {published data only}
-
- Shi R, Wei W, Jiang P. Laparoscopic nerve‐sparing radical hysterectomy for cervical carcinoma: emphasis on nerve content in removed cardinal ligaments. International Journal of Gynecological Cancer 2016;26(1):192‐8. - PubMed
Skret‐Magierlo 2010 {published data only}
-
- Skret‐Magierlo J, Narog M, Kruczek A, Kluza R, Kluz T, Magon T, et al. Radical hysterectomy during the transition period from traditional to nerve‐sparing technique. Gynecologic Oncology 2010;116(3):502‐5. - PubMed
Su 2017 {published data only}
-
- Su Y, Zhang M, Zhang W, Shi H. Application research on nerve sparing radical hysterectomy for rectal function. Pakistan Journal of Pharmaceutical Sciences 2017;30(1 Suppl):329‐34. - PubMed
Todo 2006 {published data only}
-
- Todo Y, Kuwabara M, Watari H, Ebina Y, Takeda M, Kudo M, et al. Urodynamic study on postsurgical bladder function in cervical cancer treated with systematic nerve‐sparing radical hysterectomy. International Journal of Gynecological Cancer 2006;16(1):369‐75. - PubMed
Tseng 2012 {published data only}
-
- Tseng CJ, Shen HP, Lin YH, Lee CY, Wei‐Cheng Chiu W. A prospective study of nerve‐sparing radical hysterectomy for uterine cervical carcinoma in Taiwan. Taiwanese Journal of Obstetrics and Gynecology 2012;51(1):55‐9. - PubMed
Yang 2016 {published data only}
-
- Yang Y, Qin T, Zhang W, Wu Q, Yang A, Xu F. Laparoscopic nerve‐sparing radical hysterectomy for bulky cervical cancer (>6 cm) after neoadjuvant chemotherapy: a multicenter prospective cohort study. International Journal of Surgery 2016;34:35‐40. - PubMed
References to ongoing studies
Gaballa 2015 {unpublished data only}
-
- Feasibility and functional outcome of laparoscopic nerve sparing radical hysterectomy (NCT02524756). Ongoing study November 2014.
Additional references
Aoun 2015
-
- Aoun F, Albisinni S, Peltier A, Maoula A, Velthoven R, Roumeguère T. Lower urinary tract dysfunction following nerve sparing radical hysterectomy: A systematic review. Progress in Urology 2015;S1166‐7087(15):690‐9. - PubMed
Barry 1992
-
- Barry MJ, Fowler FJ Jr, O'Leary MP, Bruskewitz RC, Holtgrewe HL, Mebust WK, et al. The American Urological Association symptom index for benign prostatic hyperplasia. The measurement committee of the American Urological Association. Journal of Urology 1992;148(5):1549‐57. - PubMed
Basaran 2015
-
- Basaran D, Dusek L, Majek O, Cibula D. Oncological outcomes of nerve‐sparing radical hysterectomy for cervical cancer: a systematic review. Annals of Surgical Oncology 2015;22(9):3033‐40. - PubMed
Butler‐Manuel 2000
-
- Butler‐Manuel SA, Buttery LD, A'Hern RP, Polak JM, Barton DP. Pelvic nerve plexus trauma at radical hysterectomy and simple hysterectomy: the nerve content of the uterine supporting ligaments. Cancer 2000;89(4):834‐41. - PubMed
Charoenkwan 2006
-
- Charoenkwan K, Srisomboon J, Suprasert P, Tantipalakorn C, Kietpeerakool C. Nerve‐sparing class III radical hysterectomy: a modified technique to spare the pelvic autonomic nerves without compromising radicality. International Journal of Gynecological Cancer 2006;16(4):1705‐12. - PubMed
Cherny 2015
-
- Cherny NI, Sullivan R, Dafni U, Kerst JM, Sobrero A, Zielinski C, et al. A standardised, generic, validated approach to stratify the magnitude of clinical benefit that can be anticipated from anti‐cancer therapies: the European Society for Medical Oncology Magnitude of Clinical Benefit Scale (ESMO‐MCBS). Annals of Oncology 2015;26(8):1547‐73. - PubMed
Chong 2013
-
- Chong GO, Lee YH, Hong DG, Cho YL, Park IS, Lee YS. Robot versus laparoscopic nerve‐sparing radical hysterectomy for cervical cancer: a comparison of the intraoperative and perioperative results of a single surgeon's initial experience. International Journal of Gynecological Cancer 2013;23(6):1145‐9. - PubMed
Cibula 2011
-
- Cibula D, Abu‐Rustum NR, Benedetti‐Panici P, Köhler C, Raspagliesi F, Querleu D, et al. New classification system of radical hysterectomy: emphasis on a three‐dimensional anatomic template for parametrial resection. Gynecologic Oncology 2011;122(2):264‐8. - PubMed
Covidence [Computer program]
-
- Veritas Health Innovation. Covidence. Version accessed 27 September 2017. Melbourne, Australia: Veritas Health Innovation, 2017.
