Discrimination of ventricular tachycardia and localization of its exit site using surface electrocardiography
- PMID: 31105757
- PMCID: PMC6503474
- DOI: 10.11909/j.issn.1671-5411.2019.04.008
Discrimination of ventricular tachycardia and localization of its exit site using surface electrocardiography
Abstract
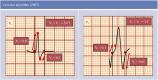
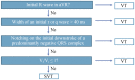
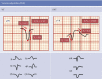
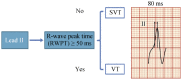
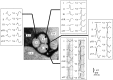
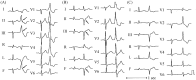
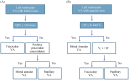
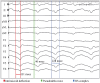
Differential diagnosis of supraventricular tachycardia (SVT) and ventricular tachycardia (VT) is of paramount importance for appropriate patient management. Several diagnostic algorithms for discrimination of VT and SVT based on surface electrocardiogram (ECG) analysis have been proposed. Following established diagnosis of VT, a specific origination tachycardia site can be supposed according to QRS complex characteristics. This review aims to cover comprehensive and comparative description of the main VT diagnostic algorithms and to present ECG characteristics which permit to suggest the most common VT origination sites.
Keywords: Arrhythmias; Electrocardiogram; Supraventricular; Tachycardia; Ventricular.
Figures










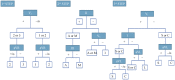
References
-
- Blomström-Lundqvist C, Scheinman MM, Aliot EM, et al. Writing Committee to Develop Guidelines for the Management of Patients With Supraventricular A. ACC/AHA/ESC guidelines for the management of patients with supraventricular arrhythmias-executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Supraventricular Arrhythmias) Circulation. 2003;108:1871–1909. - PubMed
-
- Katritsis DG, Boriani G, Cosio FG, et al. European Heart Rhythm Association (EHRA) consensus document on the management of supraventricular arrhythmias, endorsed by Heart Rhythm Society (HRS), Asia-Pacific Heart Rhythm Society (APHRS), and Sociedad Latinoamericana de Estimulacion Cardiaca y Electrofisiologia (SOLAECE) Europace. 2017;19:465–511. - PubMed
-
- Cohen HC, Gozo EG, Jr, Pick A. Ventricular Tachycardia with narrow QRS complexes (left posterior fascicular tachycardia) Circulation. 1972;45:1035–1043. - PubMed
-
- Lebedev DS. Wide QRS tachycardia: differential diagnosis and treatment. J Arrhythmol. 1998;7:65–73.
-
- Brugada P, Brugada J, Mont L, et al. A new approach to the differential diagnosis of a regular tachycardia with a wide QRS complex. Circulation. 1991;83:1649–1659. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
