Ability of known susceptibility SNPs to predict colorectal cancer risk for persons with and without a family history
- PMID: 31209717
- PMCID: PMC6785388
- DOI: 10.1007/s10689-019-00136-6
Ability of known susceptibility SNPs to predict colorectal cancer risk for persons with and without a family history
Abstract
Before SNP-based risk can be incorporated in colorectal cancer (CRC) screening, the ability of these SNPs to estimate CRC risk for persons with and without a family history of CRC, and the screening implications need to be determined. We estimated the association with CRC of a 45 SNP-based risk using 1181 cases and 999 controls, and its correlation with CRC risk predicted from detailed family history. We estimated the predicted change in the distribution across predefined risk categories, and implications for recommended screening commencement age, from adding SNP-based risk to family history. The inter-quintile risk ratio for colorectal cancer risk of the SNP-based risk was 3.28 (95% CI 2.54-4.22). SNP-based and family history-based risks were not correlated (r = 0.02). For persons with no first-degree relatives with CRC, screening could commence 4 years earlier for women (5 years for men) in the highest quintile of SNP-based risk. For persons with two first-degree relatives with CRC, screening could commence 16 years earlier for men and women in the highest quintile, and 7 years earlier for the lowest quintile. This 45 SNP panel in conjunction with family history, can identify people who could benefit from earlier screening. Risk reclassification by 45 SNPs could inform targeted screening for CRC prevention, particularly in clinical genetics settings when mutations in high-risk genes cannot be identified. Yet to be determined is cost-effectiveness, resources requirements, community, patient and clinician acceptance, and feasibility with potentially ethical, legal and insurance implications.
Keywords: Colorectal cancer; Family history; Prediction model; Risk prediction; Single nucleotide polymorphism.
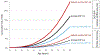
Figures

References
-
- Win AK, Ait Ouakrim D, Jenkins MA. Risk profiling: familial colorectal cancer. Cancer Forum 2014;38(1):15–25.
Publication types
MeSH terms
Grants and funding
- U24 CA074794/CA/NCI NIH HHS/United States
- U01 CA167551/CA/NCI NIH HHS/United States
- HHSN261201300021C/CA/NCI NIH HHS/United States
- U01 CA097735/CA/NCI NIH HHS/United States
- U01 CA 122839/NH/NIH HHS/United States
- U01 CA074783/CA/NCI NIH HHS/United States
- UM1 CA167551/NH/NIH HHS/United States
- HHSN261201000121C/CP/NCI NIH HHS/United States
- U19 CA148107/CA/NCI NIH HHS/United States
- U24 CA074783/CA/NCI NIH HHS/United States
- N01 CN067009/CN/NCI NIH HHS/United States
- R01 CA170122/CA/NCI NIH HHS/United States
- U24 CA097735/CA/NCI NIH HHS/United States
- U01 CA074794/CA/NCI NIH HHS/United States
- HHSN261201300011C/RC/CCR NIH HHS/United States
- HHSN261201300012I/CA/NCI NIH HHS/United States
- R01 CA143237/CA/NCI NIH HHS/United States
- N01 PC035142/CA/NCI NIH HHS/United States
- K05 CA152715/CA/NCI NIH HHS/United States
- UM1 CA167551/CA/NCI NIH HHS/United States
- U01 CA122839/CA/NCI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

