Estimated Life-Time Savings in the Cost of Ongoing Care Following Specialist Rehabilitation for Severe Traumatic Brain Injury in the United Kingdom
- PMID: 30801440
- PMCID: PMC6687405
- DOI: 10.1097/HTR.0000000000000473
Estimated Life-Time Savings in the Cost of Ongoing Care Following Specialist Rehabilitation for Severe Traumatic Brain Injury in the United Kingdom
Abstract
Objectives: To evaluate cost-efficiency of rehabilitation following severe traumatic brain injury (TBI) and estimate the life-time savings in costs of care.
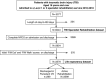
Setting/participants: TBI patients (n = 3578/6043) admitted to all 75 specialist rehabilitation services in England 2010-2018.
Design: A multicenter cohort analysis of prospectively collated clinical data from the UK Rehabilitation Outcomes Collaborative national clinical database.
Main measures: Primary outcomes: (a) reduction in dependency (UK Functional Assessment Measure), (b) cost-efficiency, measured in time taken to offset rehabilitation costs by savings in costs of ongoing care estimated by the Northwick Park Dependency Scale/Care Needs Assessment (NPDS/NPCNA), and (c) estimated life-time savings.
Results: The mean age was 49 years (74% males). Including patients who remained in persistent vegetative state on discharge, the mean episode cost of rehabilitation was £42 894 (95% CI: £41 512, £44 235), which was offset within 18.2 months by NPCNA-estimated savings in ongoing care costs. The mean period life expectancy adjusted for TBI severity was 21.6 years, giving mean net life-time savings in care costs of £679 776/patient (95% CI: £635 972, £722 786).
Conclusions: Specialist rehabilitation proved highly cost-efficient for severely disabled patients with TBI, despite their reduced life-span, potentially generating over £4 billion savings in the cost of ongoing care for this 8-year national cohort.
Figures
References
-
- Turner-Stokes L, Disler PB, Nair A, Wade DT. Multi-disciplinary rehabilitation for acquired brain injury in adults of working age. Cochrane Database Syst Rev. 2005;(3):CD004170. - PubMed
-
- Turner-Stokes L. Evidence for the effectiveness of multi-disciplinary rehabilitation following acquired brain injury: a synthesis of two systematic approaches. J Rehabil Med. 2008;40(9):691–701. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

