Effects of Positive End-Expiratory Pressure on Pulmonary Oxygenation and Biventricular Function during One-Lung Ventilation: A Randomized Crossover Study
- PMID: 31126111
- PMCID: PMC6571862
- DOI: 10.3390/jcm8050740
Effects of Positive End-Expiratory Pressure on Pulmonary Oxygenation and Biventricular Function during One-Lung Ventilation: A Randomized Crossover Study
Abstract
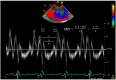
Although the application of positive end-expiratory pressure (PEEP) can alter cardiopulmonary physiology during one-lung ventilation (OLV), these changes have not been clearly elucidated. This study assessed the effects of different levels of PEEP on biventricular function, as well as pulmonary oxygenation during OLV. Thirty-six lung cancer patients received one PEEP combination of six sequences, consisting of 0 (PEEP_0), 5 (PEEP_5), and 10 cmH2O (PEEP_10), using a crossover design during OLV. The ratio of arterial oxygen partial pressure to inspired oxygen fraction (P/F ratio), systolic and diastolic echocardiographic parameters were measured at 20 min after the first, second, and third PEEP. P/F ratio at PEEP_5 was significantly higher compared to PEEP_0 (p = 0.014), whereas the P/F ratio at PEEP_10 did not show significant differences compared to PEEP_0 or PEEP_5. Left ventricular ejection fraction (LV EF) and right ventricular fractional area change (RV FAC) at PEEP_10 (EF, p < 0.001; FAC, p = 0.001) were significantly lower compared to PEEP_0 or PEEP_5. RV E/E' (p = 0.048) and RV myocardial performance index (p < 0.001) at PEEP_10 were significantly higher than those at PEEP_0 or PEEP_5. In conclusion, increasing PEEP to 10 cmH2O decreased biventricular function, especially on RV function, with no further improvement on oxygenation compared to PEEP 5 cmH2O during OLV.
Keywords: biventricular function; one-lung ventilation; positive end-expiratory pressure; pulmonary oxygenation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
A randomized controlled trial of positive end-expiratory pressure on pulmonary oxygenation and biventricular function in esophageal cancer patients receiving one-lung ventilation under a lower FiO2.J Gastrointest Oncol. 2022 Oct;13(5):2105-2114. doi: 10.21037/jgo-22-522. J Gastrointest Oncol. 2022. PMID: 36388664 Free PMC article.
-
Effects of positive end-expiratory pressure on regional cerebral oxygen saturation in elderly patients undergoing thoracic surgery during one-lung ventilation: a randomized crossover-controlled trial.BMC Pulm Med. 2024 Mar 6;24(1):120. doi: 10.1186/s12890-024-02931-z. BMC Pulm Med. 2024. PMID: 38448844 Free PMC article. Clinical Trial.
-
The impact of positive end-expiratory pressure on right ventricular function in patients with moderate-to-severe ARDS: a prospective paired-design study.Front Med (Lausanne). 2024 Jul 2;11:1424090. doi: 10.3389/fmed.2024.1424090. eCollection 2024. Front Med (Lausanne). 2024. PMID: 39015782 Free PMC article.
-
Arterial oxygenation and shunt fraction during one-lung ventilation: a comparison of isoflurane and sevoflurane.Anesth Analg. 1998 Jun;86(6):1266-70. doi: 10.1097/00000539-199806000-00025. Anesth Analg. 1998. PMID: 9620517 Clinical Trial.
-
The effect of incremental positive end-expiratory pressure on right ventricular hemodynamics and ejection fraction.Anesth Analg. 1988 Feb;67(2):144-51. Anesth Analg. 1988. PMID: 3277479 Review.
Cited by
-
A randomized controlled trial of positive end-expiratory pressure on pulmonary oxygenation and biventricular function in esophageal cancer patients receiving one-lung ventilation under a lower FiO2.J Gastrointest Oncol. 2022 Oct;13(5):2105-2114. doi: 10.21037/jgo-22-522. J Gastrointest Oncol. 2022. PMID: 36388664 Free PMC article.
-
Effects of positive end-expiratory pressure on regional cerebral oxygen saturation in elderly patients undergoing thoracic surgery during one-lung ventilation: a randomized crossover-controlled trial.BMC Pulm Med. 2024 Mar 6;24(1):120. doi: 10.1186/s12890-024-02931-z. BMC Pulm Med. 2024. PMID: 38448844 Free PMC article. Clinical Trial.
-
Comparison between Sugammadex and Neostigmine after Video-Assisted Thoracoscopic Surgery-Thymectomy in Patients with Myasthenia Gravis: A Single-Center Retrospective Exploratory Analysis.J Pers Med. 2023 Sep 15;13(9):1380. doi: 10.3390/jpm13091380. J Pers Med. 2023. PMID: 37763148 Free PMC article.
References
-
- Ferrando C., Mugarra A., Gutierrez A., Carbonell J.A., Garcia M., Soro M., Tusman G., Belda F.J. Setting individualized positive end-expiratory pressure level with a positive end-expiratory pressure decrement trial after a recruitment maneuver improves oxygenation and lung mechanics during one-lung ventilation. Anesth. Analg. 2014;118:657–665. doi: 10.1213/ANE.0000000000000105. - DOI - PubMed
LinkOut - more resources
Full Text Sources

