Chlamydia trachomatis bacterial load, estimated by Cq values, in urogenital samples from men and women visiting the general practice, hospital or STI clinic
- PMID: 31002729
- PMCID: PMC6474615
- DOI: 10.1371/journal.pone.0215606
Chlamydia trachomatis bacterial load, estimated by Cq values, in urogenital samples from men and women visiting the general practice, hospital or STI clinic
Abstract
Background: The bacterial load of Chlamydia trachomatis (CT) is assumed to play a role in transmission and sequelae. We assessed urogenital CT cycle quantification (Cq) values, as an indicator for CT load, of men and women diagnosed by general practitioners (GPs), hospital physicians and the STI clinic.
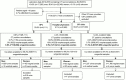
Methods: Urogenital CT-positive samples (n = 2,055 vaginal swabs, n = 77 cervical swabs, n = 1,519 urine samples and n = 19 urethral swabs) diagnosed by GPs, hospital physicians and the STI clinic from the Maastricht Medical Microbiology Laboratory were included (2012-2016). The outcome measure 'urogenital Cq values' was used as an inversely proportional measure for CT load. Among all patients, multivariate linear regression analyses were used to assess primary determinants for mean urogenital Cq values, stratified by sex. Additional clinical determinants were assessed among STI clinic patients.
Results: In men, mean urogenital Cq values were similar between GPs, hospital physicians and the STI clinic (32.7 and 33.5 vs. 32.7; p>0.05). Women visiting the GP had lower urogenital Cq values than women visiting the STI clinic (30.2 vs. 30.9; p = <0.001). Women visiting the hospital had higher urogenital Cq values than women visiting the STI clinic (32.4 vs. 30.9; p = <0.001). Among STI clinic women, urogenital Cq values were lower in women with concurrent anorectal CT and in rectally untested women compared to anorectal CT-negative women (30.7 and 30.6 vs. 33.9; p = <0.001).
Conclusion: Men visiting different STI care providers had similar urogenital Cq values, which could be an indicator for similar CT loads. The lower Cq values of women visiting the GP compared to women visiting the STI clinic could be an indicator for higher CT loads and likely higher transmission potential. Notably, urogenital Cq values of STI clinic women were much lower (>3 Cq) when STI clinic women also had anorectal CT. This finding could indicate higher urogenital CT loads and likely higher chances of transmission and sequelae.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

Similar articles
-
Spontaneous clearance of urogenital, anorectal and oropharyngeal Chlamydia trachomatis and Neisseria gonorrhoeae in women, MSM and heterosexual men visiting the STI clinic: a prospective cohort study.Sex Transm Infect. 2019 Nov;95(7):505-510. doi: 10.1136/sextrans-2018-053825. Epub 2019 Mar 11. Sex Transm Infect. 2019. PMID: 30858330
-
Who tests whom? A comprehensive overview of Chlamydia trachomatis test practices in a Dutch region among different STI care providers for urogenital, anorectal and oropharyngeal sites in young people: a cross-sectional study.Sex Transm Infect. 2016 May;92(3):211-7. doi: 10.1136/sextrans-2015-052065. Epub 2015 Aug 11. Sex Transm Infect. 2016. PMID: 26265066
-
Men and Women Have an Equal Oropharyngeal and Anorectal Chlamydia trachomatis Bacterial Load: A Comparison of 3 Anatomic Sites.J Infect Dis. 2021 May 20;223(9):1582-1589. doi: 10.1093/infdis/jiz668. J Infect Dis. 2021. PMID: 31840181
-
Standardisation is necessary in urogenital and extragenital Chlamydia trachomatis bacterial load determination by quantitative PCR: a review of literature and retrospective study.Sex Transm Infect. 2019 Dec;95(8):562-568. doi: 10.1136/sextrans-2018-053522. Epub 2019 Feb 7. Sex Transm Infect. 2019. PMID: 30733424
-
Use and Misuse of Cq in qPCR Data Analysis and Reporting.Life (Basel). 2021 May 29;11(6):496. doi: 10.3390/life11060496. Life (Basel). 2021. PMID: 34072308 Free PMC article. Review.
Cited by
-
Cervical Cytology of Samples with Ureaplasma urealyticum, Ureaplasma parvum, Chlamydia trachomatis, Trichomonas vaginalis, Mycoplasma hominis, and Neisseria gonorrhoeae Detected by Multiplex PCR.Biomed Res Int. 2020 Jul 7;2020:7045217. doi: 10.1155/2020/7045217. eCollection 2020. Biomed Res Int. 2020. PMID: 32724807 Free PMC article.
-
The characteristics of patients frequently tested and repeatedly infected with Chlamydia trachomatis in Southwest Limburg, the Netherlands.BMC Public Health. 2020 Aug 14;20(1):1239. doi: 10.1186/s12889-020-09334-9. BMC Public Health. 2020. PMID: 32795362 Free PMC article.
-
Controversies and evidence on Chlamydia testing and treatment in asymptomatic women and men who have sex with men: a narrative review.BMC Infect Dis. 2022 Mar 14;22(1):255. doi: 10.1186/s12879-022-07171-2. BMC Infect Dis. 2022. PMID: 35287617 Free PMC article. Review.
-
Diagnosis of Chlamydia trachomatis genital infections in the era of genomic medicine.Braz J Microbiol. 2021 Sep;52(3):1327-1339. doi: 10.1007/s42770-021-00533-z. Epub 2021 Jun 23. Braz J Microbiol. 2021. PMID: 34164797 Free PMC article. Review.
-
Evaluation of a novel point-of-care lateral flow assay screening for Neisseria gonorrhoeae infection among pregnant women in Zimbabwe.PLOS Glob Public Health. 2025 Feb 11;5(2):e0003839. doi: 10.1371/journal.pgph.0003839. eCollection 2025. PLOS Glob Public Health. 2025. PMID: 39932971 Free PMC article.
References
-
- Newman L, Rowley J, Vander Hoorn S, Wijesooriya NS, Unemo M, Low N, et al. Global Estimates of the Prevalence and Incidence of Four Curable Sexually Transmitted Infections in 2012 Based on Systematic Review and Global Reporting. PLoS One. 2015;10(12):e0143304 10.1371/journal.pone.0143304 - DOI - PMC - PubMed
-
- Wetten S, Mohammed H, Yung M, Mercer CH, Cassell JA, Hughes G. Diagnosis and treatment of chlamydia and gonorrhoea in general practice in England 2000–2011: a population-based study using data from the UK Clinical Practice Research Datalink. BMJ Open. 2015;5(5):e007776 10.1136/bmjopen-2015-007776 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

