Specialist palliative care support is associated with improved pain relief at home during the last 3 months of life in patients with advanced disease: analysis of 5-year data from the national survey of bereaved people (VOICES)
- PMID: 30898162
- PMCID: PMC6429790
- DOI: 10.1186/s12916-019-1287-8
Specialist palliative care support is associated with improved pain relief at home during the last 3 months of life in patients with advanced disease: analysis of 5-year data from the national survey of bereaved people (VOICES)
Abstract
Background: Studies have shown that more than half of patients with advanced progressive diseases approaching the end-of-life report pain and that pain relief for these patients is poorest at home compared to other care settings such as acute care facilities and hospice. Although home is the most common preferred place of death, the majority of deaths occur outside the home. Specialist palliative care is associated with improved quality of life, but systematic reviews of RCTs have failed to show a consistent association with better pain relief. The aim of this study was to examine the factors associated with good pain relief at home in the last 3 months of life for people with advanced progressive disease.
Methods: Data were obtained from the National Bereavement Survey in England, a cross-sectional post-bereavement survey of a stratified random sample of 246,763 deaths which were registered in England from 2011 to 2015. From 110,311 completed surveys (45% response rate), the analysis was based on individual-level data from 43,509 decedents who were cared for at home before death.
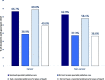
Results: Decedents who experienced good pain relief at home before death were significantly more likely to have received specialist palliative care (adjusted OR = 2.67; 95% CI, 2.62 to 2.72) and to have a recorded preferred place of death (adjusted OR = 1.87; 95% CI, 1.84 to 1.90) compared to those who did not. Good pain relief was more likely to be reported by a spouse or partner of the decedents compared to reports from their son or daughter (adjusted OR = 1.50, 95% CI, 1.47 to 1.53).
Conclusion: This study indicates that patients at home who are approaching the end-of-life experience substantially better pain relief if they receive specialist palliative care and their preferred place of death is recorded regardless of their disease aetiology.
Keywords: Advance care planning; End-of-life care; Home; Pain management; Palliative care; Primary care; Quality of Life.
Conflict of interest statement
Ethics approval and consent to participate
All data analysed in this study were secondary data that had been previously anonymised. This secondary data analysis study approved by the School of Medicine Ethics Committee (SoMREC) - University of Leeds (Ref no: MREC16-046). Ethical approval for the VOICES survey was granted from Southampton University Ethics Committee and the National Statistician’s Data Ethics Advisory [36].
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
Comment in
-
Access to specialist palliative care to manage pain in people dying at home: give them a VOICE.Evid Based Nurs. 2020 Apr;23(2):59. doi: 10.1136/ebnurs-2019-103130. Epub 2019 Jul 10. Evid Based Nurs. 2020. PMID: 31292151 No abstract available.
References
-
- British Medical Association. End-of-life care and physician-assisted dying. London: British Medical Association; 2016. https://scholar.google.com/scholar_lookup?hl=en&publication_year=2016&au.... Accessed 12 Feb 2019.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical