A unique case of ectopic Cushing's syndrome from a thymic neuroendocrine carcinoma
- PMID: 30802210
- PMCID: PMC6391898
- DOI: 10.1530/EDM-19-0002
A unique case of ectopic Cushing's syndrome from a thymic neuroendocrine carcinoma
Abstract
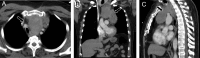
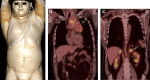
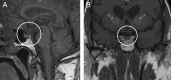
Ectopic adrenocorticotropic hormone (ACTH) production leading to ectopic ACTH syndrome accounts for a small proportion of all Cushing's syndrome (CS) cases. Thymic neuroendocrine tumors are rare neoplasms that may secrete ACTH leading to rapid development of hypercortisolism causing electrolyte and metabolic abnormalities, uncontrolled hypertension and an increased risk for opportunistic infections. We present a unique case of a patient who presented with a mediastinal mass, revealed to be an ACTH-secreting thymic neuroendocrine tumor (NET) causing ectopic CS. As the diagnosis of CS from ectopic ACTH syndrome (EAS) remains challenging, we emphasize the necessity for high clinical suspicion in the appropriate setting, concordance between biochemical, imaging and pathology findings, along with continued vigilant monitoring for recurrence after definitive treatment. Learning points: Functional thymic neuroendocrine tumors are exceedingly rare. Ectopic Cushing's syndrome secondary to thymic neuroendocrine tumors secreting ACTH present with features of hypercortisolism including electrolyte and metabolic abnormalities, uncontrolled hypertension and hyperglycemia, and opportunistic infections. The ability to undergo surgery and completeness of resection are the strongest prognostic factors for improved overall survival; however, the recurrence rate remains high. A high degree of initial clinical suspicion followed by vigilant monitoring is required for patients with this challenging disease.
Keywords: 2019; ACTH; ACTH stimulation; Adrenal; Adult; Bicarbonate; Bilateral adrenal hyperplasia; Biopsy; Blood pressure; Buffalo hump; CT scan; Chest pain; Chest pain (pleuritic); Chromogranin A; Cortisol; Cortisol, free (24-hour urine); Creatine kinase; Cushing's syndrome; Dexamethasone; Dexamethasone suppression; Dyspnoea; Ectopic ACTH syndrome; Ectopic Cushing's syndrome; Facial fullness; Facial plethora; February; Glucocorticoids; Glucose (blood); Histopathology; Hypercortisolaemia; Hyperglycaemia; Hyperpigmentation; Hypertension; Hypokalaemia; Hypotension; Immunohistochemistry; Ketoconazole; Leukocytosis; Lymphadenitis; Lymphadenopathy; MRI; Male; Metabolic alkalosis; Myasthaenia; Neuroendocrine tumour; Obesity; PET scan; Photosensitivity; Pituitary; Potassium; Resection of tumour; Rhabdomyolysis; Steroids; Supraclavicular fat pads; Synaptophysin; Syncope; Thymus; Unique/unexpected symptoms or presentations of a disease; United Kingdom; Weight gain; White; White blood cell count; X-ray.
Figures


References
-
- Liddle GW, Island DP, Ney RL, Nicholson WE, Shimizu N. Nonpituitary neoplasms and Cushing’s syndrome. Ectopic ‘adrenocorticotropin’ produced by nonpituitary neoplasms as a cause of Cushing’s syndrome. Archives of Internal Medicine 1963. 111 471–475. ( 10.1001/archinte.1963.03620280071011) - DOI - PubMed
-
- Travis W, Brambilla E, Burke A, Marx A & Nicholson AG. WHO Classification of Tumors of the Lung, Pleura, Thymus and Heart. Lyon: IARC Press, 2015. - PubMed
-
- Filosso PL, Yao X, Ahmad U, Zhan Y, Huang J, Ruffini E, Travis W, Lucchi M, Rimner A, Antonicelli A, et al Outcome of primary neuroendocrine tumors of the thymus: a joint analysis the International Thymic Malignancy Interest Group and the European Society of Thoracic Surgeons databases. Journal of Thoracic and Cardiovascular Surgery 2015. 149 103.e2–109.e2. ( 10.1016/j.jtcvs.2014.08.061) - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

