Mobile Spinal Schwannoma with a Completely Cystic Appearance
- PMID: 31204384
- PMCID: PMC6590268
- DOI: 10.12659/AJCR.916249
Mobile Spinal Schwannoma with a Completely Cystic Appearance
Abstract
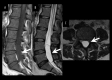
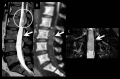
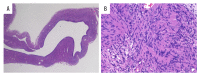
BACKGROUND Spinal schwannomas are benign tumors arising from Schwann cells. Although they have been well described, tumor movement in the spinal canal is an extremely rare finding, and entirely cystic spinal schwannomas have rarely been reported. This is the first report of a spinal schwannoma that simultaneously exhibited both these unusual features. CASE REPORT A 48-year-old female presented with dysuria and right leg pain. Initial magnetic resonance imaging (MRI) revealed a well-delineated intradural cystic lesion at the level of L4-S1 vertebrae that was isointense with cerebrospinal fluid on both T1- and T2-weighted images. A follow-up MRI 6 months later showed that the tumor had moved to the level of L2-L4; it also revealed tortuous configuration of nerve roots of the cauda equina. The tumor was resected, and a diagnosis of schwannoma with extensive cystic degeneration was pathologically confirmed. CONCLUSIONS Various possible mechanisms have been suggested for the mobility of extramedullary tumors. In the present case, MRI findings indicated the cause of the tumor movement might be attributed to the laxity of nerve roots. Besides, it is highly atypical for a schwannoma to present an entirely cystic appearance, and the combination of the 2 extraordinary features made preoperative diagnosis difficult. However, 16 out of 22 (73%) of previously reported mobile spinal tumors were schwannomas, so the differential diagnosis for a mobile spinal tumor should include schwannoma, even when the lesion seems entirely cystic on MRI. To minimize the risk of complications and additional surgical dissection, physicians should acknowledge that spinal tumors can migrate.
Conflict of interest statement
None.
Figures
Similar articles
-
Partially Cystic Lumbar Schwannoma with Atypical Histopathologic Features.World Neurosurg. 2020 Jun;138:440-443. doi: 10.1016/j.wneu.2020.03.131. Epub 2020 Apr 3. World Neurosurg. 2020. PMID: 32251817
-
Melanotic schwannoma of the L5 root.Neuroradiol J. 2016 Jun;29(3):219-21. doi: 10.1177/1971400916638359. Epub 2016 Mar 11. Neuroradiol J. 2016. PMID: 26969197 Free PMC article.
-
Totally cystic intradural extramedullary schwannoma.Turk Neurosurg. 2008 Oct;18(4):404-6. Turk Neurosurg. 2008. PMID: 19107689
-
A Mobile Schwannoma of the Cervical Spinal Cord: Case Report and Review of the Literature.Neurosurgery. 2016 Jan;78(1):E156-9. doi: 10.1227/NEU.0000000000000975. Neurosurgery. 2016. PMID: 26287552 Review.
-
Midline ventral intradural schwannoma of the cervical spinal cord resected via anterior corpectomy with reconstruction: technical case report and review of the literature.Neurosurgery. 2003 Jun;52(6):1482-5; discussion 1485-6. doi: 10.1227/01.neu.0000065182.16584.d0. Neurosurgery. 2003. PMID: 12762896 Review.
Cited by
-
Giant cystic Intradural extramedullary tumor of the lumbar spine mimicking arachnoid cyst: A case report.Int J Surg Case Rep. 2024 Dec;125:110535. doi: 10.1016/j.ijscr.2024.110535. Epub 2024 Oct 28. Int J Surg Case Rep. 2024. PMID: 39488070 Free PMC article.
-
Migratory schwannoma of the cauda equina with a change in radicular pattern: illustrative case.J Neurosurg Case Lessons. 2024 Apr 8;7(15):CASE23706. doi: 10.3171/CASE23706. Print 2024 Apr 8. J Neurosurg Case Lessons. 2024. PMID: 38588598 Free PMC article.
-
Mobile schwannoma of the lumbar spine: A case report and literature review.Medicine (Baltimore). 2023 Aug 25;102(34):e34966. doi: 10.1097/MD.0000000000034966. Medicine (Baltimore). 2023. PMID: 37653782 Free PMC article. Review.
-
Mobile thoracic intraspinal neurilemmoma.Acta Neurol Belg. 2023 Jun;123(3):1153-1154. doi: 10.1007/s13760-023-02253-7. Epub 2023 Apr 5. Acta Neurol Belg. 2023. PMID: 37016268 No abstract available.
-
Intradural cystic schwannomas of the spine: A case-based systematic review of an unusual tumor.Brain Spine. 2024 May 28;4:102843. doi: 10.1016/j.bas.2024.102843. eCollection 2024. Brain Spine. 2024. PMID: 38947985 Free PMC article. Review.
References
-
- Hollin SA, Drapkin AJ, Wancier J, Huang YP. Mobile schwannoma of the cauda equina. Case report. J Neurosurg. 1978;48(1):135–37. - PubMed
-
- Parmar H, Patkar D, Gadani S, Shah J. Cystic lumbar nerve sheath tumours: MRI features in five patients. Australas Radiol. 2001;45(2):123–27. - PubMed
-
- Marin-Sanabria EA, Sih IM, Tan KK, Tan JS. Mobile cauda equina schwannomas. Singapore Med J. 2007;48(2):e53–56. - PubMed
-
- Iizuka H, Iida T, Akai T. Mobile neurinoma of the cervicothoracic junction. Surg Neurol. 1998;50(5):492–93. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

