Central Venous Stenosis, Access Outcome and Survival in Patients undergoing Maintenance Hemodialysis
- PMID: 30765534
- PMCID: PMC6419278
- DOI: 10.2215/CJN.07010618
Central Venous Stenosis, Access Outcome and Survival in Patients undergoing Maintenance Hemodialysis
Abstract
Background and objectives: Central venous catheters have traditionally provided access for urgent hemodialysis, but are also sometimes advocated as an option for older or more comorbid patients. Adverse effects of this type of dialysis access include central venous stenosis, for which the risk factors and consequences are incompletely understood.
Design, setting, participants, & measurements: We conducted two studies within the same population cohort, comprising all patients starting hemodialysis in a single center from January 2006 to December 2013. First, patients were retrospectively analyzed for the presence of central venous stenosis; their access outcomes are described and survival compared with matched controls drawn from the same population. Second, a subset of patients with a history of catheter access within this cohort was analyzed to determine risk factors for central venous stenosis.
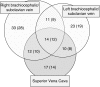
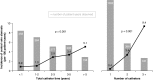
Results: Among 2811 patients, central venous stenosis was diagnosed in 120 (4.3%), at a median dialysis vintage of 2.9 (interquartile range, 1.8-4.6) years. Compared with matched controls, patients with central venous stenosis had similar survival (median 5.1 versus 5.2 years; P=0.54). Among a subset of 500 patients, all with a history of catheter use, 34 (6.8%) developed central venous stenosis, at a rate of 2.2 per 100 patient-years. The incidence of central venous stenosis was higher with larger number of previous catheters (relative risk [RR], 2.2; 95% confidence interval [95% CI]. 1.6 to 2.9), pacemaker insertion (RR, 3.9; 95% CI, 1.7 to 8.9), and was lower with older age (RR, 0.7 per decade; 95% CI, 0.6 to 0.8). In a Cox proportional hazards model, the catheter number, pacemaker, and younger age at dialysis initiation were all significant independent risk factors for central venous stenosis.
Conclusions: Central venous stenosis occurred in a minority of patients on hemodialysis, and was associated with compromised future access, but unchanged survival. Among patients with a history of catheter use, risk related to both the number of catheters and the total catheter duration, although nondialysis factors such as pacemakers were also important. Central venous stenosis risk was lower in older patients, supporting the selective use of tunneled catheters in this group.
Keywords: Artificial; Catheterization; Central Venous Catheter; Central Venous Stenosis; Cohort Studies; Constriction; Incidence; Pacemaker; Pathologic; Proportional Hazards Models; Retrospective Studies; Tunneled Dialysis Catheter; arteriovenous fistula; dialysis; hemodialysis; risk factors.
Copyright © 2019 by the American Society of Nephrology.
Figures



References
-
- Aitken E, Jackson AJ, Kasthuri R, Kingsmore DB: Bilateral central vein stenosis: Options for dialysis access and renal replacement therapy when all upper extremity access possibilities have been lost. J Vasc Access 15: 466–473, 2014 - PubMed
-
- Sabet B, Soltani S, Mafi AA, Yaghmaie S, Ghorbani R, Keramati A: Survey of factors that affect the arteriovenous fistulas survival in Semnan and Mahdishahr, Iran. Acad J Surg 2: 15–18, 2015
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

