Increased production and reduced urinary buffering of acid in uric acid stone formers is ameliorated by pioglitazone
- PMID: 30795852
- PMCID: PMC6478507
- DOI: 10.1016/j.kint.2018.11.024
Increased production and reduced urinary buffering of acid in uric acid stone formers is ameliorated by pioglitazone
Abstract
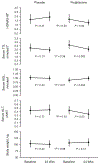
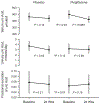
Idiopathic uric acid nephrolithiasis is characterized by an overly acidic urine pH caused by the combination of increased acid production and inadequate buffering of urinary protons by ammonia. A large proportion of uric acid stone formers exhibit features of the metabolic syndrome. We previously demonstrated that thiazolidinediones improved the urinary biochemical profile in an animal model of the metabolic syndrome. In this proof-of-concept study, we examined whether the thiazolidinedione pioglitazone can also ameliorate the overly acidic urine in uric acid stone formers. Thirty-six adults with idiopathic uric acid nephrolithiasis were randomized to pioglitazone 30 mg/day or matching placebo for 24 weeks. At baseline and study end, participants underwent collection of blood and 24-hour urine in an inpatient research unit while consuming a fixed metabolic diet, followed by assessment of the ammoniagenic response to an acute oral acid load. Twenty-eight participants completed the study. Pioglitazone treatment improved features of the metabolic syndrome. Pioglitazone also reduced net acid excretion and increased urine pH (5.37 to 5.59), the proportion of net acid excreted as ammonium, and ammonium excretion in response to an acute acid load, whereas these parameters were unchanged with placebo. Treatment of patients with idiopathic uric acid nephrolithiasis with pioglitazone for 24 weeks led to a reduction in the acid load presented to the kidney and a more robust ammoniagenesis and ammonium excretion, resulting in significantly higher urine pH. Future studies should consider the impact of this targeted therapy on uric acid stone formation.
Keywords: insulin resistance; metabolic syndrome; nephrolithiasis; pioglitazone; thiazolidinedione; uric acid.
Copyright © 2019 International Society of Nephrology. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Disclosures:
The authors disclose no competing interests.
Figures
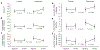
Comment in
-
Effect of thiazolidinedione therapy on the risk of uric acid stones.Kidney Int. 2019 May;95(5):1022-1024. doi: 10.1016/j.kint.2019.02.003. Kidney Int. 2019. PMID: 31010476
-
Re: Increased Production and Reduced Urinary Buffering of Acid in Uric Acid Stone Formers is Ameliorated by Pioglitazone.J Urol. 2019 Oct;202(4):655-656. doi: 10.1097/01.JU.0000577240.47597.4d. Epub 2019 Sep 6. J Urol. 2019. PMID: 31294658 No abstract available.
-
Pioglitazone and nephrolithiasis.Kidney Int. 2019 Aug;96(2):518-519. doi: 10.1016/j.kint.2019.04.015. Kidney Int. 2019. PMID: 31331471 No abstract available.
-
The authors reply.Kidney Int. 2019 Aug;96(2):519. doi: 10.1016/j.kint.2019.04.016. Kidney Int. 2019. PMID: 31331472 No abstract available.
-
Re: Increased Production and Reduced Urinary Buffering of Acid in Uric Acid Stone Formers is Ameliorated by Pioglitazone.Eur Urol. 2019 Dec;76(6):868-869. doi: 10.1016/j.eururo.2019.07.023. Epub 2019 Jul 24. Eur Urol. 2019. PMID: 31350069 No abstract available.
References
-
- Shoag J, Tasian GE, Goldfarb DS, et al. The new epidemiology of nephrolithiasis. Advances in chronic kidney disease. 2015;22(4):273–278. - PubMed
-
- Daudon M, Knebelmann B. [Epidemiology of urolithiasis]. La Revue du praticien. 2011. ;61 (3):372–378. - PubMed
-
- Maalouf NM, Cameron MA, Moe OW, et al. Novel insights into the pathogenesis of uric acid nephrolithiasis. Curr Opin Nephrol Hypertens. 2004;13(2):181–189. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

