Choroid plexus tumours on MRI: similarities and distinctions in different grades
- PMID: 30894223
- PMCID: PMC6427869
- DOI: 10.1186/s40644-019-0200-1
Choroid plexus tumours on MRI: similarities and distinctions in different grades
Abstract
Background: The therapeutic planning varies for different grades of choroid plexus tumours (CPTs). The aim of this study was to define the similarities and distinctions among MRIs for different grades of CPTs, providing more guidance for clinical decisions.
Methods: We reviewed the MRI findings in 35 patients with CPT verified by surgical pathology, including 18 choroid plexus papillomas (CPPs, grade I), 11 atypical choroid plexus papillomas (aCPPs, grade II), and 6 choroid plexus carcinomas (CPCs, grade III). Nonparametric testing based on ranks was performed to evaluate the association of pathological grade with MRI findings.
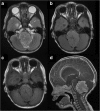
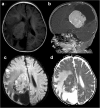
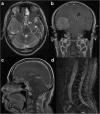
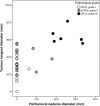
Results: Among the 35 CPTs, 29 were located in the ventricular system. The tumours were generally slightly hypo- or isointense on T1WI, slightly hyper- or isointense on T2WI, and moderately or strongly enhanced in post-contrast imaging. Twenty cases were accompanied by hydrocephalus. The median tumour longest diameters of CPPs, aCPPs, and CPCs were 28.6, 44.6, and 60.6 mm, respectively. Four cases were purely cystic, 6 were papillary, 10 were lobulated, and 2 were irregular. Three cases had necrosis. The median oedema diameters of CPPs, aCPPs, and CPCs were 0, 0, and 24.1 mm, respectively. The grades of CPTs were statistically associated with tumour longest diameter (rs = 0.68, P < 0.001), internal morphology (χ2 = 10.32, P = 0.016), necrosis (Z = 2.27, P = 0.023), and oedema diameter (rs = 0.72, P < 0.001).
Conclusion: CPTs typically appeared as intraventricular papillary or lobulated lesions, often accompanied by hydrocephalus. Larger tumour, irregular or fuzzy internal morphology, presentation of necrosis and wide-ranging peritumoural oedema might increase the likelihood of malignancy.
Keywords: Atypical choroid plexus papilloma; Choroid plexus carcinoma; Choroid plexus papilloma; Choroid plexus tumour; Magnetic resonance imaging; Pathological grade.
Conflict of interest statement
Ethics approval and consent to participate
Ethical approval was obtained from the Research Ethics Committee of Zhujiang Hospital of Southern Medical University and Guangdong 999 Brain Hospital. Informed consent was obtained from all patients.
Consent for publication
A copy of consent form could be requested at any stage.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures



Similar articles
-
Pediatric atypical choroid plexus papilloma: Clinical features and diagnosis.Clin Neurol Neurosurg. 2021 Jan;200:106345. doi: 10.1016/j.clineuro.2020.106345. Epub 2020 Nov 4. Clin Neurol Neurosurg. 2021. PMID: 33203591
-
Molecular characterization of choroid plexus tumors reveals novel clinically relevant subgroups.Clin Cancer Res. 2015 Jan 1;21(1):184-92. doi: 10.1158/1078-0432.CCR-14-1324. Epub 2014 Oct 21. Clin Cancer Res. 2015. PMID: 25336695
-
Choroid Plexus Tumors: Experience of 10 Cases with Special References to Adult Cases.Neurol Med Chir (Tokyo). 2015;55(12):891-900. doi: 10.2176/nmc.oa.2015-0126. Epub 2015 Oct 16. Neurol Med Chir (Tokyo). 2015. PMID: 26478476 Free PMC article.
-
Spinal drop metastasis from a benign fourth ventricular choroid plexus papilloma in a pediatric patient: case report.J Neurosurg Pediatr. 2017 Nov;20(5):471-479. doi: 10.3171/2017.5.PEDS17130. Epub 2017 Aug 25. J Neurosurg Pediatr. 2017. PMID: 28841111 Review.
-
[Choroid plexus tumours: cytogenetic analysis of a single case and literature review].Pathologica. 2007 Dec;99(6):424-7. Pathologica. 2007. PMID: 18416333 Review. Italian.
Cited by
-
Intracranial Subdural Fluid Accumulation Associated with a Choroid Plexus Carcinoma in a Dog.Vet Sci. 2022 Dec 30;10(1):24. doi: 10.3390/vetsci10010024. Vet Sci. 2022. PMID: 36669025 Free PMC article.
-
Atypical Choroid Plexus Papilloma in a Newborn, Misdiagnosed by Ultrasound and MRI: A Case Report.Am J Case Rep. 2024 Dec 13;25:e945575. doi: 10.12659/AJCR.945575. Am J Case Rep. 2024. PMID: 39668528 Free PMC article.
-
Diagnosis of choroid plexus papilloma: Current perspectives and future directions.Cancer Pathog Ther. 2023 Sep 26;2(3):173-179. doi: 10.1016/j.cpt.2023.09.005. eCollection 2024 Jul. Cancer Pathog Ther. 2023. PMID: 39027146 Free PMC article. Review.
-
Obstructive hydrocephalus due to choroid plexus carcinoma of third ventricle in pediatric: A rare case report.Radiol Case Rep. 2024 Sep 21;19(12):6112-6116. doi: 10.1016/j.radcr.2024.08.127. eCollection 2024 Dec. Radiol Case Rep. 2024. PMID: 39364273 Free PMC article.
-
Pre-operative embolization for staged treatment of infantile choroid plexus papilloma.Childs Nerv Syst. 2022 Feb;38(2):429-433. doi: 10.1007/s00381-021-05212-w. Epub 2021 May 19. Childs Nerv Syst. 2022. PMID: 34009420
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

