Disease progression and treatment response in data-driven subgroups of type 2 diabetes compared with models based on simple clinical features: an analysis using clinical trial data
- PMID: 31047901
- PMCID: PMC6520497
- DOI: 10.1016/S2213-8587(19)30087-7
Disease progression and treatment response in data-driven subgroups of type 2 diabetes compared with models based on simple clinical features: an analysis using clinical trial data
Abstract
Background: Research using data-driven cluster analysis has proposed five subgroups of diabetes with differences in diabetes progression and risk of complications. We aimed to compare the clinical utility of this subgroup-based approach for predicting patient outcomes with an alternative strategy of developing models for each outcome using simple patient characteristics.
Methods: We identified five clusters in the ADOPT trial (n=4351) using the same data-driven cluster analysis as reported by Ahlqvist and colleagues. Differences between clusters in glycaemic and renal progression were investigated and contrasted with stratification using simple continuous clinical features (age at diagnosis for glycaemic progression and baseline renal function for renal progression). We compared the effectiveness of a strategy of selecting glucose-lowering therapy using clusters with one combining simple clinical features (sex, BMI, age at diagnosis, baseline HbA1c) in an independent trial cohort (RECORD [n=4447]).
Findings: Clusters identified in trial data were similar to those described in the original study by Ahlqvist and colleagues. Clusters showed differences in glycaemic progression, but a model using age at diagnosis alone explained a similar amount of variation in progression. We found differences in incidence of chronic kidney disease between clusters; however, estimated glomerular filtration rate at baseline was a better predictor of time to chronic kidney disease. Clusters differed in glycaemic response, with a particular benefit for thiazolidinediones in patients in the severe insulin-resistant diabetes cluster and for sulfonylureas in patients in the mild age-related diabetes cluster. However, simple clinical features outperformed clusters to select therapy for individual patients.
Interpretation: The proposed data-driven clusters differ in diabetes progression and treatment response, but models that are based on simple continuous clinical features are more useful to stratify patients. This finding suggests that precision medicine in type 2 diabetes is likely to have most clinical utility if it is based on an approach of using specific phenotypic measures to predict specific outcomes, rather than assigning patients to subgroups.
Funding: UK Medical Research Council.
Copyright © 2019 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved.
Figures



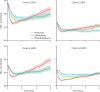

Comment in
-
Predicting individual treatment response in diabetes.Lancet Diabetes Endocrinol. 2019 Jun;7(6):415-417. doi: 10.1016/S2213-8587(19)30118-4. Epub 2019 Apr 29. Lancet Diabetes Endocrinol. 2019. PMID: 31047903 No abstract available.
-
Clusters provide a better holistic view of type 2 diabetes than simple clinical features.Lancet Diabetes Endocrinol. 2019 Sep;7(9):668-669. doi: 10.1016/S2213-8587(19)30257-8. Lancet Diabetes Endocrinol. 2019. PMID: 31439272 No abstract available.
-
Clusters provide a better holistic view of type 2 diabetes than simple clinical features - Authors' reply.Lancet Diabetes Endocrinol. 2019 Sep;7(9):669. doi: 10.1016/S2213-8587(19)30250-5. Lancet Diabetes Endocrinol. 2019. PMID: 31439274 No abstract available.
References
-
- Ahlqvist E, Storm P, Käräjämäki A. Novel subgroups of adult-onset diabetes and their association with outcomes: a data-driven cluster analysis of six variables. Lancet Diabetes Endocrinol. 2018;6:361–369. - PubMed
- E Ahlqvist, P Storm, A Käräjämäki. Novel subgroups of adult-onset diabetes and their association with outcomes: a data-driven cluster analysis of six variables. Lancet Diabetes Endocrinol, 6, 2018, 361–369 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

