Cyst Fluid Biosignature to Predict Intraductal Papillary Mucinous Neoplasms of the Pancreas with High Malignant Potential
- PMID: 30794864
- PMCID: PMC6487216
- DOI: 10.1016/j.jamcollsurg.2019.02.040
Cyst Fluid Biosignature to Predict Intraductal Papillary Mucinous Neoplasms of the Pancreas with High Malignant Potential
Abstract
Background: Current standard-of-care technologies, such as imaging and cyst fluid analysis, are unable to consistently distinguish intraductal papillary mucinous neoplasms (IPMNs) of the pancreas at high risk of pancreatic cancer from low-risk IPMNs. The objective was to create a single-platform assay to identify IPMNs that are at high risk for malignant progression.
Study design: Building on the Verona International Consensus Conference branch duct IPMN biomarker review, additional protein, cytokine, mucin, DNA, and microRNA cyst fluid targets were identified for creation of a quantitative polymerase chain reaction-based assay. This included messenger RNA markers: ERBB2, GNAS, interleukin 1β, KRAS, MUCs1, 2, 4, 5AC, 7, prostaglandin E2R, PTGER2, prostaglandin E synthase 2, prostaglandin E synthase 1, TP63; microRNA targets: miRs 101, 106b, 10a, 142, 155, 17, 18a, 21, 217, 24, 30a, 342, 532, 92a, and 99b; and GNAS and KRAS mutational analysis. A multi-institutional international collaborative contributed IPMN cyst fluid samples to validate this platform. Cyst fluid gene expression levels were normalized, z-transformed, and used in classification and regression analysis by a support vector machine training algorithm.
Results: From cyst fluids of 59 IPMN patients, principal component analysis confirmed no institutional bias/clustering. Lasso (least absolute shrinkage and selection operator)-penalized logistic regression with binary classification and 5-fold cross-validation used area under the curve as the evaluation criterion to create the optimal signature to discriminate IPMNs as low risk (low/moderate dysplasia) or high risk (high-grade dysplasia/invasive cancer). The most predictive signature was achieved with interleukin 1β, MUC4, and prostaglandin E synthase 2 to accurately discriminate high-risk cysts from low-risk cysts with an area under the curve of up to 0.86 (p = 0.002).
Conclusions: We have identified a single-platform polymerase chain reaction-based assay of cyst fluid to accurately predict IPMNs with high malignant potential for additional studies.
Copyright © 2019 American College of Surgeons. Published by Elsevier Inc. All rights reserved.
Figures

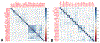

References
-
- Scheiman JM, Hwang JH, Moayyedi P. American gastroenterological association technical review on the diagnosis and management of asymptomatic neoplastic pancreatic cysts. Gastroenterology 2015; 148(4):824–48 e22. - PubMed
-
- Kimura W, Nagai H, Kuroda A, et al. Analysis of small cystic lesions of the pancreas. International Journal of Pancreatology 1995; 18(3):197–206. - PubMed
-
- Khoury RE, Kabir C, Maker VK, et al. What is the Incidence of Malignancy in Resected Intraductal Papillary Mucinous Neoplasms? An Analysis of Over 100 US Institutions in a Single Year. Ann Surg Oncol 2018; 25(6):1746–1751. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

