Paediatric focal intracranial suppurative infection: a UK single-centre retrospective cohort study
- PMID: 31023283
- PMCID: PMC6482535
- DOI: 10.1186/s12887-019-1486-7
Paediatric focal intracranial suppurative infection: a UK single-centre retrospective cohort study
Abstract
Background: Paediatric focal intracranial suppurative infections are uncommon but cause significant mortality and morbidity. There are no uniform guidelines regarding antibiotic treatment. This study reviewed management in a tertiary healthcare centre in the United Kingdom and considers suggestions for empirical treatment.
Methods: A retrospective, single-centre cohort review of 95 children (< 18 years of age) with focal intracranial suppurative infection admitted between January 2001 and June 2016 in Newcastle upon Tyne, United Kingdom. Microbiological profiles and empirical antibiotic regimens were analysed for coverage, administration and duration of use. Mortality and neurological morbidity were reviewed. Data was analysed using t-tests, Mann-Whitney U tests, independent-samples median tests, and χ2-tests where appropriate. P-values < 0.05 were considered statistically significant.
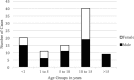
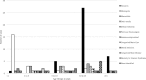
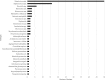
Results: Estimated annual incidence was 8.79 per million. Age was bimodally distributed. Predisposing factors were identified in 90.5%, most commonly sinusitis (42.1%) and meningitis (23.2%). Sinusitis was associated with older children (p < 0.001) and meningitis with younger children (p < 0.001). The classic triad was present in 14.0%. 43.8% of 114 isolates were Streptococcus spp., most commonly Streptococcus milleri group organisms. Twelve patients cultured anaerobes. Thirty one empirical antibiotic regimens were used, most often a third-generation cephalosporin plus metronidazole and amoxicillin (32.2%). 90.5% would have sufficient cover with a third generation cephalosporin plus metronidazole. 66.3% converted to oral antibiotics. Median total antibiotic treatment duration was 90 days (interquartile range, 60-115.50 days). Mortality was 3.2, 38.5% had short-term and 24.2% long-term neurological sequelae.
Conclusions: Paediatric focal intracranial suppurative infection has a higher regional incidence than predicted from national estimates and still causes significant mortality and morbidity. We recommend a third-generation cephalosporin plus metronidazole as first-choice empirical treatment. In infants with negative anaerobic cultures metronidazole may be discontinued.
Keywords: Antimicrobials; Brain abscess; Empyema, subdural; Paediatrics.
Conflict of interest statement
Ethics approval and consent to participate
Local ethical approval and consent for the use of human data was obtained by de Caldicott commission for the Newcastle upon Tyne Hospitals NHS Foundation Trust Reference number: ID: 4738.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Bonfield CM, Sharma J, Dobson S. Pediatric intracranial abscesses. J Inf Secur. 2015;71(Suppl 1):S42–S46. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous