Hearing impairment after subarachnoid hemorrhage
- PMID: 30911566
- PMCID: PMC6414479
- DOI: 10.1002/acn3.714
Hearing impairment after subarachnoid hemorrhage
Erratum in
-
Erratum: Hearing impairment after subarachnoid hemorrhage.Ann Clin Transl Neurol. 2019 May 22;6(5):1006. doi: 10.1002/acn3.794. eCollection 2019 May. Ann Clin Transl Neurol. 2019. PMID: 31139699 Free PMC article.
Abstract
Background: Subarachnoid hemorrhage (SAH) survivors experience significant neurological disability, some of which is under-recognized by neurovascular clinical teams. We set out to objectively determine the occurrence of hearing impairment after SAH, characterize its peripheral and/or central origin, and investigate likely pathological correlates.
Methods: In a case-control study (n = 41), participants were asked about new onset hearing difficulty 3 months post-SAH, compared with pre-SAH. Formal audiological assessment included otoscopy, pure tone audiometry, a questionnaire identifying symptoms of peripheral hearing loss and/or auditory processing disorder, and a test of speech understanding in noise. A separate cohort (n = 21) underwent quantitative susceptibility mapping (QSM) of the auditory cortex 6 months after SAH, for correlation with hearing difficulty.
Results: Twenty three percent of SAH patients reported hearing difficulty that was new in onset post-SAH. SAH patients had poorer pure tone thresholds compared to controls. The proportion of patients with peripheral hearing loss as defined by the World Health Organization and British Audiological Society was however not increased, compared to controls. All SAH patients experienced symptoms of auditory processing disorder post-SAH, with speech-in-noise test scores significantly worse versus controls. Iron deposition in the auditory cortex was higher in patients reporting hearing difficulty versus those who did not.
Conclusion: This study firmly establishes hearing impairment as a frequent clinical feature after SAH. It primarily consists of an auditory processing disorder, mechanistically linked to iron deposition in the auditory cortex. Neurovascular teams should inquire about hearing, and refer SAH patients for audiological assessment and management.
Conflict of interest statement
Nothing to report.
Figures
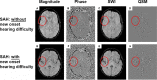


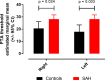

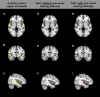

References
-
- Kreiter KT, Copeland D, Bernardini GL, et al. Predictors of cognitive dysfunction after subarachnoid hemorrhage. Stroke 2002;33:200–208. - PubMed
-
- Visser‐Meily JM, Rinkel GJ, Vergouwen MD, et al. Post‐traumatic stress disorder in patients 3 years after aneurysmal subarachnoid haemorrhage. Cerebrovasc Dis 2013;36:126–130. - PubMed
-
- Pace A, Mitchell S, Casselden E, et al. A subarachnoid haemorrhage‐specific outcome tool. Brain 2018;141:1111–1121. - PubMed
-
- Vos EM, Greebe P, Visser‐Meily JMA, et al. Subjective hearing impairment after subarachnoid haemorrhage: prevalence and risk factors. J Neurol Sci 2017;15:184–186. - PubMed
-
- British Society of Audiology (BSA). Auditory processing disorder special interest group. [Internet]. Bathgate, UK: BSA, 2018. https://www.thebsa.org.uk/wp-content/uploads/2018/02/Position-Statement-....
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
