Radiographic and Histological Analysis of a Synthetic Bone Graft Substitute Eluting Gentamicin in the Treatment of Chronic Osteomyelitis
- PMID: 31011512
- PMCID: PMC6470655
- DOI: 10.7150/jbji.31592
Radiographic and Histological Analysis of a Synthetic Bone Graft Substitute Eluting Gentamicin in the Treatment of Chronic Osteomyelitis
Abstract
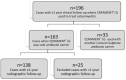
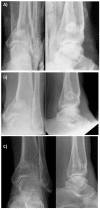
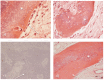
Introduction: Managing chronic osteomyelitis can be challenging and attention to the osseous dead-space left following resection is an important part of successful treatment. We assess radiographic bone healing following implantation of a gentamicin-eluting synthetic bone graft substitute (gBGS) used at chronic osteomyelitis (cOM) resection. We also describe histological carrier changes from biopsies in nine cases at various time points. Methods: This was a retrospective review of a prospectively collected consecutive series of 163 patients with Cierny-Mader Type III or IV cOM who underwent single-stage excision, insertion of gBGS and definitive soft-tissue closure or coverage. Bone defect filling was assessed radiographically using serial radiographs. Nine patients had subsequent surgery, not related to infection recurrence, allowing opportunistic biopsy between 19 days and two years after implantation. Results: Infection was eradicated in 95.7% with a single procedure. 138 patients had adequate radiographs for assessment with minimum one-year follow-up (mean 1.7 years, range 1.0-4.7 years). Mean void-filling at final follow-up was 73.8%. There was significantly higher void-filling in metaphyseal compared to diaphyseal voids (mean 79.0% versus 65.6%; p=0.017) and in cases with good initial interdigitation of the carrier (mean 77.3% versus 68.7%; p=0.021). Bone formation continued for more than two years in almost two-thirds of patients studied (24/38; 63.2%). Histology revealed active biomaterial remodelling. It was osteoconductive with osteoblast recruitment, leading to the formation of osteoid, then woven and lamellar bone on the substrate's surface. Immunohistochemistry demonstrated osteocyte specific markers, dentine matrix protein-1 and podoplanin within the newly formed bone. Conclusion: This antibiotic-loaded biomaterial is effective in managing dead-space in surgically treated cOM with a low infection recurrence rate (4.3%) and good mean bone void-filling (73.8%). The radiographic resolution of the bone defect is associated with bone formation, as supported by histological analysis.
Keywords: bone graft substitute; histology; osteomyelitis; outcome; radiology; treatment.
Conflict of interest statement
Competing Interests: JF, NA and MM declare no competing interests. MD works as Head of Research & Development, Medical and Clinical Affairs for Bonesupport AB.
Figures

References
-
- Cierny G, Mader JT, Penninck JJ. The classic: A clinical staging system for adult osteomyelitis. Clinical Orthopaedics & Related Research. 2003;414:7–24. - PubMed
-
- McNally M, Nagarajah K. Osteomyelitis. Orthopaedics and Trauma. 2010;24(6):416–29.
-
- Walenkamp GH, Vree TOMB, Van Rens TJ. Gentamicin-PMMA beads: Pharmacokinetic and nephrotoxicological study. Clinical Orthopaedics & Related Research. 1986;205:171–83. - PubMed
-
- Dressmann H. Über Knochenplombierung bei höhlenformigen Defekten des Knochens. Beitr Klin Chir. 1892;9:804–810.
LinkOut - more resources
Full Text Sources
Research Materials