CTCAE 2010
-
- NCI. Common Terminology Criteria for Adverse Events v4.03. National Institutes of Health, US Department of Health and Human Services (accessed 27 September 2017); Vol. publication 09‐7473.
Deeks 2001
-
- Deeks J, Altman D, Bradburn M. Statistical methods for examining heterogeneity and combining results from several studies in meta‐analysis. In: Egger M, Davey Smith G, Altman DG editor(s). Systematic Reviews in Health Care: Meta‐Analysis in Context. 2nd Edition. London (UK): BMJ Publication Group, 2001:285–312.
DeSimonian 1986
-
- DerSimonian R, Laird N. Meta‐analysis in clinical trials. Controlled Clinical Trials 1986;7(3):177‐88. - PubMed
EndNote [Computer program]
-
- Thomas Reuters. EndNote. Version x7. New York: Thomas Reuters, 2015.
Ercoli 2003
-
- Ercoli A, Delmas V, Gadonneix P, Fanfani F, Villet R, Paparella P, et al. Classical and nerve‐sparing radical hysterectomy: an evaluation of the risk of injury to the autonomous pelvic nerves. Surgical and Radiologic Anatomy 2003;25(3‐4):200‐6. - PubMed
Ferlay 2015
-
- Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. International Journal of Cancer 2015;136(5):E359‐86. - PubMed
FIGO Committee 2014
-
- FIGO Committee on Gynecologic Oncology. FIGO staging for carcinoma of the vulva, cervix, and corpus uteri. International Journal of Gynaecology & Obstetrics 2014;125(2):97‐8. - PubMed
Fujii 2007
-
- Fujii S, Takakura K, Matsumura N, Higuchi T, Yura S, Mandai M, et al. Anatomic identification and functional outcomes of the nerve sparing Okabayashi radical hysterectomy. Gynecologic Oncology 2007;107(1):4‐13. - PubMed
Fujii 2008
-
- Fujii S. Anatomic identification of nerve‐sparing radical hysterectomy: a step‐by‐step procedure. Gynecologic Oncology 2008;111(2 Suppl):S33‐41. - PubMed
Gotay 2002
-
- Gotay CC, Holup JL, Pagano I. Ethnic differences in quality of life among early breast and prostate cancer survivors. Psychooncology 2002;11(2):103‐13. - PubMed
GRADEpro GDT [Computer program]
-
- McMaster University (developed by Evidence Prime). GRADEpro GDT. Version accessed 27 September 2017. Hamilton (ON): McMaster University (developed by Evidence Prime), 2015.
Greimel 2006
-
- Greimel ER, Kuljanic Vlasic K, Waldenstrom AC, Duric VM, Jensen PT, Singer S, et al. The European Organization for Research and Treatment of Cancer (EORTC) Quality‐of‐Life questionnaire cervical cancer module: EORTC QLQ‐CX24. Cancer 2006;107(8):1812‐22. - PubMed
Heinemann 2016
-
- Heinemann J, Atallah S, Rosenbaum T. The impact of culture and ethnicity on sexuality and sexual function. Current Sexual Health Reports 2016;8(3):144‐50.
Higgins 2011
-
- Higgins JP, Green S, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from handbook.cochrane.org.
