Moderators of Response to Cognitive Behavior Therapy for Major Depression in Patients With Heart Failure
- PMID: 31083052
- PMCID: PMC6919214
- DOI: 10.1097/PSY.0000000000000712
Moderators of Response to Cognitive Behavior Therapy for Major Depression in Patients With Heart Failure
Erratum in
-
Moderators of Response to Cognitive Behavior Therapy for Major Depression in Patients With Heart Failure: Erratum.Psychosom Med. 2019 Sep;81(7):674. doi: 10.1097/PSY.0000000000000738. Psychosom Med. 2019. PMID: 31460968 No abstract available.
Abstract
Objective: Although cognitive behavior therapy (CBT) is efficacious for major depression in patients with heart failure (HF), approximately half of patients do not remit after CBT. To identify treatment moderators that may help guide treatment allocation strategies and serve as new treatment targets, we performed a secondary analysis of a randomized clinical trial. Based on evidence of their prognostic relevance, we evaluated whether clinical and activity characteristics moderate the effects of CBT.
Methods: Participants were randomized to enhanced usual care (UC) alone or CBT plus enhanced UC. The single-blinded outcomes were 6-month changes in Beck Depression Inventory total scores and remission (defined as a Beck Depression Inventory ≤ 9). Actigraphy was used to assess daily physical activity patterns. We performed analyses to identify the specific activity and clinical moderators of the effects of CBT in 94 adults (mean age = 58, 49% female) with HF and major depressive disorder.
Results: Patients benefited more from CBT (versus UC) if they had the following: more medically severe HF (i.e., a higher New York Heart Association class or a lower left ventricular ejection fraction), more stable activity patterns, wider active periods, and later evening settling times. These individual moderator effects were small (|r| = 0.10-0.21), but combining the moderators yielded a medium moderator effect size (r = 0.38; 95% CI = 0.20-0.52).
Conclusions: These findings suggest that increasing the cross-daily stability of activity patterns, and prolonging the daily active period, might help increase the efficacy of CBT. Given moderating effects of HF severity measures, research is also needed to clarify and address factors in patients with less severe HF that diminish the efficacy of CBT.
Clinical trial registration: clinicaltrials.gov identifier: NCT01028625.
Figures

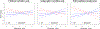

Comment in
-
Extending Behavioral Medicine to Heart Failure With Preserved Ejection Fraction.Psychosom Med. 2020 Apr;82(3):345-346. doi: 10.1097/PSY.0000000000000783. Psychosom Med. 2020. PMID: 32150010 Free PMC article. No abstract available.
References
-
- Koenig HG. Depression in hospitalized older patients with congestive heart failure. General hospital psychiatry 1998;20(1):29–43. - PubMed
-
- Freedland KE, Rich MW, Skala JA, Carney RM, Davila-Roman VG, Jaffe AS. Prevalence of depression in hospitalized patients with congestive heart failure. Psychosomatic medicine 2003;65(1):119–128. - PubMed
-
- O’Connor CM, Jiang W, Kuchibhatla M, et al. Safety and efficacy of sertraline for depression in patients with heart failure: results of the SADHART-CHF (Sertraline Against Depression and Heart Disease in Chronic Heart Failure) trial. Journal of the American College of Cardiology 2010;56(9):692–699. - PMC - PubMed
-
- Angermann CE, Gelbrich G, Stork S, et al. Effect of Escitalopram on All-Cause Mortality and Hospitalization in Patients With Heart Failure and Depression: The MOOD-HF Randomized Clinical Trial. Jama 2016;315(24):2683–2693. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

