Setting fire to fat
- PMID: 31227622
- PMCID: PMC6597812
- DOI: 10.1074/jbc.H119.009488
Setting fire to fat
Erratum in
-
Correction: Setting fire to fat.J Biol Chem. 2019 Jul 26;294(30):11653. doi: 10.1074/jbc.AAC119.009988. J Biol Chem. 2019. PMID: 31350285 Free PMC article. No abstract available.
Abstract
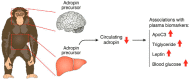
Adropin is a liver-secreted peptide that is crucial for metabolic health. However, the molecular functions and clinical significance of adropin have not been adequately explored. Butler et al. now investigate adropin expression profiles and links to cardiometabolic disease risk in two nonhuman primate models, increasing our translational and mechanistic understanding of this fascinating hormone.
© 2019 Zhang and Li.
Conflict of interest statement
The authors declare that they have no conflicts of interest with the contents of this article
Figures
Comment on
-
Low plasma adropin concentrations increase risks of weight gain and metabolic dysregulation in response to a high-sugar diet in male nonhuman primates.J Biol Chem. 2019 Jun 21;294(25):9706-9719. doi: 10.1074/jbc.RA119.007528. Epub 2019 Apr 15. J Biol Chem. 2019. PMID: 30988006 Free PMC article.
References
-
- Butler A. A., Zhang J., Price C. A., Stevens J. R., Graham J. L., Stanhope K. L., King S., Krauss R. M., Bremer A. A., and Havel P. J. (2019) Low plasma adropin concentrations increase risks of weight gain and metabolic dysregulation in response to a high-sugar diet in male nonhuman primates. J. Biol. Chem. 294, 9706–9719 10.1074/jbc.RA119.007528 - DOI - PMC - PubMed
-
- Kumar K. G., Trevaskis J. L., Lam D. D., Sutton G. M., Koza R. A., Chouljenko V. N., Kousoulas K. G., Rogers P. M., Kesterson R. A., Thearle M., Ferrante A. W. Jr., Mynatt R. L., Burris T. P., Dong J. Z., Halem H. A., et al. (2008) Identification of adropin as a secreted factor linking dietary macronutrient intake with energy homeostasis and lipid metabolism. Cell Metab. 8, 468–481 10.1016/j.cmet.2008.10.011 - DOI - PMC - PubMed
-
- Ghoshal S., Stevens J. R., Billon C., Girardet C., Sitaula S., Leon A. S., Rao D. C., Skinner J. S., Rankinen T., Bouchard C., Nuñez M. V., Stanhope K. L., Howatt D. A., Daugherty A., Zhang J., et al. (2018) Adropin: An endocrine link between the biological clock and cholesterol homeostasis. Mol. Metab. 8, 51–64 10.1016/j.molmet.2017.12.002 - DOI - PMC - PubMed
-
- Gao S., McMillan R. P., Jacas J., Zhu Q., Li X., Kumar G. K., Casals N., Hegardt F. G., Robbins P. D., Lopaschuk G. D., Hulver M. W., and Butler A. A. (2014) Regulation of substrate oxidation preferences in muscle by the peptide hormone adropin. Diabetes 63, 3242–3252 10.2337/db14-0388 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources