Effects of ATP administration on isolated swine hearts: Implications for ex vivo perfusion and cardiac transplantation
- PMID: 31132883
- PMCID: PMC6690142
- DOI: 10.1177/1535370219850786
Effects of ATP administration on isolated swine hearts: Implications for ex vivo perfusion and cardiac transplantation
Abstract
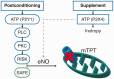
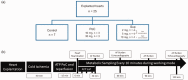
Cardiac transplant outcomes can be compromised by the effects of global ischemia and associated reperfusion injury. In attempts to alleviate these phenomena, various pharmaceutical agents can be administered. Previous reports have shown that adenosine triphosphate (ATP) may act as either a postconditioning (PoC) or supplementary (Sup) therapy with cardiosupportive benefits. To further evaluate ATP’s relative effectiveness, we used an isolated swine heart four-chamber working model to monitor both hemodynamic and metabolic responses. We employed two strategies of ATP administration: (1) a postconditional (PoC) bolus just prior to reanimation, and (2) regular dosing throughout the assessment period (Sup). Ex vivo swine hearts in the Sup group elicited significantly higher left ventricular function during the 2 h monitoring period than controls. In contrast, PoC administration appeared to induce depressed cardiac function. The effects of ATP on cardiac function can have varied effects, dependent on when it is administered.
Impact statement: We employed an isolated swine heart four-chamber working model to investigate two potential strategies for adenosine triphosphate (ATP) administration as an ex vivo therapy: (1) application of a single bolus dose during reperfusion (postconditioning or PoC), and (2) repeated bolus dosing throughout the experiment (supplementary or Sup). Ex vivo swine hearts in the Sup group elicited significantly higher left ventricular function during the 2 h experimental monitoring period. In contrast, ATP administration in the PoC group appeared to induce a degree of depressed hemodynamic function. These data suggest varied functional roles of ATP administration relative to their use in ex vivo perfusion strategies. We consider that both treatment strategies, if appropriately administered and with further investigation of dosing paradigms, may eventually elicit value in various clinical scenarios, including heart transplantation and ex vivo heart perfusion to assess potential organs for transplantation and potentially increase the pool of viable donor hearts.
Keywords: perfusion; ATP supplementation; Pharmacologic cardioprotection; adenosine triphosphate; postconditioning; transplantation.
Figures
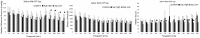
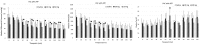
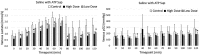
References
-
- Yellon DM, Hausenloy DJ. Myocardial reperfusion injury. N Engl J Med 2007; 357:1121–35 - PubMed
-
- Howard BT, Iles TL, Coles JA, Sigg DC, Iaizzo PA. Reversible and irreversible damage of the myocardium: ischemia/reperfusion injury and cardioprotection In: Iaizzo PA. (ed) Handbook of cardiac anatomy, physiology, and devices. 3rd ed Basel: Springer International Publishing, 2015, pp. 279–93
-
- Murry CE, Jennings RB, Reimer KA. Preconditioning with ischemia: injury delay of lethal cell in ischemic myocardium. Circulation 1986; 74:1124–36 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

