Potential prognostic factors for predicting the chemotherapeutic outcomes and prognosis of patients with metastatic colorectal cancer
- PMID: 31218745
- PMCID: PMC6805281
- DOI: 10.1002/jcla.22958
Potential prognostic factors for predicting the chemotherapeutic outcomes and prognosis of patients with metastatic colorectal cancer
Abstract
Objectives: The purpose of this study was to explore whether pretreatment potential prognostic factors are related to chemotherapeutic outcomes and the prognosis of inpatients with metastatic colorectal cancer (mCRC) undergoing chemotherapy.
Materials and methods: Data from 71 patients with mCRC were analyzed retrospectively. The relationship between the potential prognostic factors before first-line chemotherapy and the clinicopathological characteristics and chemotherapy response of the patients was calculated using Fisher's exact test and the chi-square test. The prognostic factors were analyzed using univariate and multivariate analyses. We analyzed the subgroups using the Mann-Whitney U test.
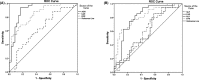
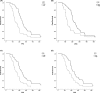
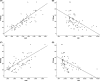
Results: Four factors were eventually used as prognostic factors, namely the albumin-to-globulin ratio (AGR), the fibrinogen-to-albumin ratio (FAR), the prealbumin-to-globulin ratio (PGR), and the fibrinogen-to-prealbumin ratio (FPR); the cutoff values of the four potential prognostic factors were 1.40, 10.63, 5.44, and 18.49, respectively. The high AGR and PGR groups had a higher response rate than that of the low groups. Patients in the low FAR and FPR groups showed a higher objective response rate than the high FAR and FPR groups. Patients with low FPR were associated with a higher disease control rate than patients with high FPR. Higher progression-free survival (PFS) was observed in the high AGR and PGR and low FAR and FPR groups. The AGR, FAR, PGR, and FPR were considered reliable prognostic factors for PFS in a univariate analysis.
Conclusions: The prechemotherapy AGR, FAR, PGR, and FPR were good prognostic factors to predict the chemotherapy response and PFS in patients with mCRC.
Keywords: FAR; PGR; chemotherapy response; colorectal cancer; prealbumin; prealbumin to globulin.
© 2019 The Authors. Journal of Clinical Laboratory Analysis Published by Wiley Periodicals, Inc.
Figures
Similar articles
-
Prealbumin-to-Globulin Ratio Can Predict the Chemotherapy Outcomes and Prognosis of Patients with Gastric Cancer Receiving First-Line Chemotherapy.J Immunol Res. 2020 Aug 5;2020:6813176. doi: 10.1155/2020/6813176. eCollection 2020. J Immunol Res. 2020. PMID: 32832571 Free PMC article.
-
The role of preoperative FPR and FAR in prognostic evaluation of stages II and III radical colorectal cancer: A single-center retrospective study.Medicine (Baltimore). 2024 May 17;103(20):e38145. doi: 10.1097/MD.0000000000038145. Medicine (Baltimore). 2024. PMID: 38758911 Free PMC article.
-
Prognostic Significance of Preoperative Fibrinogen-to-Prealbumin Ratio in Patients with Stage I-III Colorectal Cancer Undergoing Surgical Resection: A Retrospective Cohort Study.Biomed Res Int. 2021 Jan 12;2021:3905353. doi: 10.1155/2021/3905353. eCollection 2021. Biomed Res Int. 2021. PMID: 33521127 Free PMC article.
-
Albumin-fibrinogen ratio and fibrinogen-prealbumin ratio as promising prognostic markers for cancers: an updated meta-analysis.World J Surg Oncol. 2020 Jan 13;18(1):9. doi: 10.1186/s12957-020-1786-2. World J Surg Oncol. 2020. PMID: 31931816 Free PMC article. Review.
-
Pretreatment albumin to globulin ratio can serve as a prognostic marker in human cancers: a meta-analysis.Clin Chim Acta. 2018 Jan;476:81-91. doi: 10.1016/j.cca.2017.11.019. Epub 2017 Nov 21. Clin Chim Acta. 2018. PMID: 29170102 Review.
Cited by
-
Research Progress of Preoperative FPR, FAR or AFR in Patients with Colorectal Cancer.Cancer Manag Res. 2021 Feb 22;13:1791-1801. doi: 10.2147/CMAR.S292605. eCollection 2021. Cancer Manag Res. 2021. PMID: 33654428 Free PMC article. Review.
-
The prognostic value of sarcopenia combined with preoperative fibrinogen-albumin ratio in patients with intrahepatic cholangiocarcinoma after surgery: A multicenter, prospective study.Cancer Med. 2021 Jul;10(14):4768-4780. doi: 10.1002/cam4.4035. Epub 2021 Jun 8. Cancer Med. 2021. PMID: 34105304 Free PMC article.
-
Preoperative fibrinogen-to-albumin ratio, a potential prognostic factor for patients with stage IB-IIA cervical cancer.BMC Cancer. 2020 Jul 25;20(1):691. doi: 10.1186/s12885-020-07191-8. BMC Cancer. 2020. PMID: 32711484 Free PMC article.
-
Sodium to globulin ratio as a prognostic factor for patients with advanced gastric cancer.J Cancer. 2020 Oct 23;11(24):7320-7328. doi: 10.7150/jca.47314. eCollection 2020. J Cancer. 2020. PMID: 33193896 Free PMC article.
-
A nomogram of inflammatory indexes for preoperatively predicting the risk of lymph node metastasis in colorectal cancer.Tech Coloproctol. 2024 Nov 4;28(1):148. doi: 10.1007/s10151-024-03010-5. Tech Coloproctol. 2024. PMID: 39495392 Free PMC article.
References
-
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394‐424. - PubMed
-
- Zheng RS, Sun KX, Zhang SW, et al. Report of cancer epidemiology in China, 2015. Zhonghua zhong liu za zhi [Chin J Oncol]. 2019;41(1):19‐28. - PubMed
-
- Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144(5):646‐674. - PubMed
-
- Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet (London, England). 2001;357(9255):539‐545. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

