Spinal Cord Ependymoma - Surgical Management and Outcome
- PMID: 31001024
- PMCID: PMC6454966
- DOI: 10.4103/jnrp.jnrp_267_18
Spinal Cord Ependymoma - Surgical Management and Outcome
Abstract
Background: Ependymoma is a common primary neoplasm of the spinal cord and filum terminale. Patients with spinal ependymoma usually experience gradual symptoms due to slow progression of the tumor; thus, early diagnosis can be challenging to make.
Objective: The objective of this study was to report 5 years' experience in treating spinal intramedullary ependymomas and to illustrate the advantage of aggressive complete resection whenever possible.
Patients and methods: Retrospective medical notes of all patients with spinal ependymoma treated surgically over a 5-year period between January 2003 and January 2008 were recorded. Clinical presentation, spinal level, extent of resection, and complications were recorded. A prolonged follow-up was documented.
Results: There were 20 patients - 11 males, and nine females -included in this study. Their median age was 48 years (range 3-75 years). In 18 patients, total gross resection was achieved. Subtotal resection was only possible in one patient due to surgical difficulty. One patient underwent biopsy and referred for further surgery and subsequently had total resection.
Conclusions: Radical total resection is achievable in spinal ependymomas, with minimal resultant morbidity.
Keywords: Ependymoma; intramedullary; myxopapillary; spinal tumors; spine.
Conflict of interest statement
There are no conflicts of interest.
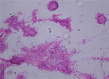
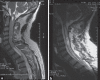
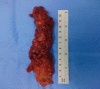
Figures

Similar articles
-
Spinal ependymomas. Part 2: Ependymomas of the filum terminale.Neurosurg Focus. 2015 Aug;39(2):E7. doi: 10.3171/2015.5.FOCUS15151. Neurosurg Focus. 2015. PMID: 26235024
-
Concomitant localization of a myxopapillary ependymoma at the middle thoracic part of the spinal cord and at the distal part of the filum terminale. Case report.J Neurosurg Sci. 2008 Sep;52(3):87-91. J Neurosurg Sci. 2008. PMID: 18636054
-
Outcome of surgery for intramedullary spinal ependymoma.Ann Saudi Med. 2008 Mar-Apr;28(2):109-13. doi: 10.5144/0256-4947.2008.109. Ann Saudi Med. 2008. PMID: 18398287 Free PMC article.
-
MYXOPAPILLARY EPENDYMOMA OF THE SPINAL CORD IN ADULTS: A REPORT OF PERSONAL SERIES AND REVIEW OF LITERATURE.Acta Clin Croat. 2020 Jun;59(2):329-337. doi: 10.20471/acc.2020.59.02.17. Acta Clin Croat. 2020. PMID: 33456121 Free PMC article. Review.
-
Remarkable efficacy of temozolomide for relapsed spinal myxopapillary ependymoma with multiple recurrence and cerebrospinal dissemination: a case report and literature review.Eur Spine J. 2018 Jul;27(Suppl 3):421-425. doi: 10.1007/s00586-017-5413-z. Epub 2017 Dec 21. Eur Spine J. 2018. PMID: 29270703 Review.
Cited by
-
Disease characteristics and clinical specific survival prediction of spinal ependymoma: a genetic and population-based study.Front Neurol. 2024 Sep 13;15:1454061. doi: 10.3389/fneur.2024.1454061. eCollection 2024. Front Neurol. 2024. PMID: 39346772 Free PMC article.
-
Clinical presentation and extent of resection impacts progression-free survival in spinal ependymomas.J Neurooncol. 2024 May;167(3):437-446. doi: 10.1007/s11060-024-04623-4. Epub 2024 Mar 4. J Neurooncol. 2024. PMID: 38438766 Free PMC article.
-
Intramedullary clear cell ependymoma of the lower thoracic spinal cord: report of a new case.Surg Neurol Int. 2020 Dec 11;11:423. doi: 10.25259/SNI_215_2020. eCollection 2020. Surg Neurol Int. 2020. PMID: 33365185 Free PMC article.
References
-
- Helseth A, Mørk SJ. Primary intraspinal neoplasms in Norway, 1955 to 1986. A population-based survey of 467 patients. J Neurosurg. 1989;71:842–5. - PubMed
-
- Fourney DR, Siadati A, Bruner JM, Gokaslan ZL, Rhines LD. Giant cell ependymoma of the spinal cord. Case report and review of the literature. J Neurosurg. 2004;100:75–9. - PubMed
-
- Chang UK, Choe WJ, Chung SK, Chung CK, Kim HJ. Surgical outcome and prognostic factors of spinal intramedullary ependymomas in adults. J Neurooncol. 2002;57:133–9. - PubMed
-
- Sakai Y, Matsuyama Y, Katayama Y, Imagama S, Ito Z, Wakao N, et al. Spinal myxopapillary ependymoma: Neurological deterioration in patients treated with surgery. Spine (Phila Pa 1976) 2009;34:1619–24. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
