Relationship between multimorbidity, demographic factors and mortality: findings from the UK Biobank cohort
- PMID: 30967141
- PMCID: PMC6456941
- DOI: 10.1186/s12916-019-1305-x
Relationship between multimorbidity, demographic factors and mortality: findings from the UK Biobank cohort
Abstract
Background: Multimorbidity is associated with higher mortality, but the relationship with cancer and cardiovascular mortality is unclear. The influence of demographics and type of condition on the relationship of multimorbidity with mortality remains unknown. We examine the relationship between multimorbidity (number/type) and cause of mortality and the impact of demographic factors on this relationship.
Methods: Data source: the UK Biobank; 500,769 participants; 37-73 years; 53.7% female. Exposure variables: number and type of long-term conditions (LTCs) (N = 43) at baseline, modelled separately. Cox regression models were used to study the impact of LTCs on all-cause/vascular/cancer mortality during median 7-year follow-up. All-cause mortality regression models were stratified by age/sex/socioeconomic status.
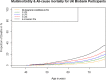
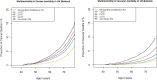
Results: All-cause mortality is 2.9% (14,348 participants). Of all deaths, 8350 (58.2%) were cancer deaths and 2985 (20.8%) vascular deaths. Dose-response relationship is observed between the increasing number of LTCs and all-cause/cancer/vascular mortality. A strong association is observed between cardiometabolic multimorbidity and all three clinical outcomes; non-cardiometabolic multimorbidity (excluding cancer) is associated with all-cause/vascular mortality. All-cause mortality risk for those with ≥ 4 LTCs was nearly 3 times higher than those with no LTCs (HR 2.79, CI 2.61-2.98); for ≥ 4 cardiometabolic conditions, it was > 3 times higher (HR 3.20, CI 2.56-4.00); and for ≥ 4 non-cardiometabolic conditions (excluding cancer), it was 50% more (HR 1.50, CI 1.36-1.67). For those with ≥ 4 LTCs, morbidity combinations that included cardiometabolic conditions, chronic kidney disease, cancer, epilepsy, chronic obstructive pulmonary disease, depression, osteoporosis and connective tissue disorders had the greatest impact on all-cause mortality. In the stratified model by age/sex, absolute all-cause mortality was higher among the 60-73 age group with an increasing number of LTCs; however, the relative effect size of the increasing number of LTCs on higher mortality risk was larger among those 37-49 years, especially men. While socioeconomic status was a significant predictor of all-cause mortality, mortality risk with increasing number of LTCs remained constant across different socioeconomic gradients.
Conclusions: Multimorbidity is associated with higher all-cause/cancer/vascular mortality. Type, as opposed to number, of LTCs may have an important role in understanding the relationship between multimorbidity and mortality. Multimorbidity had a greater relative impact on all-cause mortality in middle-aged as opposed to older populations, particularly males, which deserves exploration.
Keywords: Cancer mortality; Condition clusters; Mortality; Multimorbidity; Vascular mortality.
Conflict of interest statement
Ethics approval and consent to participate
All participants gave informed consent for data provision and linkage. UK Biobank has full ethical approval from the NHS National Research Ethics Service (16/NW/0274).
Consent for publication
The authors confirm that this manuscript does not contain any personal data or images from any individual participants.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Academy of Medical Sciences. Multimorbidity: a priority for global health research. 2018. https://acmedsci.ac.uk/file-download/82222577. Accessed 18 Mar 2019.
-
- Arokiasamy P, Uttamacharya U, Jain K, Biritwum RB, Yawson AE, Wu F, et al. The impact of multimorbidity on adult physical and mental health in low- and middle-income countries: what does the study on global ageing and adult health (SAGE) reveal? BMC Med. 2015;13:178. doi: 10.1186/s12916-015-0402-8. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

