The role of wearable devices and objective gait analysis for the assessment and monitoring of patients with lumbar spinal stenosis: systematic review
- PMID: 31202276
- PMCID: PMC6570936
- DOI: 10.1186/s12891-019-2663-4
The role of wearable devices and objective gait analysis for the assessment and monitoring of patients with lumbar spinal stenosis: systematic review
Abstract
Background: The purpose of this systematic review was to evaluate the accuracy and reliability of wearable devices for objective gait measurement of Lumbar Spinal Stenosis (LSS) patients, with a focus on relevant gait metrics.
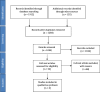
Methods: Systematic searches were conducted of five electronic databases to identify studies that assessed gait metrics by wearable or portable technology. Data was collected according to the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) statement guidelines.
Results: Four articles were identified for inclusion in this review. The objectives, methodology and quality of the studies varied. No single gait metric was investigated in all four studies, making comparison difficult. The most relevant metrics reported included gait cycle, gait velocity, step length and cadence, which were reported in two studies. Two studies explored gait symmetry. Differences between LSS patients and normal healthy subjects are demonstrable using wearable technology.
Conclusions: The measurements of gait cycle, cadence, step length, gait velocity, and number of steps with wearable devices can be used in the gait measurement of LSS patients for initial assessment, and objective outcomes following interventions. However, data and analysis are limited, and further studies are necessary to comment on reliability.
Keywords: Gait assessment; Gait metrics; Lumbar spinal stenosis; Wearables.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Analysis of Patterns of Gait Deterioration in Patients with Lumbar Spinal Stenosis.World Neurosurg. 2020 Sep;141:e55-e59. doi: 10.1016/j.wneu.2020.04.146. Epub 2020 May 7. World Neurosurg. 2020. PMID: 32387784
-
Analysing Gait Patterns in Degenerative Lumbar Spine Disease Using Inertial Wearable Sensors: An Observational Study.World Neurosurg. 2022 Jul;163:e501-e515. doi: 10.1016/j.wneu.2022.04.013. Epub 2022 Apr 8. World Neurosurg. 2022. PMID: 35398575
-
Clinical Gait Evaluation of Patients with Lumbar Spine Stenosis.Orthop Surg. 2018 Feb;10(1):32-39. doi: 10.1111/os.12367. Epub 2018 Feb 12. Orthop Surg. 2018. PMID: 29430858 Free PMC article.
-
The role of wearables in spinal posture analysis: a systematic review.BMC Musculoskelet Disord. 2019 Feb 8;20(1):55. doi: 10.1186/s12891-019-2430-6. BMC Musculoskelet Disord. 2019. PMID: 30736775 Free PMC article.
-
Psychometric properties of wearable technologies to assess post-stroke gait parameters: A systematic review.Gait Posture. 2024 Sep;113:543-552. doi: 10.1016/j.gaitpost.2024.08.004. Epub 2024 Aug 8. Gait Posture. 2024. PMID: 39178597
Cited by
-
Commercial Postural Devices: A Review.Sensors (Basel). 2019 Nov 23;19(23):5128. doi: 10.3390/s19235128. Sensors (Basel). 2019. PMID: 31771130 Free PMC article. Review.
-
Inter-bout and intra-bout gait variability-proposed objective measures of gait deterioration during prolonged walking in spine care.J Spine Surg. 2022 Mar;8(1):180-184. doi: 10.21037/jss-21-88. J Spine Surg. 2022. PMID: 35441111 Free PMC article. No abstract available.
-
Proposed objective scoring algorithm for walking performance, based on relevant gait metrics: the Simplified Mobility Score (SMoS™)-observational study.J Orthop Surg Res. 2021 Jul 1;16(1):419. doi: 10.1186/s13018-021-02546-8. J Orthop Surg Res. 2021. PMID: 34210345 Free PMC article.
-
Development of a Gait Feature-Based Model for Classifying Cognitive Disorders Using a Single Wearable Inertial Sensor.Neurology. 2023 Jul 4;101(1):e12-e19. doi: 10.1212/WNL.0000000000207372. Epub 2023 May 15. Neurology. 2023. PMID: 37188539 Free PMC article.
-
Gait velocity (walking speed) is an indicator of spine health, and objective measure of pre and post intervention recovery for spine care providers.J Spine Surg. 2020 Jun;6(2):353-355. doi: 10.21037/jss-20-602. J Spine Surg. 2020. PMID: 32656370 Free PMC article. No abstract available.
References
-
- Mobbs RJ, Li J, Sivabalan P, Raley D, PJJJoNS R. Outcomes after decompressive laminectomy for lumbar spinal stenosis: comparison between minimally invasive unilateral laminectomy for bilateral decompression and open laminectomy. J Neurosurg Spine. 2014;21(2):179–186. doi: 10.3171/2014.4.SPINE13420. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical