Risk factors affecting post-pubertal high serum follicle-stimulating hormone in patients with hypospadias
- PMID: 30820650
- PMCID: PMC6867975
- DOI: 10.1007/s00345-019-02687-w
Risk factors affecting post-pubertal high serum follicle-stimulating hormone in patients with hypospadias
Abstract
Purpose: The factors affecting spermatogenesis in adulthood in patients with hypospadias (HS) are not clearly understood. In the present study, risk factors affecting post-pubertal high serum follicle-stimulating hormone (FSH) were evaluated in patients with HS.
Materials and methods: Among those with a history of HS surgery, patients in whom endocrinological evaluation regarding pituitary-gonadal axis was performed at 15 years of age or older between March 2004 and April 2018 were enrolled in the present study. High serum FSH was defined as greater than 10 mIU/ml. The severity of HS was divided into mild and severe. Factors affecting the post-pubertal high serum FSH were estimated.
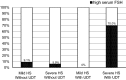
Results: Seventy-nine patients were included in the present study. The severity of HS was mild in 35 and severe in 44. History of undescended testis (UDT) was confirmed in 12. High serum FSH was detected in nine. On logistic regression model analysis, a history of UDT was the only significant factor for high serum FSH. The incidence of high serum FSH in patients with UDT was significantly higher than that in those without UDT (58.3% vs 7.5%, p < 0.01). When stratified by severity of HS and the presence of UDT, high serum FSH was detected in 70% in patients with severe HS and UDT, whereas less than 10% in other groups.
Conclusions: A history of UDT was a significant factor for post-pubertal high serum FSH in patients with HS. Accordingly, the presence of UDT may be a marker for impaired spermatogenesis in patients with HS, especially in severe cases.
Keywords: Follicle-stimulating hormone; Hypospadias; Spermatogenesis; Undescended testis.
Conflict of interest statement
The author(s) declare that they have no competing interests.
Figures
Similar articles
-
Long-term outcome of pituitary-gonadal axis and gonadal growth in patients with hypospadias at puberty.J Urol. 2010 Oct;184(4 Suppl):1610-4. doi: 10.1016/j.juro.2010.04.022. Epub 2010 Aug 21. J Urol. 2010. PMID: 20728133
-
Maternal first trimester serum levels of free-beta human chorionic gonadotrophin and male genital anomalies.Hum Reprod. 2016 Aug;31(8):1895-903. doi: 10.1093/humrep/dew150. Epub 2016 Jun 19. Hum Reprod. 2016. PMID: 27496947
-
A retrospective population-based cohort study to evaluate the impact of an older sibling with undescended testis and hypospadias on the known maternal and fetal risk factors for undescended testis and hypospadias in Ontario, Canada, 1997-2007.J Pediatr Urol. 2019 Feb;15(1):41.e1-41.e9. doi: 10.1016/j.jpurol.2018.09.021. Epub 2018 Oct 10. J Pediatr Urol. 2019. PMID: 30459092
-
The immature HPO axis.J Reprod Med. 1975 Jan;14(1):21-5. J Reprod Med. 1975. PMID: 1089157 Review.
-
The role of follicle-stimulating hormone in spermatogenesis: lessons from knockout animal models.Arch Med Res. 2001 Nov-Dec;32(6):601-8. doi: 10.1016/s0188-4409(01)00328-9. Arch Med Res. 2001. PMID: 11750736 Review.
Cited by
-
Sexual functions and fertility outcomes after hypospadias repair.Int J Impot Res. 2021 Mar;33(2):149-163. doi: 10.1038/s41443-020-00377-5. Epub 2020 Dec 1. Int J Impot Res. 2021. PMID: 33262531 Review.
References
-
- Marrocco G, Grammatico P, Vallasciani S, Gulia C, Zangari A, Marrocco F, Bateni ZH, Porrello A, Piergentili R. Environmental, parental and gestational factors that influence the occurrence of hypospadias in male patients. J Pediatr Urol. 2015;11(1):12–19. doi: 10.1016/j.jpurol.2014.10.003. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