Hongladaromp 2014
-
- Hongladaromp W, Tantipalakorn C, Charoenkwan K, Srisomboon J. Locoregional spread and survival of stage IIA1 versus stage IIA2 cervical cancer. Asian Pacific Journal of Cancer Prevention 2014;15(2):887‐90. - PubMed
Huber 2015
-
- Huber SA, Northington GM, Karp DR. Bowel and bladder dysfunction following surgery within the presacral space: an overview of neuroanatomy, function, and dysfunction. International Urogynecology Journal 2015;26(7):941‐6. - PubMed
IntHout 2015
-
- IntHout J, Ioannidis JP, Borm GF, Goeman JJ. Small studies are more heterogeneous than large ones: a meta‐meta‐analysis. Journal of Clinical Epidemiology 2015;68(8):860‐9. - PubMed
Jensen 2004
-
- Jensen PT, Klee MC, Thranov I, Groenvold M. Validation of a questionnaire for self‐assessment of sexual function and vaginal changes after gynaecological cancer. Psycho‐oncology 2004;13(8):577‐92. - PubMed
Katepratoom 2014
-
- Katepratoom C, Manchana T, Amornwichet N. Lower urinary tract dysfunction and quality of life in cervical cancer survivors after concurrent chemoradiation versus radical hysterectomy. International Urogynecology Journal 2014;25(1):91‐6. - PubMed
Kato 2003
-
- Kato T, Murakami G, Yabuki Y. A new perspective on nerve‐sparing radical hysterectomy: nerve topography and over‐preservation of the cardinal ligament. Japanese Journal of Clinical Oncology 2003;33(11):589‐91. - PubMed
Kim 2000
-
- Kim SM, Choi HS, Byun JS. Overall 5‐year survival rate and prognostic factors in patients with stage IB and IIA cervical cancer treated by radical hysterectomy and pelvic lymph node dissection. International Journal of Gynecologic Cancer 2000;10(4):305–12. - PubMed
Kim 2015a
-
- Kim HS, Kim TH, Suh DH, Kim SY, Kim MA, Jeong CW, et al. Success factors of laparoscopic nerve‐sparing radical hysterectomy for preserving bladder function in patients with cervical cancer: a protocol‐based prospective cohort study. Annals of Surgical Oncology 2015;22(6):1987‐95. - PubMed
Kim 2015b
Kyo 2016
-
- Kyo S, Kato T, Nakayama K. Current concepts and practical techniques of nerve‐sparing laparoscopic radical hysterectomy. European Journal of Obstetrics & Gynecology and Reproductive Biology 2016;207:80‐8. - PubMed
Langendam 2013
Laterza 2015
-
- Laterza RM, Sievert KD, Ridder D, Vierhout ME, Haab F, Cardozo L, et al. Bladder function after radical hysterectomy for cervical cancer. Neurourology and Urodynamics 2015;34(4):309‐15. - PubMed
Liberati 2009
Long 2014
Maas 2005
-
- Maas CP, Kenter GG, Trimbos JB, Deruiter MC. Anatomical basis for nerve‐sparing radical hysterectomy: immunohistochemical study of the pelvic autonomic nerves. Acta Obstetricia et Gynecologica Scandinavica 2005;84(9):868‐74. - PubMed
Mahawerawat 2013
-
- Mahawerawat S, Charoenkwan K, Srisomboon J, Khunamornpong S, Suprasert P, Sae‐Teng CT. Surgical outcomes of patients with stage IA2 cervical cancer treated with radical hysterectomy. Asian Pacific Journal of Cancer Prevention 2013;14(9):5375–8. - PubMed
Manchana 2009
-
- Manchana T, Sirisabya N, Lertkhachonsuk R, Worasethsin P, Khemapech N, Sittisomwong T, et al. Long term complications after radical hysterectomy with pelvic lymphadenectomy. Journal of the Medical Association of Thailand 2009;92(4):451‐6. - PubMed
Mantzaris 2008
-
- Mantzaris G, Rodolakis A, Vlachos G, Athanasiou S, Theocharis S, Sotiripoulou ChM, et al. Magnifying lenses assisted nerve‐sparing radical hysterectomy and prevention of nerve plexus trauma. International Journal of Gynecological Cancer 2008;18(4):868‐75. - PubMed
Marin 2014
Maserejian 2014
Mota 2008
-
- Mota F, Vergote I, Trimbos JB, Amant F, Siddiqui N, Rio A, et al. Classification of radical hysterectomy adopted by the Gynecological Cancer Group of the European Organization for Research and Treatment of Cancer. International Journal of Gynecological Cancer 2008;18(5):1136‐8. - PubMed
Park 2016 [pers comm]
-
- Park SY. Asking some information of published article. Email to: parksang@ncc.re.kr 29 October 2016.
Park 2017
-
- Park DA, Yun JE, Kim SW, Lee SH. Surgical and clinical safety and effectiveness of robot‐assisted laparoscopic hysterectomy compared to conventional laparoscopy and laparotomy for cervical cancer: A systematic review and meta‐analysis. European Journal of Surgical Oncology 2017;43(6):994‐1002. - PubMed
Parkin 2014
-
- Parkin DM, Bray F, Ferlay J, Jemal A. Cancer in Africa 2012. Cancer Epidemiology, Biomarkers & Prevention 2014;23(6):953‐66. - PubMed
Parmar 1998
-
- Parmar MK, Torri V, Stewart L. Extracting summary statistics to perform meta‐analyses of the published literature for survival endpoints. Statistics in Medicine 1998;17(24):2815‐34. - PubMed
Piver 1974
-
- Piver MS, Rutledge F, Smith JP. Five classes of extended hysterectomy for women with cervical cancer. Obstetrics & Gynecology 1974;44(2):265‐72. - PubMed
Plotti 2011
-
- Plotti F, Angioli R, Zullo MA, Sansone M, Altavilla T, Antonelli E, et al. Update on urodynamic bladder dysfunctions after radical hysterectomy for cervical cancer. Critical Reviews in Oncology/Hematology 2011;80(2):323‐9. - PubMed
Querleu 2008
-
- Querleu D, Morrow CP. Classification of radical hysterectomy. Lancet Oncology 2008;9(3):297‐303. - PubMed
Ramirez 2018
-
- Ramireza PT, Frumovitza M, Parejab R, Lopezc A, Vieirad MA, Ribeiro R. Phase III randomized trial of laparoscopic or robotic versus abdominal radical hysterectomy in patients with early‐stage cervical cancer: LACC trial. 2018 Society of Gynecologic Oncology Annual Meeting on Women’s Cancer. LBA1. Presented March 26, 2018.
Review Manager 2014 [Computer program]
-
- Nordic Cochrane Centre, The Cochrane Collaboration. Review Manager 5 (RevMan 5). Version 5.3. Copenhagen: Nordic Cochrane Centre, The Cochrane Collaboration, 2014.
Schünemann 2011
-
- Schünemann HJ, Oxman AD, Higgins JP, Vist GE, Glasziou P, Guyatt GH. Chapter 11: Presenting results and ‘Summary of findings' tables. In: Higgins JP, Green S, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from handbook.cochrane.org.
Schünemann 2013
-
- Schünemann HJ, Tugwell P, Reeves BC, Akl EA, Santesso N, Spencer FA, et al. Non‐randomized studies as a source of complementary, sequential or replacement evidence for randomized controlled trials in systematic reviews on the effects of interventions. Research Synthesis Methods 2013;4(1):49‐62. - PubMed
Spirtos 2002
-
- Spirtos NM, Eisenkop SM, Schlaerth JB, Ballon SC. Laparoscopic radical hysterectomy (type III) with aortic and pelvic lymphadenectomy in patients with stage I cervical cancer: surgical morbidity and intermediate follow‐up. American Journal of Obstetrics and Gynecology 2002;187(2):340‐8. - PubMed
Srisomboon 2011
-
- Srisomboon J, Kietpeerakool C, Suprasert P, Manopanya M, Siriaree S, Charoenkwan K, et al. Survival and prognostic factors comparing stage IB 1 versus stage IB 2 cervical cancer treated with primary radical hysterectomy. Asian Pacific Journal of Cancer Prevention 2011;12(7):1753–6. - PubMed
Sterne 2011
-
- Sterne J, Sutton A, Loannidis J, Terrin N, Jones D, Lau J, et al. Recommendations for examining and interpreting funnel plot asymmetry in meta‐analyses of randomised controlled trials. BMJ 2011;343:d4002. - PubMed
Suprasert 2010
-
- Suprasert P, Srisomboon J, Charoenkwan K, Siriaree S, Cheewakriangkrai C, Kietpeerakool C, et al. Twelve years experience with radical hysterectomy and pelvic lymphadenectomy in early stage cervical cancer. Journal of Obstetrics and Gynaecology 2010;30(3):294–8. - PubMed
Vale 2010
van Gent 2016
-
- Gent MD, Romijn LM, Santen KE, Trimbos JB, Kroon CD. Nerve‐sparing radical hysterectomy versus conventional radical hysterectomy in early‐stage cervical cancer. A systematic review and meta‐analysis of survival and quality of life. Maturitas 2016;94:30‐8. - PubMed
Verleye 2009
-
- Verleye L, Vergote I, Reed N, Ottevanger PB. Quality assurance for radical hysterectomy for cervical cancer: the view of the European Organization for Research and Treatment of Cancer‐Gynecological Cancer Group (EORTC‐GCG). Annals of Oncology 2009;20(10):1631‐8. - PubMed
von Hippel 2015
Wan 2014
Webster 2003
Xue 2016
-
- Xue Z, Zhu X, Teng Y. Comparison of nerve‐sparing radical hysterectomy and radical hysterectomy: a systematic review and meta‐analysis. Cellular Physiology and Biochemistry 2016;38(5):1841‐50. - PubMed
References to other published versions of this review
Kietpeerakool 2017
-
- Kietpeerakool C, Aue‐aungkul A, Galaal K, Ngamjarus C, Lumbiganon P. Nerve‐sparing radical hysterectomy compared to standard radical hysterectomy for women with early stage cervical cancer (stage Ia2 to IIa). Cochrane Database of Systematic Reviews 2017, Issue 10. [DOI: 10.1002/14651858.CD012828] - DOI - PMC - PubMed

