Licochalcone A inhibits cell proliferation, migration, and invasion through regulating the PI3K/AKT signaling pathway in oral squamous cell carcinoma
- PMID: 31239711
- PMCID: PMC6556467
- DOI: 10.2147/OTT.S201728
Licochalcone A inhibits cell proliferation, migration, and invasion through regulating the PI3K/AKT signaling pathway in oral squamous cell carcinoma
Abstract
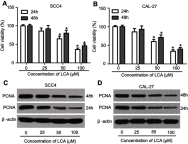
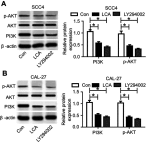
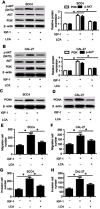
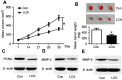
Background: Oral squamous cell carcinoma (OSCC) is one of the most common cancers, with high metastasis and mortality. Licochalcone A (LCA) is a chalconoid from the root of Glycyrrhiza inflata, which has anti-tumor, anti-inflammatory, anti-angiogenesis effects in many cancers. However, the mechanism that underlies LCA regulating cell proliferation, migration, and invasion in OSCC remains poorly understood. Methods: LY294002 or insulin-like growth factor 1 (IGF-1) were used to block or stimulate the phosphatidylinositol 3 kinase (PI3K)/protein kinase B (AKT) pathway in OSCC cells. Cell proliferation was investigated by MTT assay and proliferating cell nuclear antigen (PCNA) protein level using Western blot. The expression of metastasis-related protein was detected via Western blot. Cell migration and invasion abilities were evaluated by trans-well assay. A murine xenograft model of OSCC was established to investigate the anti-tumor effect of LCA in vivo. Results: Treatment of LCA inhibited cell proliferation in SCC4 and CAL-27 cells. Moreover, PI3K/AKT signaling was blocked by LY294002, and activated by IGF-1. LCA could suppress proliferation, migration, and invasion of OSCC cells, which was similar to the treatment of LY294002. In addition, LCA decreased IGF-1-induced OSCC progression. In a murine xenograft model, LCA treatment protected against tumor growth and metastasis in vivo. Conclusions: LCA might inhibit cell proliferation, migration, and invasion through regulating the PI3K/AKT pathway in OSCC, developing a potential chemotherapeutic agent for OSCC.
Keywords: Licochalcone A; PCNA; PI3K/AKT; invasion; migration; oral squamous cell carcinoma.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures

Similar articles
-
Anticancer effects of licochalcones: A review of the mechanisms.Front Pharmacol. 2023 Jan 23;14:1074506. doi: 10.3389/fphar.2023.1074506. eCollection 2023. Front Pharmacol. 2023. PMID: 36755942 Free PMC article.
-
[Effect of licochalcone A on autophagy in renal cell carcinoma via PI3K/Akt/mTOR signaling pathway].Zhongguo Zhong Yao Za Zhi. 2018 Sep;43(17):3545-3552. doi: 10.19540/j.cnki.cjcmm.20180427.001. Zhongguo Zhong Yao Za Zhi. 2018. PMID: 30347925 Chinese.
-
Alkannin restrains oral squamous carcinoma cell growth, migration and invasion by regulating microRNA-9/RECK axis.Artif Cells Nanomed Biotechnol. 2019 Dec;47(1):3153-3162. doi: 10.1080/21691401.2019.1642206. Artif Cells Nanomed Biotechnol. 2019. PMID: 31349748
-
[Licochalcone A induces cell cycle arrest in human lung squamous carcinoma cells via the PI3K/Akt signaling pathway].Nan Fang Yi Ke Da Xue Xue Bao. 2023 Jan 20;43(1):111-116. doi: 10.12122/j.issn.1673-4254.2023.01.15. Nan Fang Yi Ke Da Xue Xue Bao. 2023. PMID: 36856218 Free PMC article. Chinese.
-
Local Anesthetic Lidocaine and Cancer: Insight Into Tumor Progression and Recurrence.Front Oncol. 2021 Jun 24;11:669746. doi: 10.3389/fonc.2021.669746. eCollection 2021. Front Oncol. 2021. PMID: 34249706 Free PMC article. Review.
Cited by
-
Epigenetic Regulation in Oral Squamous Cell Carcinoma Microenvironment: A Comprehensive Review.Cancers (Basel). 2023 Nov 27;15(23):5600. doi: 10.3390/cancers15235600. Cancers (Basel). 2023. PMID: 38067304 Free PMC article. Review.
-
Tanshinone IIA inhibits proliferation and migration by downregulation of the PI3K/Akt pathway in small cell lung cancer cells.BMC Complement Med Ther. 2024 Jan 31;24(1):68. doi: 10.1186/s12906-024-04363-y. BMC Complement Med Ther. 2024. PMID: 38297301 Free PMC article.
-
Anticancer effects of licochalcones: A review of the mechanisms.Front Pharmacol. 2023 Jan 23;14:1074506. doi: 10.3389/fphar.2023.1074506. eCollection 2023. Front Pharmacol. 2023. PMID: 36755942 Free PMC article.
-
Licochalcone A Promotes the Ubiquitination of c-Met to Abrogate Gefitinib Resistance.Biomed Res Int. 2022 Mar 10;2022:5687832. doi: 10.1155/2022/5687832. eCollection 2022. Biomed Res Int. 2022. PMID: 35309168 Free PMC article.
-
Amalgamated Pharmacoinformatics Study to Investigate the Mechanism of Xiao Jianzhong Tang against Chronic Atrophic Gastritis.Curr Comput Aided Drug Des. 2024;20(5):598-615. doi: 10.2174/1573409919666230720141115. Curr Comput Aided Drug Des. 2024. PMID: 37475552
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

