Role of Procalcitonin as a Predictor of Clinical Outcome in Acute Diabetic Foot Infections: A Prospective Study
- PMID: 31016166
- PMCID: PMC6446684
- DOI: 10.4103/ijem.IJEM_525_18
Role of Procalcitonin as a Predictor of Clinical Outcome in Acute Diabetic Foot Infections: A Prospective Study
Abstract
Background: Prediction of outcome in diabetic foot infection (DFI) remains difficult due to lack of active signs of infection, and apparently normal white blood cell (WBC) count. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) have been studied previously in this regard and were not useful. Hence, we evaluated procalcitonin (PCT) as a prognostic marker in this study.
Objectives: We aimed to study the role of PCT, CRP, and ESR levels in predicting clinical outcome of acute DFI.
Materials and methods: A total of 250 subjects (197 men, 53 women) with acute DFI were enrolled. WBC count, ESR, CRP, and PCT were done for all subjects at admission after obtaining informed consent. Subjects were managed according to hospital protocol and followed up for 1 month. Clinical outcome was assessed based on mobility and morbidity status of the subject.
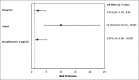
Results: Old age, anemia, hyponatremia, hypoalbuminemia, and elevated serum creatinine were risk factors for poor outcome. Presence of cardiac failure, diabetic retinopathy, peripheral vascular disease, previous amputations, and positive bone culture had negative influence on clinical outcome. Elevated WBC count, ESR, CRP, and serum PCT were significantly associated with bad outcome. Elevated PCT (>2 ng/ml) [odds ratio (OR) (95% confidence interval (CI)), 2.03 (1.13-5.19), P < 0.001], gangrene [OR (95% CI), 2.2 (1.02-4.73), P = 0.04], and sepsis [OR (95% CI), 10.101 (4.34-23.25), P < 0.001] were good predictors of clinical outcome in acute DFI.
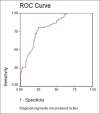
Conclusion: PCT proved to be a reliable marker of acute DFI and good predictor of clinical outcome than existing markers WBC count, ESR, and CRP. Hence it should be useful for clinicians while managing acute DFI.
Keywords: C-reactive protein; diabetic foot infection; erythrocyte sedimentation rate; procalcitonin.
Conflict of interest statement
There are no conflicts of interest.
Figures
Similar articles
-
Procalcitonin as a diagnostic aid in diabetic foot infections.Tohoku J Exp Med. 2007 Dec;213(4):305-12. doi: 10.1620/tjem.213.305. Tohoku J Exp Med. 2007. PMID: 18075234
-
Diagnostic value of procalcitonin, erythrocyte sedimentation rate (ESR), quantitative C-reactive protein (CRP) and clinical findings associated with osteomyelitis in patients with diabetic foot.Hum Antibodies. 2021;29(2):115-121. doi: 10.3233/HAB-210439. Hum Antibodies. 2021. PMID: 33749641
-
[Diagnosis value of serum infection index for early infection of patients undergoing posterior cervical expansive open-door laminoplasty].Zhongguo Gu Shang. 2019 Oct 25;32(10):892-897. doi: 10.3969/j.issn.1003-0034.2019.10.004. Zhongguo Gu Shang. 2019. PMID: 32512957 Chinese.
-
[Clinical significance of PCT, CRP, ESR, WBC count as predictors in postoperative early infectious complications with fever after posterior lumbar internal fixation].Zhongguo Gu Shang. 2015 Jan;28(1):66-70. Zhongguo Gu Shang. 2015. PMID: 25823137 Chinese.
-
Comparison of serum procalcitonin level with erythrocytes sedimentation rate, C-reactive protein, white blood cell count, and blood culture in the diagnosis of bacterial infections in patients hospitalized in Motahhari hospital of Urmia (2016).J Adv Pharm Technol Res. 2018 Oct-Dec;9(4):147-152. doi: 10.4103/japtr.JAPTR_319_18. J Adv Pharm Technol Res. 2018. PMID: 30637233 Free PMC article.
Cited by
-
Procalcitonin and Diabetic Foot Ulcer Infections: A Meta-Analysis.Endocrinol Diabetes Metab. 2025 Jul;8(4):e70066. doi: 10.1002/edm2.70066. Endocrinol Diabetes Metab. 2025. PMID: 40653844 Free PMC article.
-
[Characteristics of Inflammatory Markers in Diabetic Foot Patients and Their Relationship With Prognosis of Diabetic Foot Ulcers].Sichuan Da Xue Xue Bao Yi Xue Ban. 2023 Nov 20;54(6):1233-1238. doi: 10.12182/20230960506. Sichuan Da Xue Xue Bao Yi Xue Ban. 2023. PMID: 38162051 Free PMC article. Chinese.
-
Diabetic Wound-Healing Science.Medicina (Kaunas). 2021 Oct 8;57(10):1072. doi: 10.3390/medicina57101072. Medicina (Kaunas). 2021. PMID: 34684109 Free PMC article. Review.
References
-
- King H, Aubert RE, Herman WH. Global burden of diabetes, 1995-2025: Prevalence, numerical estimates, and projections. Diabetes Care. 1998;21:1414–31. - PubMed
-
- Borssen B, Bergenheim T, Lithner F. The epidemiology of foot lesions in diabetic patients aged 15-50 years. Diabet Med. 1990;7:438–44. - PubMed
-
- Williams DT, Hilton JR, Harding KG. Diagnosing foot infection in diabetes. Clin Infect Dis. 2004;39(Suppl 2):S83–6. - PubMed
-
- Uzun G, Solmazgul E, Curuksulu H, Turhan V. Procalcitonin as a diagnostic aid in diabetic foot infections. Tohoku J Exp Med. 2007;213:305–12. - PubMed
-
- Ramsey SD, Newton K, Blough D, McCulloch DK, Sandhu N, Reiber GE, et al. Incidence, outcomes, and cost of foot ulcers in patients with diabetes. Diabetes Care. 1999;22:382–7. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous