The use of arthrocentesis in patients with temporomandibular joint disc displacement without reduction
- PMID: 30759144
- PMCID: PMC6374052
- DOI: 10.1371/journal.pone.0212307
The use of arthrocentesis in patients with temporomandibular joint disc displacement without reduction
Abstract
The aim of this study was to evaluate the efficacy of the use of the arthrocentesis in patients with disc displacement without reduction (DDWOR). Two hundred and thirty-four (234) patients with DDWOR were evaluated and the following data collected: gender; affected side; age (years); duration of the pain (months); patient's perception of pain (measured by Visual Analogue Scale [VAS 0-10]); maximal interincisal distance (MID) (mm); and joint disc position, determined by magnetic resonance imaging. Data were obtained in two different moments: before the arthrocentesis (M1) and three or four months later (M2). Paired t-Student Test, Scores Test and Wilcoxon Test showed a statistical significant difference (p<0.0001) between the M1 and M2 for the variables VAS and MID. There was an alteration in the joint disc position in 93.88% of the cases after arthrocentesis. There was no association between the general characteristics of the patients on the M1 and the results of the arthrocentesis (p>0.05). It can be concluded that the arthrocentesis is efficient in reducing the pain, in increasing interincisal distance, and altering the joint disc position in patients with DDWOR regardless gender, age side and pain duration.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
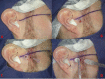
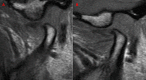
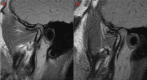
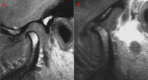
Similar articles
-
Double puncture versus single puncture arthrocentesis for the management of unilateral temporomandibular joint disc displacement without reduction: A randomized controlled trial.J Craniomaxillofac Surg. 2018 Dec;46(12):2003-2007. doi: 10.1016/j.jcms.2018.10.015. Epub 2018 Oct 26. J Craniomaxillofac Surg. 2018. PMID: 30446325 Clinical Trial.
-
Can protrusive movements during TMJ arthrocentesis improve final results?J Craniomaxillofac Surg. 2025 May;53(5):454-458. doi: 10.1016/j.jcms.2025.01.020. Epub 2025 Jan 24. J Craniomaxillofac Surg. 2025. PMID: 39855983 Clinical Trial.
-
The benefits of performing temporomandibular joint arthrocentesis with catheters and a vacuum pump: A randomized control trial.J Craniomaxillofac Surg. 2024 Mar;52(3):369-373. doi: 10.1016/j.jcms.2024.01.020. Epub 2024 Jan 17. J Craniomaxillofac Surg. 2024. PMID: 38253472 Clinical Trial.
-
Temporomandibular joint arthrocententesis: evaluation of results and review of the literature.Braz J Otorhinolaryngol. 2006 Sep-Oct;72(5):634-8. doi: 10.1016/s1808-8694(15)31019-3. Braz J Otorhinolaryngol. 2006. PMID: 17221055 Free PMC article. Review.
-
Temporomandibular Disorders: Surgical Implications and Management.Dent Clin North Am. 2023 Apr;67(2):349-365. doi: 10.1016/j.cden.2022.12.002. Dent Clin North Am. 2023. PMID: 36965936 Review.
Cited by
-
A Bibliometric Analysis of Research on Temporomandibular Joint Disc Displacement from 1992 to 2022.Healthcare (Basel). 2023 Jul 24;11(14):2108. doi: 10.3390/healthcare11142108. Healthcare (Basel). 2023. PMID: 37510548 Free PMC article. Review.
-
State of the Art in Temporomandibular Joint Arthrocentesis-A Systematic Review.J Clin Med. 2023 Jun 30;12(13):4439. doi: 10.3390/jcm12134439. J Clin Med. 2023. PMID: 37445474 Free PMC article. Review.
-
Double-Puncture Versus Single-Puncture Arthrocentesis: A Randomized Controlled Trial with 3 Years of Follow-Up.J Oral Facial Pain Headache. 2022 Spring;36(2):141-146. doi: 10.11607/ofph.3074. J Oral Facial Pain Headache. 2022. PMID: 35943324 Free PMC article. Clinical Trial.
-
Is arthrocentesis effective for temporomandibular joint disorders?Acta Cir Bras. 2025 Aug 8;40:e406425. doi: 10.1590/acb406425. eCollection 2025. Acta Cir Bras. 2025. PMID: 40802355 Free PMC article. Review.
References
-
- Lazarin RD, Previdelli IT, Silva RD, Iwaki LC, Grossmann E, Filho LI. Correlation of gender and age with magnetic resonance imaging findings in patients with arthrogenic temporomandibular disorders: a cross-sectional study. Int J Oral Maxillofac Surg. 2016; 45:1222–1228. 10.1016/j.ijom.2016.04.016 - DOI - PubMed
-
- Dworkin SF, Leresche L. Research diagnostic criteria for temporomandibular disorders: review criteria, examinations and specifications, critique. J Craniomandib Disord. 1992;6(4):301–350. - PubMed
-
- Ahmad M, Hollender L, Anderson Q, Kartha K, Ohrbach R, Truelove EL, et al. Research diagnostic criteria for temporomandibular disorders (RDC/TMD): development of image analysis criteria and examiner reliability for image analysis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009; 107:844–60. 10.1016/j.tripleo.2009.02.023 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

