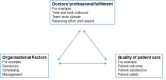
How do doctors experience the interactions among professional fulfilment, organisational factors and quality of patient care? A qualitative study in a Norwegian hospital
- PMID: 31129585
- PMCID: PMC6537988
- DOI: 10.1136/bmjopen-2018-026971
How do doctors experience the interactions among professional fulfilment, organisational factors and quality of patient care? A qualitative study in a Norwegian hospital
Abstract
Objectives: Doctors increasingly experience high levels of burnout and loss of engagement. To address this, there is a need to better understand doctors' work situation. This study explores how doctors experience the interactions among professional fulfilment, organisational factors and quality of patient care.
Design: An exploratory qualitative study design with semistructured individual interviews was chosen. Interviews were transcribed verbatim and analysed by a transdisciplinary research group.
Setting: The study focused on a surgical department of a mid-sized hospital in Norway.
Participants: Seven doctors were interviewed. A purposeful sampling was used with gender and seniority as selection criteria. Three senior doctors (two female, one male) and four in training (three male, one female) were interviewed.
Results: We found that in order to provide quality care to the patients, individual doctors described 'stretching themselves', that is, handling the tensions between quantity and quality, to overcome organisational shortcomings. Experiencing a workplace emphasis on production numbers and budget concerns led to feelings of estrangement among the doctors. Participants reported a shift from serving as trustworthy, autonomous professionals to becoming production workers, where professional identity was threatened. They felt less aligned with workplace values, in addition to experiencing limited management recognition for quality of patient care. Management initiatives to include doctors in development of organisational policies, processes and systems were sparse.
Conclusion: The interviewed doctors described their struggle to balance the inherent tension among professional fulfilment, organisational factors and quality of patient care in their everyday work. They communicated how 'stretching themselves', to overcome organisational shortcomings, is no longer a feasible strategy without compromising both professional fulfilment and quality of patient care. Managers need to ensure that doctors are involved when developing organisational policies, processes and systems. This is likely to be beneficial for both professional fulfilment and quality of patient care.
Keywords: ethics (see medical ethics); preventive medicine; qualitative research.
© Author(s) (or their employer(s)) 2019. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures
References
-
- Trockel M, Bohman B, Lesure E, et al. A brief instrument to assess both burnout and professional fulfillment in physicians: reliability and validity, including correlation with self-reported medical errors, in a sample of resident and practicing physicians. Acad Psychiatry 2018;42:11–24. 10.1007/s40596-017-0849-3 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources