A multi-institutional analysis of presentation and outcomes for leptomeningeal disease recurrence after surgical resection and radiosurgery for brain metastases
- PMID: 30828727
- PMCID: PMC6682204
- DOI: 10.1093/neuonc/noz049
A multi-institutional analysis of presentation and outcomes for leptomeningeal disease recurrence after surgical resection and radiosurgery for brain metastases
Abstract
Background: Radiographic leptomeningeal disease (LMD) develops in up to 30% of patients following postoperative stereotactic radiosurgery (SRS) for brain metastases. However, the clinical relevancy of this finding and outcomes after various salvage treatments are not known.
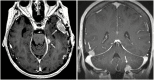
Methods: Patients with brain metastases, of which 1 was resected and treated with adjunctive SRS, and who subsequently developed LMD were combined from 7 tertiary care centers. LMD pattern was categorized as nodular (nLMD) or classical ("sugarcoating," cLMD).
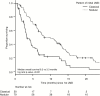
Results: The study cohort was 147 patients. Most patients (60%) were symptomatic at LMD presentation, with cLMD more likely to be symptomatic than nLMD (71% vs. 51%, P = 0.01). Salvage therapy was whole brain radiotherapy (WBRT) alone (47%), SRS (27%), craniospinal radiotherapy (RT) (10%), and other (16%), with 58% receiving a WBRT-containing regimen. WBRT was associated with lower second LMD recurrence compared with focal RT (40% vs 68%, P = 0.02). Patients with nLMD had longer median overall survival (OS) than those with cLMD (8.2 vs 3.3 mo, P < 0.001). On multivariable analysis for OS, pattern of initial LMD (nodular vs classical) was significant, but type of salvage RT (WBRT vs focal) was not.
Conclusions: Nodular LMD is a distinct pattern of LMD associated with postoperative SRS that is less likely to be symptomatic and has better OS outcomes than classical "sugarcoating" LMD. Although focal RT demonstrated increased second LMD recurrence compared with WBRT, there was no associated OS detriment. Focal cranial RT for nLMD recurrence after surgery and SRS for brain metastases may be a reasonable alternative to WBRT.
Keywords: brain metastases; leptomeningeal disease; postoperative radiosurgery; radiosurgery.
© The Author(s) 2019. Published by Oxford University Press on behalf of the Society for Neuro-Oncology. All rights reserved. For permissions, please e-mail: journals.permissions@oup.com.
Figures

Comment in
-
Nodular leptomeningeal disease after surgery for a brain metastasis-should we be concerned?Neuro Oncol. 2019 Aug 5;21(8):959-960. doi: 10.1093/neuonc/noz081. Neuro Oncol. 2019. PMID: 31051044 Free PMC article. No abstract available.
References
-
- Nayak L, Lee EQ, Wen PY. Epidemiology of brain metastases. Curr Oncol Rep. 2012;14(1):48–54. - PubMed
-
- Aoyama H, Shirato H, Tago M, et al. Stereotactic radiosurgery plus whole-brain radiation therapy vs stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA. 2006;295(21):2483–2491. - PubMed
-
- Chang EL, Wefel JS, Hess KR, et al. Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol. 2009;10(11):1037–1044. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

