Association between cumulative anticholinergic burden and falls and fractures in patients with overactive bladder: US-based retrospective cohort study
- PMID: 31061036
- PMCID: PMC6502005
- DOI: 10.1136/bmjopen-2018-026391
Association between cumulative anticholinergic burden and falls and fractures in patients with overactive bladder: US-based retrospective cohort study
Abstract
Objective: To estimate the association between cumulative anticholinergic burden and falls and fractures in patients with overactive bladder (OAB).
Design: A retrospective claims-based study (2007-2015) of patients with OAB; outcomes from a subset were contrasted to a non-OAB comparison.
Setting: United States, commercially and Medicare-insured population.
Participants: 154 432 adults with OAB and 86 966 adults without OAB, mean age of 56 years, and 67.9% women.
Main outcome measures: Cumulative anticholinergic burden, a unitless value representing exposure over time, was estimated over the 12 months pre-index ('at baseline') and every 6 months post index. Burden was categorised as no burden (0), low burden (1-89), medium burden (90-499) or high burden (500+). Unadjusted rates of falls or fractures were estimated, and the increased risk associated with anticholinergic burden (measured at the closest 6-month interval prior to a fall or fracture) was assessed using a Cox proportional hazards model and a marginal structural model.
Results: Median (IQR) baseline anticholinergic burden was 30 (0.0-314.0) and higher among older (≥65 years, 183 [3.0-713.0]) versus younger (<65 years, 13 [0.0-200.0]) adults. The unadjusted rate of falls or fractures over the period was 5.0 per 100 patient-years, ranging from 3.1 (95% CI 3.0-3.2) for those with no burden, to 7.4 (95% CI 7.1-7.6) for those with high burden at baseline. The adjusted risk of falls and fractures was greater with higher anticholinergic burden in the previous 6 months, with an HR of 1.2 (95% CI 1.2 to 1.3) for low burden versus no burden, to 1.4 (95% CI 1.3 to 1.4) for high versus no burden. Estimates from marginal structural models adjusting for time-varying covariates were lower but remained significantly higher with a higher anticholinergic burden. Rates of falls and fractures were approximately 40% higher among those with OAB (vs those without).
Conclusion: Higher levels of anticholinergic burden are associated with higher rates of falls and fractures, highlighting the importance of considering anticholinergic burden when treating patients with OAB.
Keywords: anticholinergic burden; falls; fractures; marginal structural models; observational study; overactive bladder.
© Author(s) (or their employer(s)) 2019. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE form for Disclosure of Potential Conflicts of Interest (available on request from the corresponding author). SMS, GL-O, AD and BR declare a relevant conflict of interest for the work under consideration for publication as Broadstreet received funding from Astellas for the design and analysis of the data for this study; they declare no conflicts relative to financial activities outside of the submitted work, intellectual property or other relationships not covered. KC, CS and DW declare a relevant conflict of interest to the work under consideration for publication and for relevant financial activities outside of the submitted work as they are employees of Astellas Pharma, the funder of the study, at the time of study completion; they declare no conflicts relative to intellectual property or other relationships not covered. EV declares a relevant conflict of interest for the work under consideration for publication and for relevant financial activities outside of the submitted work as he received personal fees for consultancy for Astellas Pharma, the study funder; he declares no conflicts relative to intellectual property or other relationships not covered. NC declares a relevant conflict of interest for relevant financial activities outside of the submitted work as he received personal fees for consultancy for Astellas Pharma, the study funder; he declares no conflicts relative to the work under consideration for publication, intellectual property or other relationships not covered.
Figures
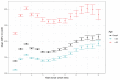

Similar articles
-
The Relationship Between Anticholinergic Exposure and Falls, Fractures, and Mortality in Patients with Overactive Bladder.Drugs Aging. 2019 Oct;36(10):957-967. doi: 10.1007/s40266-019-00694-5. Drugs Aging. 2019. PMID: 31359329
-
Health Resource Utilization and Cost for Patients with Incontinent Overactive Bladder Treated with Anticholinergics.J Manag Care Spec Pharm. 2016 Apr;22(4):406-13. doi: 10.18553/jmcp.2016.22.4.406. J Manag Care Spec Pharm. 2016. PMID: 27023694 Free PMC article.
-
A 12-Year Retrospective Study of the Prevalence of Anticholinergic Polypharmacy and Associated Outcomes Among Medicare Patients with Overactive Bladder in the USA.Drugs Aging. 2021 Dec;38(12):1075-1085. doi: 10.1007/s40266-021-00901-2. Epub 2021 Nov 8. Drugs Aging. 2021. PMID: 34746992 Free PMC article.
-
The Association Between Overactive Bladder and Falls and Fractures: A Systematic Review.Adv Ther. 2018 Nov;35(11):1831-1841. doi: 10.1007/s12325-018-0796-8. Epub 2018 Sep 25. Adv Ther. 2018. PMID: 30255417 Free PMC article.
-
The Differential Risk of Mortality Among Users of Overactive Bladder Anticholinergic Medications and β3 Agonists.Eur Urol Focus. 2023 Jan;9(1):168-171. doi: 10.1016/j.euf.2022.08.002. Epub 2022 Aug 17. Eur Urol Focus. 2023. PMID: 35987891 Review.
Cited by
-
Multicomponent behavioral intervention to reduce exposure to anticholinergics in primary care older adults.J Am Geriatr Soc. 2021 Jun;69(6):1490-1499. doi: 10.1111/jgs.17121. Epub 2021 Mar 26. J Am Geriatr Soc. 2021. PMID: 33772749 Free PMC article. Clinical Trial.
-
Association of a Novel Medication Risk Score with Adverse Drug Events and Other Pertinent Outcomes Among Participants of the Programs of All-Inclusive Care for the Elderly.Pharmacy (Basel). 2020 May 20;8(2):87. doi: 10.3390/pharmacy8020087. Pharmacy (Basel). 2020. PMID: 32443719 Free PMC article.
-
Increased risk of incident dementia following use of anticholinergic agents: A systematic literature review and meta-analysis.Neurourol Urodyn. 2021 Jan;40(1):28-37. doi: 10.1002/nau.24536. Epub 2020 Oct 23. Neurourol Urodyn. 2021. PMID: 33098213 Free PMC article.
-
Development and Delphi consensus validation of the Medication-Related Fall screening and scoring tool.Int J Clin Pharm. 2024 Aug;46(4):977-986. doi: 10.1007/s11096-024-01734-w. Epub 2024 May 16. Int J Clin Pharm. 2024. PMID: 38753075 Free PMC article.
-
Association of lower urinary tract symptoms and hip fracture in adults aged ≥ 50 years.PLoS One. 2021 Mar 3;16(3):e0246653. doi: 10.1371/journal.pone.0246653. eCollection 2021. PLoS One. 2021. PMID: 33657118 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
