Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options
- PMID: 31013941
- PMCID: PMC6514804
- DOI: 10.3390/ijms20081839
Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options
Abstract
Myeloproliferative neoplasms represent a heterogenous group of disorders of the hematopoietic stem cell, with an intrinsic risk of evolution into acute myeloid leukemia. The frequency of leukemic evolution varies according to myeloproliferative neoplasms subtype. It is highest in primary myelofibrosis, where it is estimated to be approximately 10-20% at 10 years, following by polycythemia vera, with a risk of 2.3% at 10 years and 7.9% at 20 years. In essential thrombocythemia, however, transformation to acute myeloid leukemia is considered relatively uncommon. Different factors are associated with leukemic evolution in myeloproliferative neoplasms, but generally include advanced age, leukocytosis, exposure to myelosuppressive therapy, cytogenetic abnormalities, as well as increased number of mutations in genes associated with myeloid neoplasms. The prognosis of these patients is dismal, with a medium overall survival ranging from 2.6-7.0 months. Currently, there is no standard of care for managing the blast phase of these diseases, and no treatment to date has consistently led to prolonged survival and/or hematological remission apart from an allogeneic stem cell transplant. Nevertheless, new targeted agents are currently under development. In this review, we present the current evidence regarding risk factors, molecular characterization, and treatment options for this critical subset of myeloproliferative neoplasms patients.
Keywords: blast phase; mutations; myeloproliferative neoplasms; secondary acute leukemia; targeted therapies.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
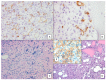
References
-
- Arber D.A., Orazi A., Hasserjian R., Thiele J., Borowitz M.J., Le Beau M.M., Bloomfield C.D., Cazzola M., Vardiman J.W. The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood. 2016;127:2391–2405. doi: 10.1182/blood-2016-03-643544. - DOI - PubMed
-
- Tefferi A., Guglielmelli P., Larson D.R., Finke C., Wassie E.A., Pieri L., Gangat N., Fjerza R., Belachew A.A., Lasho T.L., et al. Long-term survival and blast transformation in molecularly annotated essential thrombocythemia, polycythemia vera, and myelofibrosis. Blood. 2014;124:2507–2513. doi: 10.1182/blood-2014-05-579136. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials

