Tattoo free setup for partial breast irradiation: A feasibility study
- PMID: 30945803
- PMCID: PMC6448163
- DOI: 10.1002/acm2.12557
Tattoo free setup for partial breast irradiation: A feasibility study
Abstract
Purpose: Patients undergoing external beam accelerated partial breast irradiation (APBI) receive permanent tattoos to aid with daily setup alignment and verification. With the advent of three-dimensional (3D) body surface imaging and two-dimensional (2D) x-ray imaging-based matching to surgical clips, tattoos may not be necessary to ensure setup accuracy. We compared the accuracy of conventional tattoo-based setups to a patient setup without tattoos.
Materials/methods: Twenty consecutive patients receiving APBI at our institution from July 10, 2017 to February 13, 2018 were identified. All patients received tattoos per standard of care. Ten patients underwent setup using tattoos for initial positioning followed by surface imaging and 2D matching of surgical clips. The other ten patients underwent positioning using surface imaging followed by 2D matching without reference to tattoos. Overall setup time and orthogonal x-ray-based shifts after surface imaging per fraction were recorded. Shift data were used to calculate systematic and random error.
Results: Among ten patients in the "no tattoo" group, the average setup time per fraction was 6.83 min vs 8.03 min in the tattoo cohort (P < 0.01). Mean 3D vector shifts for patients in the "no tattoo" group were 4.6 vs 5.9 mm in the "tattoo" cohort (P = NS). Mean systematic errors in the "no tattoo" group were: 1.2 mm (1.5 mm SD) superior/inferior, 0.5 mm (1.6 mm SD) right/left, and 2.3 mm (1.9 mm SD) anterior/posterior directions. Mean systematic errors in the "tattoo" group were: 0.8 mm (2.2 mm SD) superior/inferior, 0.3 mm (2.5 mm SD) right/left, and 1.4 mm (4.4 mm SD) anterior/posterior directions. The random errors in the "no tattoo" group ranged from 0.6 to 0.7 mm vs 1.2 to 1.7 mm in the "tattoo" group.
Conclusions: Using both surface imaging and 2D matching to surgical clips provides excellent accuracy in APBI patient alignment and setup verification with reduced setup time relative to the tattoo cohort. Skin-based tattoos may no longer be warranted for patients receiving external beam APBI.
Keywords: APBI; breast radiotherapy; surface imaging; tattoos.
© 2019 The Authors. Journal of Applied Clinical Medical Physics published by Wiley Periodicals, Inc. on behalf of American Association of Physicists in Medicine.
Conflict of interest statement
Dr. Gierga has previously received speaking honoraria for VisionRT. The remaining authors have no conflict of interest to disclose.
Figures
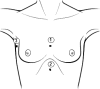
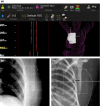
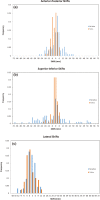

References
-
- Fobair P, Stewart SL, Chang S, et al. Body image and sexual problems in young women with breast cancer. Psychooncology. 2006;15:579–594. - PubMed
-
- Clow B, Allen J. Psychosocial impacts of radiation tattooing for breast cancer patients: a critical review. Canadian Woman Studies. 2010;28:46–52.
-
- Sewak S, Graham P, Nankervis J. Tattoo allergy in patients receiving adjuvant radiotherapy for breast cancer. Austr Radiol. 1999;43:558–561. - PubMed
-
- Bregnhol A, Haedersal M. Q‐switched YAG laser vs. punch biopsy excision for iatrogenic radiation tattoo markers – a randomized controlled trial. J Eur Acam Dermatol Venereol. 2010;24:1183–1186. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

