Depression, anxiety, and bodily pain independently predict poor sleep quality among adult women attending a primary health center of Puducherry, India
- PMID: 31041271
- PMCID: PMC6482758
- DOI: 10.4103/jfmpc.jfmpc_118_19
Depression, anxiety, and bodily pain independently predict poor sleep quality among adult women attending a primary health center of Puducherry, India
Abstract
Background: Sleep disorders and mental health problems are common diagnoses in primary care settings. The objective of this study was to estimate the magnitude of poor sleep, depression, and anxiety through opportunistic screening and to find out the independent predictors of poor sleep quality among female participants.
Materials and methods: A hospital-based study was conducted in the outpatient department (OPD) of an urban primary health center of Puducherry. Patients and accompanying healthy attendants ≥ 18 years of age who visited the OPD for any reason were included. Those with serious acute illness, previously diagnosed mental illness, pregnant women, and women in postpartum period (upto 6 weeks) were excluded. Systematic random sampling was used to select the participants. A semi-structured questionnaire was used to collect sociodemographic and clinical details along with the Pittsburgh Sleep Quality Index (PSQI) and the Hospital Anxiety and Depression Scale. Height and weight were also measured.
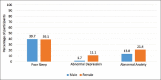
Results: A total of 301 participants were recruited. Mean age of the participants was 49.4 (standard deviation 15.2) years. Magnitude of poor sleep (PSQI score > 5), abnormal anxiety, and abnormal depression were 118 (39.2%), 60 (19.9%), and 28 (9.3%) respectively. Multivariate logistic regression analysis showed that history of pain [odds ratio (OR) 3.2 (1.6-6.5), P = 0.001], abnormal anxiety [OR 2.5 (1.2-5.6), P = 0.021], and abnormal depression [OR 4.3 (1.4-13.2), P = 0.01] independently predicted poor sleep quality among females.
Conclusion: OPD-based opportunistic screening for sleep and mental health problems should be routinely conducted by primary care and family physicians.
Keywords: Anxiety; depression; primary care; screening; sleep.
Conflict of interest statement
There are no conflicts of interest.
Figures
References
-
- Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: Apopulation health perspective. Am J Respir Crit Care Med. 2002;165:1217–39. - PubMed
-
- Netzer NC, Hoegel JJ, Loube D, Netzer CM, Hay B, Alvarez-Sala R, et al. Prevalence of symptoms and risk of sleep apnea in primary care. Chest. 2003;124:1406–14. - PubMed
-
- Hiestand DM, Britz P, Goldman M, Phillips B. Prevalence of symptoms and risk of sleep apnea in the US population: Results from the National Sleep Foundation Sleep in America 2005 poll. Chest. 2006;130:780–6. - PubMed
-
- Lavigne GJ, Montplaisir JY. Restless legs syndrome and sleep bruxism: Prevalence and association among Canadians. Sleep. 1994;17:739–43. - PubMed