Antipsychotic drug use and risk of stroke and myocardial infarction: a systematic review and meta-analysis
- PMID: 31221107
- PMCID: PMC6585081
- DOI: 10.1186/s12888-019-2177-5
Antipsychotic drug use and risk of stroke and myocardial infarction: a systematic review and meta-analysis
Abstract
Background: The effect of antipsychotic (AP) drugs on risk of stroke and myocardial infarction (MI) remains unclear due to methodological limitations of, and inconsistencies across, existing studies. We aimed to systematically review studies reporting on the associations between AP drug use and stroke or MI risk, and to investigate whether associations differed among different sub-populations.
Methods: We searched Medline, EMBASE, PsychINFO and Cochrane Library (from inception to May 28, 2017) for observational studies reporting on AP drug use and MI or stroke occurrence. We performed random-effects meta-analyses for each outcome, performing sub-groups analyses by study population - specifically general population (i.e. those not restricted to patients with a particular indication for AP drug use), people with dementia only and psychiatric illness only. Where feasible we performed subgroup analyses by AP drug class.
Results: From 7008 articles, we included 29 relevant observational studies, 19 on stroke and 10 on MI. Results of cohort studies that included a general population indicated a more than two-fold increased risk of stroke, albeit with substantial heterogeneity (pooled HR 2.31, 95% CI 1.13, 4.74, I2 = 83.2%). However, the risk among patients with dementia was much lower, with no heterogeneity (pooled HR 1.16, 95% CI 1.00, 1.33, I2 = 0%) and there was no clear association among studies of psychiatric populations (pooled HR 1.44, 95% CI 0.90, 2.30; substantial heterogeneity [I2 = 78.8])). Associations generally persisted when stratifying by AP class, but few studies reported on first generation AP drugs. We found no association between AP drug use and MI risk (pooled HR for cohort studies: 1.29, 95% CI 0.88, 1.90 and case-control studies: 1.07, 95% CI 0.94, 1.23), but substantial methodological and statistical heterogeneity among a relatively small number of studies limits firm conclusions.
Conclusions: AP drug use may be associated with an increased risk of stroke, but there is no clear evidence that this risk is further elevated in patients with dementia. Further studies are need to clarify the effect of AP drug use on MI and stroke risk in different sub-populations and should control for confounding by indication and stratify by AP drug class.
Keywords: Antipsychotics; Dementia; Meta-analyses; Myocardial infarction; Stroke.
Conflict of interest statement
None.
Figures
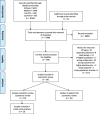


References
-
- Global Burden of Disease Study 2013 Collaborators Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the global burden of disease study 2013. Lancet. 2015;386(9995):743–800. doi: 10.1016/S0140-6736(15)60692-4. - DOI - PMC - PubMed
-
- Osborn DPJ, Levy G, Nazareth I, Petersen I, Islam A, King MB. Relative risk of cardiovascular and cancer mortality in people with severe mental illness from the United Kingdom’s general practice research database. Arch Gen Psychiatry. 2007;64(2):242–249. doi: 10.1001/archpsyc.64.2.242. - DOI - PubMed
-
- Correll CU, Solmi M, Veronese N, Bortolato B, Rosson S, Santonastaso P, Thapa-Chhetri N, Fornaro M, Gallicchio D, Collantoni E, Pigato G, Favaro A, Monaco F, Kohler C, Vancampfort D, Ward PB, Gaughran F, Carvalho AF, Stubbs B. Prevalence, incidence and mortality from cardiovascular disease in patients with pooled and specific severe mental illness: a large-scale meta-analysis of 3,211,768 patients and 113,383,368 controls. World Psychiatry. 2017;16(2):163–180. doi: 10.1002/wps.20420. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

