Long-Term Outcomes of Mechanical Thrombectomy for Stroke: A Meta-Analysis
- PMID: 31186620
- PMCID: PMC6521543
- DOI: 10.1155/2019/7403104
Long-Term Outcomes of Mechanical Thrombectomy for Stroke: A Meta-Analysis
Abstract
Mechanical thrombectomy (MT) has become the standard treatment for large vessel occlusion (LVO) in acute ischemic stroke (AIS). Few studies have investigated long-term outcomes for AIS treated with MT. Therefore, a pooled meta-analysis using data from randomized clinical trials (RCT) was performed to assess for long-term clinical outcomes. A systematic literature search was conducted on 27 September 2017, by searching the English literature in the Cochrane Library, MEDLINE, and Embase for RCTs investigating long-term outcomes (greater than standard 3-month timepoint) of endovascular intervention versus medical management for patients with AIS. The study was carried out according to PRISMA guidelines and random effects analysis was carried out to account for heterogeneity. Three trials were included: IMS III, MR CLEAN, and REVASCAT, comprising a total of 1,362 patients. Long-term clinical outcomes were available for 1-year follow-up in IMS III and REVASCAT and at 2 years in MR CLEAN. Functional independence at long-term follow-up favored endovascular stroke intervention (OR 1.51; p = 0.02). When stratified by LVO inclusion criteria, greater endovascular functional independence benefits were observed (OR 1.85; p = 0.0005). There was a significant difference between the 2 arms in favor of endovascular therapy for the quality of life at long-term follow-up (mean difference 0.11; p = 0.0002). No difference in mortality at long-term follow-up was observed (OR 0.82; p = 0.12). We conclude that endovascular therapy results in favorable outcomes at long-term follow-up for patients with acute ischemic stroke compared to standard medical treatment alone and that the 90-day timepoint offers a fair representation of the long-term outcomes.
Figures
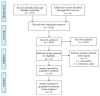

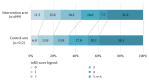

References
-
- Mozaffarian D., Benjamin E. J., Go A. S., et al. Heart disease and stroke statistics--2015 update: a report from the American heart association. Circulation. 2015;131(4):e229–e322. - PubMed
-
- Lee K.-Y., Han S. W., Kim S. H., et al. Early recanalization after intravenous administration of recombinant tissue plasminogen activator as assessed by pre- and post-thrombolytic angiography in acute ischemic stroke patients. Stroke. 2007;38(1):192–193. doi: 10.1161/01.STR.0000251788.03914.00. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

