Economic burden of lung cancer: A retrospective cohort study in South Korea, 2002-2015
- PMID: 30794674
- PMCID: PMC6386401
- DOI: 10.1371/journal.pone.0212878
Economic burden of lung cancer: A retrospective cohort study in South Korea, 2002-2015
Abstract
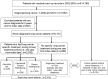
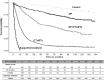
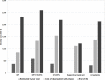
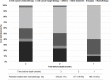
We evaluated the survival rates and medical expenditure in patients with lung cancer using a nationwide claims database in South Korea. A retrospective observational cohort study design was used, and 2,919 lung cancer patients and their matched controls were included. Medical expenditures were analyzed with the Kaplan-Meier sample average method, and patients were categorized into 4 groups by operation and primary treatment method (i.e. Patients with operation: OP = surgery, OP+CTx/RTx = surgery with anti-cancer drugs or radiotherapy; Patients without operation: CTx/RTx = anti-cancer drugs or radiotherapy, Supportive treatment). The 5-year medical expenditure per case was highest in the OP+CTx/RTx group ($36,013), followed by the CTx/RTx ($23,134), OP ($22,686), and supportive treatment group ($3,700). Lung cancer-related anti-cancer drug therapy was the major cost driver, with an average 53% share across all patients. Generalized linear regression revealed that monthly medical expenditure in lung cancer patients, after adjustment for follow-up month, was approximately 3.1-4.3 times higher than that in the control group (cost ratio for OP = 3.116, OP+CTx/RTx = 3.566, CTx/RTx = 4.340, supportive treatment = 4.157). The monthly medical expenditure at end of life was estimated at $2,139 for all decedents, and approximately a quarter of patients had received chemotherapy in the last 3 months. In conclusion, this study presented the quantified treatment costs of lung cancer on various aspects compared with matched controls according to the treatment of choice. In this study, patients with operation incurred lower lifetime treatment costs than patients with CTx/RTx or supportive treatment, indicating that the economic burden of lung cancer was affected by treatment method. Further studies including both cancer stage and treatment modality are needed to confirm these results and to provide more information on the economic burden according to disease severity.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Fitzmaurice C, Allen C, Barber RM, Barregard L, Bhutta ZA, Brenner H, et al. Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-years for 32 Cancer Groups, 1990 to 2015: A Systematic Analysis for the Global Burden of Disease Study. JAMA oncology. 2017;3(4):524–48. Epub 2016/12/06. 10.1001/jamaoncol.2016.5688 . - DOI - PMC - PubMed
-
- International Agency for Research on Cancer by World Health Organization. GLOBOCAN 2012: Estimated cancer incidence, mortality and prevalence worldwide in 2012. http://globocan.iarc.fr/Pages/fact_sheets_cancer.aspx Accessed in 1 July 2018. 2012.
-
- Youlden DR, Cramb SM, Baade PD. The International Epidemiology of Lung Cancer: geographical distribution and secular trends. Journal of thoracic oncology: official publication of the International Association for the Study of Lung Cancer. 2008;3(8):819–31. Epub 2008/08/02. 10.1097/JTO.0b013e31818020eb . - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

