Comparing the Changes in Blood Pressure After Acute Exposure to Tai Chi and Walking
- PMID: 30761199
- PMCID: PMC6355127
- DOI: 10.70252/AAUX3960
Comparing the Changes in Blood Pressure After Acute Exposure to Tai Chi and Walking
Abstract
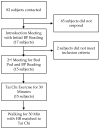
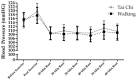
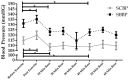
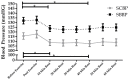
Hypertension is a major health concern throughout the United States and is a major cause of cardiovascular disease. The purpose of this study was to compare the responses of Tai Chi and walking on measures of central and peripheral cardiac mechanisms when controlling for exercise intensity. Fifteen hypertensive subjects (2 males, 13 females; age = 20.7 ± 3.77 years; body fat = 24.26 ± 10.27%) participated in Tai Chi (TC) and walking (WK) for 30 minutes on non-consecutive days. Central systolic (CSBP) and diastolic blood pressure (CDBP), augmentation index (Alx), pulse pressure (PP), heart rate (HR), and brachial systolic (BSBP) and diastolic blood pressure (BDBP) were measured prior to exercise and following exercise every 10 minutes for a total of 60 minutes in a seated position. There were no significant differences between the two exercise forms. CSBP decreased 10 minutes after exercise in both exercise types (TC = 6.63 ± 3.258 mmHG; WK = 7 ± 4.144 mmHG p < 0.05), and 40 minutes after exercise in both exercise types (TC = 6.07 ± 3.33 mmHG; WK = 8.2 ± 3.15 mmHG, p < 0.05) compared to the initial measurement. BSBP also decreased in both exercise forms following 10 min of rest (TC = 6.99 ± 3.776 mmHG; WK = 8.8 ± 3.20 mmHG p = 0.05), and 40 min (TC = 8.46 ± 3.07 mmHG; WK = 8.87 ± 3.87 mmHG, p < 0.05) when compared to the initial resting measurement. Central aortic pressure exhibits a post exercise hypotensive (PEH) effect similar to that of peripheral blood pressure. Both Tai Chi and walking elicited similar PEH effects on systolic blood pressure in hypertensive individuals.
Keywords: Exercise; acute; hemodynamics.
Figures
Similar articles
-
Caffeine ingestion alters central hemodynamics following aerobic exercise in middle-aged men.Eur J Appl Physiol. 2021 Feb;121(2):435-443. doi: 10.1007/s00421-020-04521-3. Epub 2020 Oct 24. Eur J Appl Physiol. 2021. PMID: 33098463 Clinical Trial.
-
Tai Chi exercise is more effective than brisk walking in reducing cardiovascular disease risk factors among adults with hypertension: A randomised controlled trial.Int J Nurs Stud. 2018 Dec;88:44-52. doi: 10.1016/j.ijnurstu.2018.08.009. Epub 2018 Aug 24. Int J Nurs Stud. 2018. PMID: 30195124 Clinical Trial.
-
Resistance exercise lowers blood pressure and improves vascular endothelial function in individuals with elevated blood pressure or stage-1 hypertension.Am J Physiol Heart Circ Physiol. 2024 Jan 1;326(1):H256-H269. doi: 10.1152/ajpheart.00386.2023. Epub 2023 Nov 17. Am J Physiol Heart Circ Physiol. 2024. PMID: 37975709 Free PMC article. Clinical Trial.
-
Response variation as a result of tai chi on resting blood pressure in hypertensive adults: An aggregate data meta-analysis.Complement Ther Clin Pract. 2022 Nov;49:101641. doi: 10.1016/j.ctcp.2022.101641. Epub 2022 Jul 18. Complement Ther Clin Pract. 2022. PMID: 35870250 Review.
-
Effects of the different Tai Chi exercise cycles on patients with essential hypertension: A systematic review and meta-analysis.Front Cardiovasc Med. 2023 Mar 3;10:1016629. doi: 10.3389/fcvm.2023.1016629. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 36937925 Free PMC article. Review.
Cited by
-
Effects of Tai Chi on the Executive Function and Physical Fitness of Female Methamphetamine Dependents: A Randomized Controlled Trial.Front Psychiatry. 2021 Jun 10;12:653229. doi: 10.3389/fpsyt.2021.653229. eCollection 2021. Front Psychiatry. 2021. PMID: 34177646 Free PMC article.
-
Effects of Tai Chi and Qigong intervention on anxiety and stress in diabetic and hypertensive Brazilian patients: a randomized controlled trial.Einstein (Sao Paulo). 2025 Mar 24;23:eAO1076. doi: 10.31744/einstein_journal/2025AO1076. eCollection 2025. Einstein (Sao Paulo). 2025. PMID: 40353827 Free PMC article. Clinical Trial.
References
-
- American College of Sports Medicine. Living with hypertension. Oct 7, 2016. Updated on October 7, 2016. Retrieved on August 1, 2017.
-
- Center for Disease Control. High blood pressure. Updated March 3, 2017. Retrieved on August 1, 2017.
-
- Chobanian AV, Bakris GL, Black HR. The seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2013;28(9):25–60. - PubMed
-
- Cléroux J, Kouamé N, Nadeau A, Coulombe D, Lacourcière Y. Aftereffects of exercise on regional and systemic hemodynamics in hypertension. Hypertension. 1992;19(2):183–91. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous
