Pacing in proximity to scar during cardiac resynchronization therapy increases local dispersion of repolarization and susceptibility to ventricular arrhythmogenesis
- PMID: 30930329
- PMCID: PMC6774764
- DOI: 10.1016/j.hrthm.2019.03.027
Pacing in proximity to scar during cardiac resynchronization therapy increases local dispersion of repolarization and susceptibility to ventricular arrhythmogenesis
Abstract
Background: Cardiac resynchronization therapy (CRT) increases the risk of ventricular tachycardia (VT) in patients with ischemic cardiomyopathy (ICM) when the left ventricular (LV) epicardial lead is implanted in proximity to scar.
Objective: The purpose of this study was to determine the mechanisms underpinning this risk by investigating the effects of pacing on local electrophysiology (EP) in relation to scar that provides a substrate for VT in ICM patients undergoing CRT.
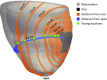
Methods: Imaging data from ICM patients (n = 24) undergoing CRT were used to create patient-specific LV anatomic computational models including scar morphology. Simulations of LV epicardial pacing at 0.2-4.5 cm from the scar were performed using EP models of chronic infarct and heart failure (HF). Dispersion of repolarization and the vulnerable window were computed as surrogates for VT risk.
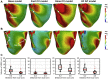
Results: Simulations predict that pacing in proximity to scar (0.2 cm) compared to more distant pacing to a scar (4.5 cm) significantly (P <.01) increased dispersion of repolarization in the vicinity of the scar and widened (P <.01) the vulnerable window, increasing the likelihood of unidirectional block. Moreover, slow conduction during HF further increased dispersion (∼194%). Analysis of variance and post hoc tests show significantly (P <.01) reduced repolarization dispersion when pacing ≥3.5 cm from the scar compared to pacing at 0.2 cm.
Conclusion: Increased dispersion of repolarization in the vicinity of the scar and widening of the vulnerable window when pacing in proximity to scar provides a mechanistic explanation for VT induction in ICM-CRT with lead placement proximal to scar. Pacing 3.5 cm or more from scar may avoid increasing VT risk in ICM-CRT patients.
Keywords: Cardiac resynchronization therapy; Infarct scar; Patient-specific modeling; Ventricular tachycardia.
Copyright © 2019 The Authors. Published by Elsevier Inc. All rights reserved.
Figures




References
-
- Mykytsey A., Maheshwari P., Dhar G. Ventricular tachycardia induced by biventricular pacing in patient with severe ischemic cardiomyopathy. J Cardiovasc Electrophysiol. 2005;16:655–658. - PubMed
-
- Peichl P., Mlčochová H., Kautzner J. Successful catheter ablation of two types of ventricular tachycardias triggered by cardiac resynchronization therapy: a case report. J Cardiovasc Electrophysiol. 2007;18:218–221. - PubMed
-
- Asvestas D., Balasubramaniam R., Sopher M., Paisey J., Babu G.G. Extended bipolar left ventricular pacing as a possible therapy for late electrical storm induced by cardiac resynchronization therapy. J Electrocardiol. 2017;50:349–352. - PubMed
-
- Roque C., Trevisi N., Silberbauer J. Electrical storm induced by cardiac resynchronization therapy is determined by pacing on epicardial scar and can be successfully managed by catheter ablation. Circ Arrhythmia Electrophysiol. 2014;7:1064–1069. - PubMed
-
- Nayak H.M., Verdino R.J., Russo A.M. Ventricular tachycardia storm after initiation of biventricular pacing: incidence, clinical characteristics, management, and outcome. J Cardiovasc Electrophysiol. 2008;19:708–715. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

