The role of polarisation of circulating tumour cells in cancer metastasis
- PMID: 31218452
- PMCID: PMC6744547
- DOI: 10.1007/s00018-019-03169-3
The role of polarisation of circulating tumour cells in cancer metastasis
Abstract
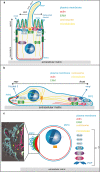
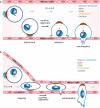
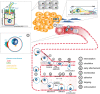
Metastasis is the spread of cancer cells from a primary tumour to a distant site of the body. Metastasising tumour cells have to survive and readjust to different environments, such as heterogeneous solid tissues and liquid phase in lymph- or blood circulation, which they achieve through a high degree of plasticity that renders them adaptable to varying conditions. One defining characteristic of the metastatic process is the transition of tumour cells between different polarised phenotypes, ranging from differentiated epithelial polarity to migratory front-rear polarity. Here, we review the polarisation types adopted by tumour cells during the metastatic process and describe the recently discovered single-cell polarity in liquid phase observed in circulating tumour cells. We propose that single-cell polarity constitutes a mode of polarisation of the cell cortex that is uncoupled from the intracellular polarisation machinery, which distinguishes single-cell polarity from other types of polarity identified so far. We discuss how single-cell polarity can contribute to tumour metastasis and the therapeutic potential of this new discovery.
Keywords: Actin; Adhesion; Attachment; CTC; Cancer; Single-cell polarity.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
Similar articles
-
Single cell polarity in liquid phase facilitates tumour metastasis.Nat Commun. 2018 Feb 28;9(1):887. doi: 10.1038/s41467-018-03139-6. Nat Commun. 2018. PMID: 29491397 Free PMC article.
-
Cell polarity in morphogenesis and metastasis.Philos Trans R Soc Lond B Biol Sci. 2013 Sep 23;368(1629):20130012. doi: 10.1098/rstb.2013.0012. Print 2013. Philos Trans R Soc Lond B Biol Sci. 2013. PMID: 24062582 Free PMC article. Review.
-
Epithelial cell polarity: a major gatekeeper against cancer?Cell Death Differ. 2011 Sep;18(9):1470-7. doi: 10.1038/cdd.2011.60. Epub 2011 May 27. Cell Death Differ. 2011. PMID: 21617693 Free PMC article. Review.
-
Cell polarity in motion: redefining mammary tissue organization through EMT and cell polarity transitions.J Mammary Gland Biol Neoplasia. 2010 Jun;15(2):149-68. doi: 10.1007/s10911-010-9180-2. Epub 2010 May 12. J Mammary Gland Biol Neoplasia. 2010. PMID: 20461450 Review.
-
Cell polarity signaling in the plasticity of cancer cell invasiveness.Oncotarget. 2016 May 3;7(18):25022-49. doi: 10.18632/oncotarget.7214. Oncotarget. 2016. PMID: 26872368 Free PMC article. Review.
Cited by
-
Detection of peripheral blood circulating tumor cells in oral squamous cell carcinoma and its clinical significance.Hua Xi Kou Qiang Yi Xue Za Zhi. 2021 Oct 1;39(5):591-597. doi: 10.7518/hxkq.2021.05.015. Hua Xi Kou Qiang Yi Xue Za Zhi. 2021. PMID: 34636209 Free PMC article. Chinese, English.
-
Ezrin Polarization as a Diagnostic Marker for Circulating Tumor Cells in Hepatocellular Carcinoma.Cells. 2024 Dec 25;14(1):6. doi: 10.3390/cells14010006. Cells. 2024. PMID: 39791707 Free PMC article.
-
Fibronectin in Cancer: Friend or Foe.Cells. 2019 Dec 20;9(1):27. doi: 10.3390/cells9010027. Cells. 2019. PMID: 31861892 Free PMC article. Review.
-
Cell polarity proteins promote macropinocytosis in response to metabolic stress.Nat Commun. 2024 Dec 3;15(1):10541. doi: 10.1038/s41467-024-54788-9. Nat Commun. 2024. PMID: 39627191 Free PMC article.
-
High Mobility Group Box 1 Promotes Lung Cancer Cell Migration and Motility via Regulation of Dynamin-Related Protein 1.Int J Mol Sci. 2021 Mar 31;22(7):3628. doi: 10.3390/ijms22073628. Int J Mol Sci. 2021. PMID: 33807275 Free PMC article.
References
-
- Chambers AF, Naumov GN, Varghese HJ, Nadkarni KV, MacDonald IC, Groom AC. Critical steps in hematogenous metastasis: an overview. Surg Oncol Clin N Am. 2001;10(243–255):vii. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

