CAFs secreted exosomes promote metastasis and chemotherapy resistance by enhancing cell stemness and epithelial-mesenchymal transition in colorectal cancer
- PMID: 31064356
- PMCID: PMC6503554
- DOI: 10.1186/s12943-019-1019-x
CAFs secreted exosomes promote metastasis and chemotherapy resistance by enhancing cell stemness and epithelial-mesenchymal transition in colorectal cancer
Abstract
Background: Cancer associated fibroblasts (CAFs) are key stroma cells that play dominant roles in tumor progression. However, the CAFs-derived molecular determinants that regulate colorectal cancer (CRC) metastasis and chemoresistance have not been fully characterized.
Methods: CAFs and NFs were obtained from fresh CRC and adjacent normal tissues. Exosomes were isolated from conditioned medium and serum of CRC patients using ultracentrifugation method and ExoQuick Exosome Precipitation Solution kit, and characterized by transmission electronic microscopy, nanosight and western blot. MicroRNA microarray was employed to identify differentially expressed miRNAs in exosomes secreted by CAFs or NFs. The internalization of exosomes, transfer of miR-92a-3p was observed by immunofluorescence. Boyden chamber migration and invasion, cell counting kit-8, flow cytometry, plate colony formation, sphere formation assays, tail vein injection and primary colon cancer liver metastasis assays were employed to explore the effect of NFs, CAFs and exosomes secreted by them on epithelial-mesenchymal transition, stemness, metastasis and chemotherapy resistance of CRC. Luciferase report assay, real-time qPCR, western blot, immunofluorescence, and immunohistochemistry staining were employed to explore the regulation of CRC metastasis and chemotherapy resistance by miR-92a-3p, FBXW7 and MOAP1.
Results: CAFs promote the stemness, epithelial-mesenchymal transition (EMT), metastasis and chemotherapy resistance of CRC cells. Importantly, CAFs exert their roles by directly transferring exosomes to CRC cells, leading to a significant increase of miR-92a-3p level in CRC cells. Mechanically, increased expression of miR-92a-3p activates Wnt/β-catenin pathway and inhibits mitochondrial apoptosis by directly inhibiting FBXW7 and MOAP1, contributing to cell stemness, EMT, metastasis and 5-FU/L-OHP resistance in CRC. Clinically, miR-92a-3p expression is significantly increased in CRC tissues and negatively correlated with the levels of FBXW7 and MOAP1 in CRC specimens, and high expression of exosomal miR-92a-3p in serum was highly linked with metastasis and chemotherapy resistance in CRC patients.
Conclusions: CAFs secreted exosomes promote metastasis and chemotherapy resistance of CRC. Inhibiting exosomal miR-92a-3p provides an alternative modality for the prediction and treatment of metastasis and chemotherapy resistance in CRC.
Keywords: Chemotherapy resistance; Colorectal cancer; Exosomes; Metastasis; Stemness; miR-92a-3p.
Conflict of interest statement
Ethics approval and consent to participate
Informed consent was obtained to bank CRC tissues and serum for research purposes. The collection of CRC tissues and serum for research purposes was approved by the Ethics Committee of the Nanfang Hospital. All animal experiments were conducted in accordance with the principles and procedures approved by the Committee on the Ethics of Animal Experiments of Southern Medical University.
Consent for publication
All authors reached an agreement to publish the study in this journal.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
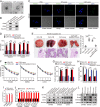






References
-
- Tournigand C, Andre T, Achille E, Lledo G, Flesh M, Mery-Mignard D, Quinaux E, Couteau C, Buyse M, Ganem G, et al. FOLFIRI followed by FOLFOX6 or the reverse sequence in advanced colorectal cancer: a randomized GERCOR study. J Clin Oncol. 2004;22:229–237. doi: 10.1200/JCO.2004.05.113. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

