An Interprofessional Standardized Patient Case for Improving Collaboration, Shared Accountability, and Respect in Team-Based Family Discussions
- PMID: 30800991
- PMCID: PMC6354797
- DOI: 10.15766/mep_2374-8265.10791
An Interprofessional Standardized Patient Case for Improving Collaboration, Shared Accountability, and Respect in Team-Based Family Discussions
Abstract
Introduction: The science of patient safety demonstrates that good communication is essential for effective interprofessional collaboration.
Methods: We created a low-stakes, formative assessment with which medical students, pharmacy students, and nursing students could practice several of the Interprofessional Education Collaborative competencies. We aimed to enable students to practice collaborative care, respect for other disciplines, and shared accountability. Senior students from medicine, nursing, and pharmacy worked in teams to disclose a medical error to a standardized patient. The activity began with an icebreaker exercise wherein students learned about each other. Next, each team planned a strategy for error disclosure and collaboratively disclosed the error. Standardized patients evaluated the team's performance. Subsequently, students regrouped for a debriefing. The participating institutions administered a survey to their students.
Results: In total, 1,151 students participated: 464 fourth-year students from the University of Houston College of Pharmacy, 450 third- and fourth-year students from Baylor College of Medicine, and 237 fourth-year students from Texas Woman's University Nelda C. Stark College of Nursing, all in Houston, Texas. Postsession survey data showed that students thought they achieved the relevant competencies. Students' understanding of the perspectives of the other two disciplines improved. Students found the simulation encounter and debriefing effective in helping them consider the contributions of other disciplines to patient care.
Discussion: This interprofessional standardized patient activity enabled collaborative problem solving. The debriefing discussion broadened students' understanding of the expertise of the other disciplines and promoted shared accountability. Students found this activity engaging and effective.
Keywords: Error Disclosure; Interprofessional Education.
Conflict of interest statement
None to report.
Figures
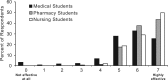

References
-
- Interprofessional Education Collaborative Expert Panel. Core Competencies for Interprofessional Collaborative Practice: Report of an Expert Panel. Washington, DC: Interprofessional Education Collaborative; 2011.
-
- Varpio L, Hall P, Lingard L, Schryer CF. Interprofessional communication and medical error: a reframing of research questions and approaches. Acad Med. 2008;83(10)(suppl):S76–S81. https://doi.org/10.1097/ACM.0b013e318183e67b - PubMed
-
- Interprofessional Education Collaborative. Core Competencies for Interprofessional Collaborative Practice: 2016 Update. Washington, DC: Interprofessional Education Collaborative; 2016.
-
- McDonough KA, White AA, Odegard PS, Shannon SE. Interprofessional error disclosure training for medical, nursing, pharmacy, dental, and physician assistant students. MedEdPORTAL. 2017;13:10606 https://doi.org/10.15766/mep_2374-8265.10606 - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
