Clinical experience of full custom-made artificial bones for the maxillofacial region
- PMID: 31245504
- PMCID: PMC6581837
- DOI: 10.1016/j.reth.2016.08.004
Clinical experience of full custom-made artificial bones for the maxillofacial region
Abstract
Introduction: Autologous, allogeneic, and artificial bones are clinically applied as graft materials for bone reconstruction, with each having their own advantages and disadvantages. Although artificial bones with various shapes are currently available, a product with a morphology that may be freely modified by operators has not yet been developed. In the present study, we developed a full custom-made artificial bone, and applied it to form the maxillofacial region. We herein report treatment outcomes.
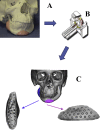
Methods: An artificial bone was prepared on a 3-dimensional solid model, and data of its shape was collected on CT. A full custom-made artificial bone was prepared by laminating α-tricalcium phosphate powder using an aqueous polysaccharide curing solution and the ink-jet powder-laminating device, Z406 3D Printer (DICO, USA). Subjects comprised patients who underwent maxillofacial plasty using this artificial bone between March 2006 and September 2009.
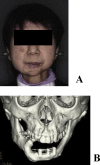
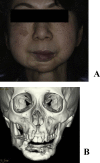
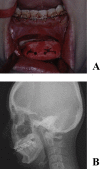
Results: Maxillofacial plasty using the full custom-made artificial bone was applied to 23 regions in 20 patients (14 females and 6 males). The recipient region was the maxilla in 3, mandibular ramus in 13, mental region in 7, and frontal bone in 1. Postoperative courses were favorable in 18 out of the 23 regions; however, the fit was insufficient in 2 regions and the recipient regions were exposed within 1 year after surgery. Three regions were exposed 1 year or more after surgery.
Conclusion: We developed a novel reconstruction method using a full custom-made artificial bone. Its fit with the recipient bone was considered to be important, since an ill fit between the recipient and artificial bones potentially resulting in the artificial bone being detached. Therefore, fixation is important in order to prevent the detachment, and careful course observations are required when an ill fit is concerned during the follow-up period.
Keywords: Artificial bones; Complication; Full custom-made; Oral-maxillofacial region.
Figures






Similar articles
-
Computed tomographic evaluation of novel custom-made artificial bones, "CT-bone", applied for maxillofacial reconstruction.Regen Ther. 2016 Jul 1;5:1-8. doi: 10.1016/j.reth.2016.05.002. eCollection 2016 Dec. Regen Ther. 2016. PMID: 31245494 Free PMC article.
-
Maxillofacial reconstruction using custom-made artificial bones fabricated by inkjet printing technology.J Artif Organs. 2009;12(3):200-5. doi: 10.1007/s10047-009-0462-7. Epub 2009 Sep 19. J Artif Organs. 2009. PMID: 19894095
-
Bone Regenerative Medicine in Oral and Maxillofacial Region Using a Three-Dimensional Printer<sup/>Tissue Eng Part A. 2017 Jun;23(11-12):515-521. doi: 10.1089/ten.TEA.2016.0543. Epub 2017 Apr 25. Tissue Eng Part A. 2017. PMID: 28351222 Review.
-
Horizontal ridge reconstruction of the anterior maxilla using customized allogeneic bone blocks with a minimally invasive technique - a case series.BMC Oral Health. 2017 Dec 8;17(1):146. doi: 10.1186/s12903-017-0423-0. BMC Oral Health. 2017. PMID: 29216869 Free PMC article.
-
Clinical application of artificial bone in the maxillofacial region.J Artif Organs. 2008;11(4):171-6. doi: 10.1007/s10047-008-0425-4. Epub 2008 Dec 17. J Artif Organs. 2008. PMID: 19184280 Review.
Cited by
-
Additive Manufacturing of Material Scaffolds for Bone Regeneration: Toward Application in the Clinics.Adv Funct Mater. 2020 Oct 15;31(5):2006967. doi: 10.1002/adfm.202006967. eCollection 2021 Jan 27. Adv Funct Mater. 2020. PMID: 33531885 Free PMC article.
-
Additive Manufacturing for Guided Bone Regeneration: A Perspective for Alveolar Ridge Augmentation.Int J Mol Sci. 2018 Oct 24;19(11):3308. doi: 10.3390/ijms19113308. Int J Mol Sci. 2018. PMID: 30355988 Free PMC article. Review.
-
Scalable production of homogeneous cardiac organoids derived from human pluripotent stem cells.Cell Rep Methods. 2023 Dec 18;3(12):100666. doi: 10.1016/j.crmeth.2023.100666. Cell Rep Methods. 2023. PMID: 38113855 Free PMC article.
References
-
- Tessier P., Kawamoto H., Matthews D., Posnick J., Raulo Y., Tulasne J.F. Autogenous bone grafts and bone substitutes – tools and techniques: I. A 20,000-case experience in maxillofacial and craniofacial surgery. Plast Reconstr Surg. 2005;116:6S–24S. - PubMed
-
- Eppley B.L., Pietrzak W.S., Blanton M.W. Allograft and alloplastic bone substitutes: a review of science and technology for the craniomaxillofacial surgeon. J Craniofac Surg. 2005;16:981–989. - PubMed
-
- Fischer-Brandies E., Dielert E. Clinical use of tricalciumphosphate and hydroxyapatite in maxillofacial surgery. J Oral Implantol. 1985;12:40–44. - PubMed
-
- Nishiyama T., Nakajima T., Yoshimura Y., Nakanishi Y. Utilizing solid model for preoperative shaping of HAP-TCP ceramic bone substitute: application for craniomaxillofacial surgery. Eur J Plast Surg. 1994;17:173–177.
-
- Eppley B.L. Craniofacial reconstruction with computer-generated HTR patient-matched implants use in primary bone tumor excision. J Craniofac Surg. 2002;13:650–657. - PubMed
LinkOut - more resources
Full Text Sources

