Phase 1 repolarization rate defines Ca2+ dynamics and contractility on intact mouse hearts
- PMID: 31000581
- PMCID: PMC6571993
- DOI: 10.1085/jgp.201812269
Phase 1 repolarization rate defines Ca2+ dynamics and contractility on intact mouse hearts
Abstract
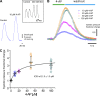
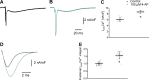
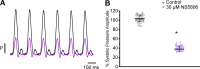
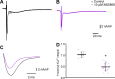
In the heart, Ca2+ influx through L-type Ca2+ channels triggers Ca2+ release from the sarcoplasmic reticulum. In most mammals, this influx occurs during the ventricular action potential (AP) plateau phase 2. However, in murine models, the influx through L-type Ca2+ channels happens in early repolarizing phase 1. The aim of this work is to assess if changes in the open probability of 4-aminopyridine (4-AP)-sensitive Kv channels defining the outward K+ current during phase 1 can modulate Ca2+ currents, Ca2+ transients, and systolic pressure during the cardiac cycle in intact perfused beating hearts. Pulsed local-field fluorescence microscopy and loose-patch photolysis were used to test the hypothesis that a decrease in a transient K+ current (Ito) will enhance Ca2+ influx and promote a larger Ca2+ transient. Simultaneous recordings of Ca2+ transients and APs by pulsed local-field fluorescence microscopy and loose-patch photolysis showed that a reduction in the phase 1 repolarization rate increases the amplitude of Ca2+ transients due to an increase in Ca2+ influx through L-type Ca2+ channels. Moreover, 4-AP induced an increase in the time required for AP to reach 30% repolarization, and the amplitude of Ca2+ transients was larger in epicardium than endocardium. On the other hand, the activation of Ito with NS5806 resulted in a reduction of Ca2+ current amplitude that led to a reduction of the amplitude of Ca2+ transients. Finally, the 4-AP effect on AP phase 1 was significantly smaller when the L-type Ca2+ current was partially blocked with nifedipine, indicating that the phase 1 rate of repolarization is defined by the competition between an outward K+ current and an inward Ca2+ current.
© 2019 López-Alarcón et al.
Figures





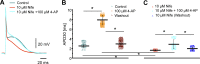


Similar articles
-
Transmural Autonomic Regulation of Cardiac Contractility at the Intact Heart Level.Front Physiol. 2019 Jul 3;10:773. doi: 10.3389/fphys.2019.00773. eCollection 2019. Front Physiol. 2019. PMID: 31333477 Free PMC article.
-
Intact Heart Loose Patch Photolysis Reveals Ionic Current Kinetics During Ventricular Action Potentials.Circ Res. 2016 Jan 22;118(2):203-15. doi: 10.1161/CIRCRESAHA.115.307399. Epub 2015 Nov 12. Circ Res. 2016. PMID: 26565013 Free PMC article.
-
Modulation of Ca(2+) release in cardiac myocytes by changes in repolarization rate: role of phase-1 action potential repolarization in excitation-contraction coupling.Circ Res. 2002 Feb 8;90(2):165-73. doi: 10.1161/hh0202.103315. Circ Res. 2002. PMID: 11834709
-
Regulation of cardiac excitation-contraction coupling by action potential repolarization: role of the transient outward potassium current (I(to)).J Physiol. 2003 Jan 1;546(Pt 1):5-18. doi: 10.1113/jphysiol.2002.026468. J Physiol. 2003. PMID: 12509475 Free PMC article. Review.
-
Physiological roles of the transient outward current Ito in normal and diseased hearts.Front Biosci (Schol Ed). 2016 Jan 1;8(1):143-59. doi: 10.2741/s454. Front Biosci (Schol Ed). 2016. PMID: 26709904 Review.
Cited by
-
Preventing the phosphorylation of RyR2 at canonical sites reduces Ca2+ leak and promotes arrhythmia by reactivating the INa current.Nat Cardiovasc Res. 2025 Aug;4(8):976-990. doi: 10.1038/s44161-025-00693-3. Epub 2025 Aug 12. Nat Cardiovasc Res. 2025. PMID: 40797044 Free PMC article.
-
Transmural Autonomic Regulation of Cardiac Contractility at the Intact Heart Level.Front Physiol. 2019 Jul 3;10:773. doi: 10.3389/fphys.2019.00773. eCollection 2019. Front Physiol. 2019. PMID: 31333477 Free PMC article.
-
Autonomic Regulation of the Goldfish Intact Heart.Front Physiol. 2022 Feb 9;13:793305. doi: 10.3389/fphys.2022.793305. eCollection 2022. Front Physiol. 2022. PMID: 35222073 Free PMC article.
-
Thermal modulation of epicardial Ca2+ dynamics uncovers molecular mechanisms of Ca2+ alternans.J Gen Physiol. 2021 Feb 1;153(2):e202012568. doi: 10.1085/jgp.202012568. J Gen Physiol. 2021. PMID: 33410862 Free PMC article.
-
Excitation-Contraction Coupling in the Goldfish (Carassius auratus) Intact Heart.Front Physiol. 2020 Sep 11;11:1103. doi: 10.3389/fphys.2020.01103. eCollection 2020. Front Physiol. 2020. PMID: 33041845 Free PMC article.

