Predictors of Lymphoceles in Women Who Underwent Laparotomic Retroperitoneal Lymph Node Dissection for Early Gynecologic Cancer: A Retrospective Cohort Study
- PMID: 30875912
- PMCID: PMC6466375
- DOI: 10.3390/ijerph16060936
Predictors of Lymphoceles in Women Who Underwent Laparotomic Retroperitoneal Lymph Node Dissection for Early Gynecologic Cancer: A Retrospective Cohort Study
Abstract
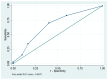
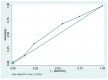
Background: Lymphoceles could represent a detrimental complication after retroperitoneal lymph node dissection. Our aim was to elucidate predictors of lymphoceles. Methods: Between 2011 and 2017, medical records of consecutive women who underwent laparotomic retroperitoneal lymph node dissection for FIGO stage I or II gynecologic cancer were reviewed. Results: A total of 204 women, including those with lymphoceles (n = 31) and symptomatic lymphoceles (n = 7), were reviewed. According to multivariable analysis, parity (odds ratio = 0.59, p = 0.003), adjuvant pelvic radiotherapy (odds ratio = 2.60, p = 0.039), and peritoneal nonclosure without pelvic drainage (odds ratio = 2.31, p = 0.048) were predictors of lymphoceles. In addition, parity (odds ratio = 0.73, p = 0.03), hypertension (odds ratio = 2.62, p = 0.02), and peritoneal partial closure with pelvic drainage (odds ratio = 0.27, p = 0.02) were predictors of complications. Conclusion: Low parity, adjuvant pelvic radiotherapy, and peritoneal nonclosure without pelvic drainage were associated with increased lymphocele formation. In addition, a lower complication rate was found in the peritoneal partial closure with pelvic drainage group; thus, peritoneal partial closure with pelvic drainage might be suggested for women who undergo laparotomic retroperitoneal lymph node dissection.
Keywords: drainage; gynecology; lymph node excision; lymphocele; peritoneum.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Effect of Peritoneal Fixation (PerFix) on Lymphocele Formation in Robot-assisted Radical Prostatectomy with Pelvic Lymphadenectomy: Results of a Randomized Prospective Trial.Eur Urol. 2023 Feb;83(2):154-162. doi: 10.1016/j.eururo.2022.07.027. Epub 2022 Aug 28. Eur Urol. 2023. PMID: 36041934 Clinical Trial.
-
Laparoscopic peritoneal drainage of symptomatic lymphoceles after pelvic lymph node dissection using methylene blue instillation.Urol Int. 2006;76(4):335-8. doi: 10.1159/000092058. Urol Int. 2006. PMID: 16679836
-
[CT in the diagnosis and treatment of lymphoceles following gynecologic cancer surgery].Radiol Med. 1993 Jul-Aug;86(1-2):106-15. Radiol Med. 1993. PMID: 8346341 Italian.
-
[Absence of peritonization after pelvic cancer surgery. Results in 157 cases].J Gynecol Obstet Biol Reprod (Paris). 1991;20(7):957-60. J Gynecol Obstet Biol Reprod (Paris). 1991. PMID: 1791288 Review. French.
-
Lymphocele: prevalence and management in gynecological malignancies.Expert Rev Anticancer Ther. 2014 Mar;14(3):307-17. doi: 10.1586/14737140.2014.866043. Epub 2014 Feb 3. Expert Rev Anticancer Ther. 2014. PMID: 24483760 Review.
Cited by
-
Resolution of large pelvic lymphocele after incidental intracystic hemorrhage caused by percutaneous catheter drainage: Case report.J Obstet Gynaecol Res. 2022 Apr;48(4):1050-1054. doi: 10.1111/jog.15178. Epub 2022 Feb 2. J Obstet Gynaecol Res. 2022. PMID: 35108750 Free PMC article.
-
Rapid recurrence of squamous cell carcinoma at a lymphocele after nephroureterectomy: A rare case report.IJU Case Rep. 2021 Feb 15;4(2):118-121. doi: 10.1002/iju5.12259. eCollection 2021 Mar. IJU Case Rep. 2021. PMID: 33718823 Free PMC article.
-
Risk factors for lymph ascites after surgery for endometrial cancer and impact on lymphedema of the legs. A prospective longitudinal Swedish multicenter study.Acta Obstet Gynecol Scand. 2025 May;104(5):976-987. doi: 10.1111/aogs.15077. Epub 2025 Mar 4. Acta Obstet Gynecol Scand. 2025. PMID: 40035366 Free PMC article.
-
Endovascular stent treatment of the iliac vein stenosis caused by a pelvic lymphocele secondary to gynecologic malignancy.J Interv Med. 2020 Aug 27;3(4):192-194. doi: 10.1016/j.jimed.2020.08.004. eCollection 2020 Dec. J Interv Med. 2020. PMID: 34805933 Free PMC article.
References
-
- Mori N. Clinical and experimental studies on the so-called lymphocyst which develops after radical hysterectomy in cancer of the uterine cervix. J. Jpn. Obstet. Gynecol. Soc. 1955;2:178–203. - PubMed
-
- Benedetti-Panici P., Maneschi F., Cutillo G., D’Andrea G., di Palumbo V.S., Conte M., Scambia G., Mancuso S. A randomized study comparing retroperitoneal drainage with no drainage after lymphadenectomy in gynecologic malignancies. Gynecol. Oncol. 1997;65:478–482. doi: 10.1006/gyno.1997.4648. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources