Predicting childhood obesity using electronic health records and publicly available data
- PMID: 31009509
- PMCID: PMC6476510
- DOI: 10.1371/journal.pone.0215571
Predicting childhood obesity using electronic health records and publicly available data
Erratum in
-
Correction: Predicting childhood obesity using electronic health records and publicly available data.PLoS One. 2019 Oct 7;14(10):e0223796. doi: 10.1371/journal.pone.0223796. eCollection 2019. PLoS One. 2019. PMID: 31589654 Free PMC article.
Abstract
Background: Because of the strong link between childhood obesity and adulthood obesity comorbidities, and the difficulty in decreasing body mass index (BMI) later in life, effective strategies are needed to address this condition in early childhood. The ability to predict obesity before age five could be a useful tool, allowing prevention strategies to focus on high risk children. The few existing prediction models for obesity in childhood have primarily employed data from longitudinal cohort studies, relying on difficult to collect data that are not readily available to all practitioners. Instead, we utilized real-world unaugmented electronic health record (EHR) data from the first two years of life to predict obesity status at age five, an approach not yet taken in pediatric obesity research.
Methods and findings: We trained a variety of machine learning algorithms to perform both binary classification and regression. Following previous studies demonstrating different obesity determinants for boys and girls, we similarly developed separate models for both groups. In each of the separate models for boys and girls we found that weight for length z-score, BMI between 19 and 24 months, and the last BMI measure recorded before age two were the most important features for prediction. The best performing models were able to predict obesity with an Area Under the Receiver Operator Characteristic Curve (AUC) of 81.7% for girls and 76.1% for boys.
Conclusions: We were able to predict obesity at age five using EHR data with an AUC comparable to cohort-based studies, reducing the need for investment in additional data collection. Our results suggest that machine learning approaches for predicting future childhood obesity using EHR data could improve the ability of clinicians and researchers to drive future policy, intervention design, and the decision-making process in a clinical setting.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


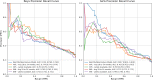
References
-
- Alston JM, Okrent AM. The effects of farm and food policy on obesity in the United States New York, NY, U.S.A.: Palgrave Macmillan; 2017. xxii, 393 pages p.
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

