Effect of preconception low dose aspirin on pregnancy and live birth according to socioeconomic status: A secondary analysis of a randomized clinical trial
- PMID: 30998747
- PMCID: PMC6472730
- DOI: 10.1371/journal.pone.0200533
Effect of preconception low dose aspirin on pregnancy and live birth according to socioeconomic status: A secondary analysis of a randomized clinical trial
Abstract
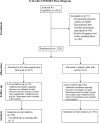
Low socioeconomic status (SES) is associated with adverse pregnancy outcomes and infertility. Low-dose aspirin (LDA) was shown to improve livebirth rates in certain subsets of women, and therefore, may impact pregnancy rates differentially by SES status. Therefore, the aim of the current study was to examine whether daily preconception-initiated LDA affects rates of pregnancy, livebirth, and pregnancy loss differently across strata of socioeconomic status (SES). This is a secondary analysis of The Effects of Aspirin in Gestation and Reproduction (EAGeR) Trial, a multisite, block- randomized, placebo-controlled trial conducted at four U.S. medical centers (n = 1,228, 2007-2012). Women attempting spontaneous conception with a history of pregnancy loss were randomly allocated preconception to 81mg of aspirin + 400mcg of folic acid (n = 615) or placebo + 400mcg of folic acid (n = 613). Study medication was administered for six menstrual cycles or until 36 weeks' gestation if pregnancy was achieved. For this analysis, women were stratified by SES, which included income (low, mid, high) and a combined grouping of education and income (low-low, low-high, high-low, high-high). Log binomial models with robust variance estimated risks of pregnancy, livebirth, and pregnancy loss for LDA versus placebo. LDA increased pregnancy and livebirth rates (RR 1.23, 95% CI: 1.03, 1.45) in the high-income, but not mid- or low-income groups. LDA increased pregnancy rates in both the low education-low income group (RR 1.22, 95% CI: 1.02, 1.46) and the high education-high income group (RR 1.23, 95%CI: 1.06, 1.42), with no effect observed in mid-SES groupings. LDA, a low-cost and widely available treatment, may be particularly beneficial to women at the highest and lowest ends of the socioeconomic spectrum, though underlying mechanisms of this disparity are unclear. Confirming these findings and identifying factors which may modulate the effectiveness of LDA will ultimately facilitate personalized clinical care and improvements in population-level reproductive health. Trial registration number: ClinicalTrials.gov, NCT00467363.
Conflict of interest statement
Study funding/competing interest(s): Eunice Kennedy Shriver National Institute of Child Health and Human Development (Contract Nos. HHSN267200603423, HHSN267200603424, HHSN267200603426); NIH Medical Research Scholars Program; Doris Duke Charitable Foundation (Grant #2014194). The authors have no competing interests to report. Trial registration number: ClinicalTrials.gov, NCT00467363.
References
-
- Marmot MG, Shipley MJ, Rose G. Inequalities in death—specific explanations of a general pattern? Lancet. 1984;1(8384): 1003–1006. - PubMed
-
- Singh GK, Siahpush M. Increasing inequalities in all-cause and cardiovascular mortality among US adults aged 25–64 years by area socioeconomic status, 1969–1998. Int J Epidemiol. 2002;31(3): 600–613. - PubMed
-
- Kramer MS, Seguin L, Lydon J, Goulet L. Socio-economic disparities in pregnancy outcome: why do the poor fare so poorly? Paediatr Perinat Epidemiol. 2000;14(3): 194–210. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical