The Relationship Between Endplate Pathology and Patient-reported Symptoms for Chronic Low Back Pain Depends on Lumbar Paraspinal Muscle Quality
- PMID: 30896590
- PMCID: PMC6597281
- DOI: 10.1097/BRS.0000000000003035
The Relationship Between Endplate Pathology and Patient-reported Symptoms for Chronic Low Back Pain Depends on Lumbar Paraspinal Muscle Quality
Abstract
Study design: Cross-sectional cohort study of chronic low back pain (CLBP) patients and matched controls.
Objective: To explore the interplay between vertebral endplate damage and adjacent paraspinal muscle (PSM) quality, and to test their association in a cohort of patients with CLBP and matched controls.
Summary of background data: Nonspecific CLBP is challenging to diagnose, in part, due to uncertainty regarding the source of pain. Delineating interactions among potential CLBP mechanisms may enhance diagnosis and treatment customization.
Methods: We collected advanced MRI imaging on 52 adult subjects, including 38 CLBP patients and 14 age- and sex-matched asymptomatic control subjects. Mean multifidus and erector spinae fat fraction (FF) was measured throughout the spine using an IDEAL MRI sequence. Presence of cartilage endplate (CEP) defects was determined at each disc level using UTE MRI. Logistic regression was used to test association of PSM FF, CEP defects, modic changes (MC), disc degeneration, and their interplay.
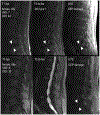
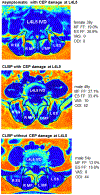
Results: We observed that CEP defects were the strongest predictor of nonspecific CLBP (OR: 14.1, P < 0.01) even after adjusting for MC and disc degeneration (OR: 26.1, P = 0.04). PSM quality did not independently distinguish patient and control groups, except for patients with high self-reported disability.At specifically L4L5, CEP damage was most prevalent and CEP damage was significantly associated with CLBP (OR: 3.7, 95% CI: 1.2-21.5, P = 0.03). CEP damage at L4L5 was predictive of CLBP when adjacent to PSMs with greater FF (MF, OR 14.7, P = 0.04; ES, OR: 17.3, P = 0.03), but not when PSM FF was lower and comparable to values in control, asymptomatic subjects.
Conclusion: These results demonstrate the clinically important reciprocity between passive and dynamic spinal stabilizers, and support the notion that therapies targeting the PSMs may provide clinical benefit even in the presence of other spinal pathologies.
Level of evidence: 4.
Figures

References
-
- Mok FPS, Samartzis D, Karppinen J, et al. Modic changes of the lumbar spine: prevalence, risk factors, and association with disc degeneration and low back pain in a large-scale population-based cohort. Spine J 2016;16:32–41. - PubMed
-
- Luoma K, Vehmas T, Kerttula L, et al. Chronic low back pain in relation to Modic changes, bony endplate lesions, and disc degeneration in a prospective MRI study. Eur Spine J 2016;25:2873–81. - PubMed
-
- Macintosh JE & Bogduk N The Biomechanics of the Lumbar Multifidus. Clin Biomech (Bristol, Avon) 1986;1:205–13. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

