Wearable Finger Pulse Oximetry for Continuous Oxygen Saturation Measurements During Daily Home Routines of Patients With Chronic Obstructive Pulmonary Disease (COPD) Over One Week: Observational Study
- PMID: 31199331
- PMCID: PMC6594211
- DOI: 10.2196/12866
Wearable Finger Pulse Oximetry for Continuous Oxygen Saturation Measurements During Daily Home Routines of Patients With Chronic Obstructive Pulmonary Disease (COPD) Over One Week: Observational Study
Abstract
Background: Chronic obstructive pulmonary disease (COPD) patients can suffer from low blood oxygen concentrations. Peripheral blood oxygen saturation (SpO2), as assessed by pulse oximetry, is commonly measured during the day using a spot check, or continuously during one or two nights to estimate nocturnal desaturation. Sampling at this frequency may overlook natural fluctuations in SpO2.
Objective: This study used wearable finger pulse oximeters to continuously measure SpO2 during daily home routines of COPD patients and assess natural SpO2 fluctuations.
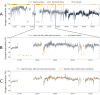
Methods: A total of 20 COPD patients wore a WristOx2 pulse oximeter for 1 week to collect continuous SpO2 measurements. A SenseWear Armband simultaneously collected actigraphy measurements to provide contextual information. SpO2 time series were preprocessed and data quality was assessed afterward. Mean SpO2, SpO2 SD, and cumulative time spent with SpO2 below 90% (CT90) were calculated for every (1) day, (2) day in rest, and (3) night to assess SpO2 fluctuations.
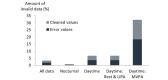
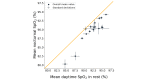
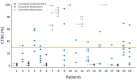
Results: A high percentage of valid SpO2 data (daytime: 93.27%; nocturnal: 99.31%) could be obtained during a 7-day monitoring period, except during moderate-to-vigorous physical activity (MVPA) (67.86%). Mean nocturnal SpO2 (89.9%, SD 3.4) was lower than mean daytime SpO2 in rest (92.1%, SD 2.9; P<.001). On average, SpO2 in rest ranged over 10.8% (SD 4.4) within one day. Highly varying CT90 values between different nights led to 50% (10/20) of the included patients changing categories between desaturator and nondesaturator over the course of 1 week.
Conclusions: Continuous SpO2 measurements with wearable finger pulse oximeters identified significant SpO2 fluctuations between and within multiple days and nights of patients with COPD. Continuous SpO2 measurements during daily home routines of patients with COPD generally had high amounts of valid data, except for motion artifacts during MVPA. The identified fluctuations can have implications for telemonitoring applications that are based on daily SpO2 spot checks. CT90 values can vary greatly from night to night in patients with a nocturnal mean SpO2 around 90%, indicating that these patients cannot be consistently categorized as desaturators or nondesaturators. We recommend using wearable sensors for continuous SpO2 measurements over longer time periods to determine the clinical relevance of the identified SpO2 fluctuations.
Keywords: COPD; finger pulse oximeter; nocturnal desaturation; oxygen saturation; telemonitoring; wearable sensor.
©Joren Buekers, Jan Theunis, Patrick De Boever, Anouk W Vaes, Maud Koopman, Eefje VM Janssen, Emiel FM Wouters, Martijn A Spruit, Jean-Marie Aerts. Originally published in JMIR Mhealth and Uhealth (http://mhealth.jmir.org), 06.06.2019.
Conflict of interest statement
Conflicts of Interest: MAS discloses receipt of renumeration for consultancy and/or lectures from Boehringer Ingelheim, GlaxoSmithKline, and AstraZeneca outside the scope of this work. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript, apart from those disclosed.
Figures

References
-
- Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease: 2019 Report. Fontana, WI: Global Initiative for Chronic Obstructive Lung Disease (GOLD); 2019. [2019-04-16]. https://goldcopd.org/wp-content/uploads/2018/11/GOLD-2019-v1.7-FINAL-14N... .
-
- World Health Organization. 2019. [2018-11-13]. Chronic obstructive pulmonary disease (COPD) http://www.who.int/respiratory/copd/en/
-
- Casanova C, Hernández MC, Sánchez A, García-Talavera I, de Torres JP, Abreu J, Valencia JM, Aguirre-Jaime A, Celli BR. Twenty-four-hour ambulatory oximetry monitoring in COPD patients with moderate hypoxemia. Respir Care. 2006 Dec;51(12):1416–1423. http://www.rcjournal.com/contents/12.06/12.06.1416.pdf - PubMed
-
- Lacasse Y, Sériès F, Vujovic-Zotovic N, Goldstein R, Bourbeau J, Lecours R, Aaron SD, Maltais F. Evaluating nocturnal oxygen desaturation in COPD--revised. Respir Med. 2011 Sep;105(9):1331–1337. doi: 10.1016/j.rmed.2011.04.003. https://linkinghub.elsevier.com/retrieve/pii/S0954-6111(11)00115-6 S0954-6111(11)00115-6 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

