Pediatric CNS-isolated hemophagocytic lymphohistiocytosis
- PMID: 31044148
- PMCID: PMC6467688
- DOI: 10.1212/NXI.0000000000000560
Pediatric CNS-isolated hemophagocytic lymphohistiocytosis
Abstract
Objective: To highlight a novel, treatable syndrome, we report 4 patients with CNS-isolated inflammation associated with familial hemophagocytic lymphohistiocytosis (FHL) gene mutations (CNS-FHL).
Methods: Retrospective chart review.
Results: Patients with CNS-FHL are characterized by chronic inflammation restricted to the CNS that is not attributable to any previously described neuroinflammatory etiology and have germline mutations in known FHL-associated genes with no signs of systemic inflammation. Hematopoietic stem cell transplantation (HCT) can be well tolerated and effective in achieving or maintaining disease remission in patients with CNS-FHL.
Conclusions: Early and accurate diagnosis followed by treatment with HCT can reduce morbidity and mortality in CNS-FHL, a novel, treatable syndrome.
Classification of evidence: This study provides Class IV evidence that HCT is well tolerated and effective in treating CNS-FHL.
Figures
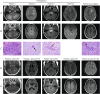
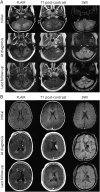
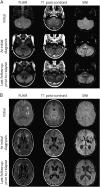
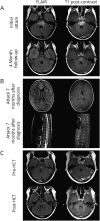
References
-
- Deiva K, Mahlaoui N, Beaudonnet F, et al. CNS involvement at the onset of primary hemophagocytic lymphohistiocytosis. Neurology 2012;78:1150–1156. - PubMed
-
- Horne A, Trottestam H, Aricò M, et al. Frequency and spectrum of central nervous system involvement in 193 children with haemophagocytic lymphohistiocytosis. Br J Haematol 2008;140:327–335. - PubMed
-
- Henter JI, Horne A, Aricó M, et al. HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer 2007;48:124–131. - PubMed
-
- Degar B. Familial hemophagocytic lymphohistiocytosis. Hematol Oncol Clin North Am 2015;29:903–913. - PubMed
-
- Zhang K, Filipovich AH, Johnson J, Marsh RA, Villanueva J. Hemophagocytic lymphohistiocytosis, familial. In: Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews®. Seattle: University of Washington; 1993.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
